Introduction
Our aims were to assess the perceptions of orthodontic case complexity among orthodontists, general dentists, orthodontic residents, and dental students and to compare their perceptions with the American Board of Orthodontics Discrepancy Index (DI).
Methods
Orthodontists, general dentists, orthodontic residents, and dental students (n = 343) participated in a Web-based survey. Pretreatment orthodontic records of 29 cases with varying DI scores were obtained. Respondents were asked to evaluate case complexity on a 100-point visual analog scale. Additional information was collected on participants’ orthodontic education and orthodontic treatment preferences. Pearson correlation coefficients were used to assess the relationship between the average complexity score and the DI score. Repeated measures analysis with linear mixed models was used to assess the association between the average complexity score and the DI score and whether the association between the 2 scores varied by level of difficulty or panel group. The level of significance for all analyses was set at P <0.05.
Results
The results showed that 71.6% of general dentists provided some orthodontic services, with 21.0% providing full fixed appliances and 38.3% providing clear aligners. DI score was significantly associated with complexity perceptions ( P = 0.0168). Associations between average complexity and DI score varied significantly by provider group ( P = 0.0033), with orthodontists and residents showing the strongest associations. When the DI score was greater than 15, orthodontists and residents perceived cases as more complex than did the other provider groups.
Conclusions
Orthodontists and orthodontic residents had better judgments for evaluating orthodontic case complexity. The high correlation between orthodontic professionals’ perceptions and DI scores suggested that additional orthodontic education and training have an influence on the ability to recognize case complexity.
Highlights
- •
Cases with mild complexity are easily identified regardless of experience level.
- •
Experience in orthodontics affects the ability to recognize case complexity.
- •
Discrepancy Index scores should not be grouped and should be used individually.
The necessity to treat dental and skeletal imbalances with orthodontic therapy can objectively be measured using different occlusal indexes. Whereas the Dental Aesthetics Index and the Index of Complexity, Outcome and Need are popular ones, the Discrepancy Index (DI) developed by the directors of the American Board of Orthodontics (ABO) has primarily been used in the United States. Orthodontists receive 2 to 3 years of additional training and education in diagnosis and correction of dental malocclusions and jaw discrepancies. However, general dentists receive limited training in orthodontic diagnosis and treatment in dental school. Therefore, individual assessment of the orthodontic treatment need can be quite subjective and may vary depending on expertise and level of dental specialty education.
Studies have shown that general dentists are providing 20% to 50% of all orthodontic treatment. Although some general dentists have pursued additional orthodontic instruction via continuing education courses, their overall ability to provide proficient comprehensive treatment remains controversial. The literature reports that although there is a high level of agreement of orthodontic treatment need among general dentists and orthodontists, orthodontists spend less time on treatment and achieve better results. However, the general public may be unaware of these substantial discrepancies between provider types and other valuable information that could influence their decision of where to seek care. This may result in incomplete care and eventually lead to retreatment of the same patient. According to Ren et al, patients seeking orthodontic retreatment have good perceptions of dental esthetics, strong motivations, and objective treatment needs. All of these factors have a strong impact on the treatment demand. Therefore, orthodontic treatment providers should be fully competent in their assessments.
Analyzing all clinical records of a case and interpreting the findings to aid in proper diagnosis is a major predictor of treatment success. Successful orthodontic treatment is highly correlated with a correct diagnosis and proper execution of an accurate treatment plan. Using patient records and evaluations, attempts were made to investigate the relationship between orthodontic treatment complexity and perceptions of orthodontists with other indexes. However, use of the DI in this regard has been limited.
The purpose of this study was to assess the possible relationships between perceived orthodontic treatment complexity and the DI in a panel group comprising orthodontists, general dentists, orthodontic residents, and dental students.
