Pain and anxiety control
Learning Outcomes
At the end of this chapter you should have an understanding of:
- 1. Why pain and anxiety control is important.
- 2. The different methods of pain and anxiety control used.
Introduction
Managing patients’ pain and anxiety control commences at the assessment stage of an appointment where the clinician undertakes a medical, dental and social history. The three histories are equally important as this gives the clinician an understanding of the patient’s anxiety levels, preferences, any medical conditions and/or medications taken. From this information the clinician can correctly plan a patient’s treatment taking into account these factors so that the patient will be safely treated in the dental surgery, along with their pain relief being individualised for them.
In their Maintaining Standards booklet, the General Dental Council have outlined a logical progression for pain and anxiety control stating that the mainstay/starting point of managing a patient’s pain relief is by using a local anaesthetic.
To appreciate pain and anxiety control methods used, it is important to understand the nerve supply to the maxilla and mandible along with their surrounding structures as discussed in Chapter 2, as well as the following terminology used:
- • Analgesia: the absence of pain without loss of consciousness.
- • Anaesthesia: loss of all sensations, including pain, with or without loss of consciousness.
- • Anaesthetic: an agent which produces anaesthesia.
- • General anaesthesia: the loss of sensation produced by putting a patient to sleep, thereby preventing reception of pain by the brain.
- • Local anaesthesia: the loss of feeling or sensation in some part of the body due to nerve impulse blockage, by use of drugs preventing conduction of stimuli along a nerve.
- • Conscious sedation: the administration of sedatives or dissociative agents with or without a local anaesthetic to help the patient accept dental treatment. At all times the patient remains conscious.
If a patient does not receive enough pain relief when undertaking maxillofacial surgery procedures they will be uncomfortable as they will experience pain. This could lead to an uncooperative patient which could have a detrimental effect on their oral health care as they may not attend the dentist in the future due to the experience.
Local Anaesthetic
A local anaesthetic is administered when any procedure involves soft tissues, enabling a patient to endure the dental treatment due to being pain free. Pressure and vibrations can still be felt and quite often these sensations are interpreted by the patient as pain; good patient management is therefore important. By providing the patient with a local anaesthetic the area administered will be numb, making it insensitive to pain without affecting their other senses. On occasions a clinician may apply a topical anaesthetic gel (Figure 3.1) to slightly de-sensitise the area being injected, thereby making the administration of the local anaesthetic more comfortable for the patient. Clinicians must appreciate the concentration and effects of the local anaesthetic they are administering to avoid reaching the maximum toxic dose. This will naturally vary from patient to patient depending upon their weight. For example, if septocaine (commonly referred to as articaine; Figure 3.1) was being administered and the patient weighed 70 kg, the maximum amount of cartridges that could be administered is 7.

Figure 3.1 Topical anaesthetic gel and anaesthetic cartridges: articaine 4% solution with epinephrine 1:100,000 lignocaine (xylocaine) 2% and adrenaline 1 in 80,000; and prilocaine (citanest) 3% and octopressin (felypressin).
How local anaesthetics work
Painful sensations from dental structures are directed to the brain along specific nerve pathways, where they are interpreted as pain. An administration of a local anaesthetic around any of these nerves or their branches temporarily prevents them from conveying painful messages to the brain. As previously explained however, pressure and vibrations can still be felt. After a while the effect of the local anaesthetic will wear off and the nerve impulses return to normal. A dental injection will be administered into an area which is richly supplied with blood vessels. This means that the local anaesthetic solution is rapidly absorbed into the blood stream. Due to the rapidity in which anaesthetic agents are removed from the injected area, plain anaesthetic such as lignocaine (xylocaine) (Figure 3.1) will not last long enough for most dental procedures; to overcome this, a vasoconstrictor is added to the solution to prolong the duration of action.