Material and methods
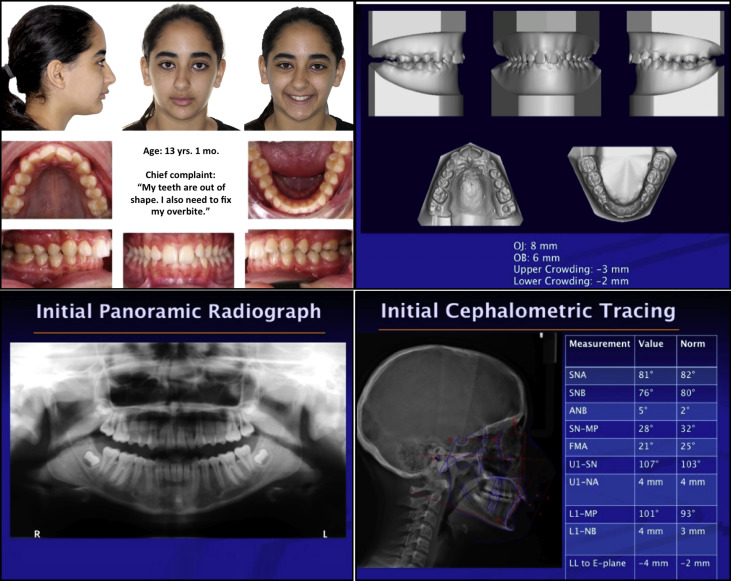
Approval for the study was granted by the Institutional Review Board of the University of Texas Health Sciences Center at Houston (HSC-DB-15-0486). Pretreatment orthodontic records of 146 patients aged between 11 and 21 years and treated between 2012 and 2015 at the University of Texas School of Dentistry were examined. All had permanent dentition and were treated with nonsurgical comprehensive orthodontic appliances. Patients with craniofacial anomalies, incomplete records, and previous orthodontic treatment were excluded from the study. Additionally, 2 authors (E.M.H., S.A.) were calibrated on the calculation of DI scores. They scored the cases independently in private sessions. Cases that did not have an absolute match of 2 independent investigators’ DI scores were also eliminated from the study. A total of 29 cases were included and examined in 3 groups: 10 mild cases (DI, 0-10), 9 moderate cases (DI, 11-20), and 10 complex cases (DI, >20). Pretreatment records including extraoral and intraoral photos, panoramic radiographs, traced cephalometric radiographs with ABO analysis values, and digital models of the patients were used in the assessments ( Fig 1 ).
A Web-based survey was sent to 1661 dental professionals, including orthodontists, general dentists, orthodontic residents, and dental students using eSurvey (enuvo, Zürich, Switzerland). An e-mail reminder was sent to those who had not already participated 4 weeks after the initial e-mail was sent. Of the 1661 participants who were sent a survey link, 392 participants attempted to start the survey, but results were only obtained from 343 participants (58.9% male, 41.1% female) who completed the survey in its entirety for a total response rate of 20.7%. Panel members were grouped as orthodontists (26 female, 33 male; n = 59; 17.2%), general dentists (38 female, 43 male; n = 81; 23.6%), orthodontic residents (14 female, 19 male; n = 33; 9.6%), and senior dental students (87 female, 83 male; n = 170; 49.6%). Average ages for the orthodontist, general dentist, orthodontic resident, and dental student groups were 48.2 ± 6, 46.0 ± 5, 28.9 ± 3, and 26.3 ± 3 years, respectively.
Demographic information including age, sex, and number of years in the dental field was recorded. Information about the provider’s use of orthodontic appliances and where they received most of their orthodontic knowledge was obtained from the panel members. Panel members also provided a rating of the adequacy of the orthodontic education they received during their undergraduate dental education. Lastly, the panel members were shown a complete set of pretreatment orthodontic records of the 29 patients in random order and were asked to determine subjective case complexity using a computer-generated 100-mm visual analog scale ranging from 0 mm (simple) to 100 mm (difficult). Four of the 29 cases were repeated in the survey to assess intrarater repeatability.
Results were analyzed using SPSS for Windows software (version 22; IBM, Armonk, NY). The relationship between the perceived complexity score and the 29 cases and the differences in complexity scores across the provider groups were assessed using repeated measures analysis of variance (ANOVA). Repeatability of the panel participants was evaluated with the Cohen kappa using a nominal conversion of the case complexity scores. The Pearson correlation coefficient was used to assess the overall correlation of the average complexity score and the DI score. We also used repeated measures ANOVA with linear mixed models to assess the association between the average complexity score and the DI score, and whether the association between the 2 scores varied by level of difficulty or provider group. The level of significance for all analyses was set at P <0.05.
Results
The results showed that 240 participants (70%) had been in the dental field for 0 to 5 years, 18 (5.2%) for 5 to 10 years, 17 (5.0%) for 10 to 20 years, 20 (5.8%) 20 to 30 years, and 48 (14.0%) for more than 30 years ( Table I ). Of the 59 orthodontists surveyed, 79.7% were board certified by the ABO.
| Group | 0-5 years | 5-10 years | 10-20 years | 20-30 years | >30 years |
|---|---|---|---|---|---|
| Orthodontists (n = 59) | 15, 25.4% | 7, 11.9% | 9, 15.3% | 6, 10.2% | 22, 37.3% |
| General dentists (n = 81) | 27, 33.3% | 7, 8.6% | 7, 8.6% | 14, 17.3% | 26, 32.1% |
| Orthodontic residents (n = 33) | 30, 90.9% | 3, 9.1% | – | – | – |
| Dental students (n = 170) | 168, 98.8% | 1, 0.6% | 1, 0.6% | – | – |
| Total (n = 343) | 240, 70.0% | 18, 5.2% | 17, 5.0% | 20, 5.8% | 48, 14.0% |
Concerning orthodontic appliance use, the orthodontic residents used all appliances at a higher percentage rate than did any other provider group ( Table II ). Overall, orthodontists and orthodontic residents reported using a wider variety of appliances than did general dentists and dental students. All orthodontic residents used clear aligners, compared with 89.8% of orthodontists and 38.3% of general dentists. Among the general dentists, 21% reported using full fixed appliances, and 28.4% used no orthodontic appliances in their practice. Among the dental students, 34.1% reported using space maintainers, whereas the majority (58.8%) of the dental students did not report using any orthodontic appliances in dental school.
| Orthodontists | Residents | General dentists | Dental students | |
|---|---|---|---|---|
| Space maintainers | 98.3 | 100 | 58 | 34.1 |
| Sectional appliances | 96.6 | 97 | 9.9 | 1.2 |
| Full fixed appliances | 100 | 100 | 21 | 2.9 |
| Palatal expanders | 100 | 100 | 21 | 1.8 |
| Functional appliances | 79.7 | 100 | 23.5 | 0.6 |
| Extraoral appliances | 64.4 | 69.7 | 3.7 | 0 |
| Clear aligners | 89.8 | 100 | 38.3 | 1.8 |
| None | 0 | 0 | 28.4 | 58.8 |
| Other | 6.8 | 3 | 4.9 | 12.9 |
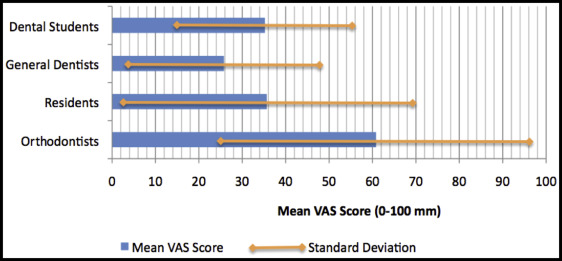
Survey participants were also asked to rate the adequacy of their orthodontic undergraduate education in dental school on a 100-mm visual analog scale from “poor” to “excellent” ( Fig 2 ). Orthodontists rated their orthodontic undergraduate education the highest, with a mean score of 60.8 ± 36.5. Residents and dental students had similar ratings with means of 35.6 ± 34.0 and 35.2 ± 20.6, respectively. General dentists gave the lowest adequacy rating with a mean of 25.7 ± 22.9.