Vasoconstrictors
A vasoconstrictor will produce vasoconstriction of the vessels in the area where the local anaesthetic has been administered, thereby reducing the blood flow to prolong anaesthesia. They also reduce bleeding, which is a useful function during maxillofacial surgery due to these being bloodletting procedures. There are two types of vasoconstrictors used:
- • Adrenaline: This vasoconstrictor is naturally occurring in the body, but is not suitable for all patients as it can affect the heart rate and blood pressure.
- • Octopressin: This vasoconstrictor is not suitable for pregnant patients as it has the ability to mimic the hormone oxytosin which stimulates the uterus during labour; if administered, it could result in premature labour.
It must be remembered that the choice of local anaesthetic to be used which contains a vasoconstrictor would be the responsibility of the treating clinician for each patient.
Equipment required to administer a local anaesthetic
The following equipment is required to administer a local anaesthetic:
- • A sterile self-aspirating syringe (Figure 3.2): This type of syringe is used to avoid the anaesthetic being injected into a blood vessel. If, upon administration, blood flowed into the cartridge the clinician should stop administration and reposition the needle until the blood disappeared.
- • A sterile disposable needle: Either a gauge 27 (long) (Figure 3.2) or gauge 30 or 31 (short and shorter) (Figure 3.2) depending upon the clinician’s choice and the site of the injection.
- • The local anaesthetic cartridge chosen by the clinician.
- • A topical anaesthetic and cotton wool roll for application if the clinician chooses.
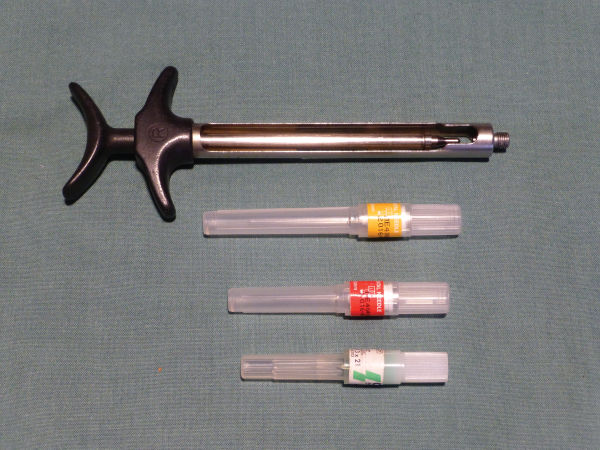
Figure 3.2 Sterile self-aspirating syringe and sterile disposable needle: gauges 27 (long), 30 and 31 (short and shorter).
Topical anaesthetic
Topical anaesthetics are applied to the appropriate area for a few minutes prior to an injection being administered to relieve discomfort. They take about 2 minutes to work and last for approximately 10 minutes. They are available as a gel or spray for dental use and commonly contain an anaesthetic agent such as lidocaine or benzocaine. Some clinicians may choose to use a flavoured topical gel, which is more easily tolerated by children.
Local anaesthetic presentation
The local anaesthetic agent/solution is supplied in glass cartridges which have a rubber diaphragm at one end and a rubber bung at the other. Each cartridge contains either 1.8 mL or 2.2 mL of injectable solution in order for them to fit into different size syringes.
Checks before preparing local anaesthetics for patients
It is important to look at the patient’s medical history to establish if there were any complications the last time he/she received a local anaesthetic. By undertaking this, the dental team can be prepared for any manifestation of an emergency. The local anaesthetic syringe should be inspected to ensure that it is sterile and moves smoothly when pressed. The local anaesthetic cartridge itself should be checked to ensure the expiry date has not been reached, the solution is intact and not cloudy or discoloured, and the bungs have not been tampered with. The disposable needle to be assembled onto the self-aspirating syringe should be inspected to ensure it is the correct size for the type of injection being administered and that it is intact. The batch number and expiry date should be written in the patient’s notes.
Types of local anaesthetic syringes
- • Self-aspirating syringe (Figure 3.1): These are used to avoid the anaesthetic being injected into a blood vessel. If blood flowed into the cartridge, the clinician should stop the administration, reposition the needle and continue to inject the local anaesthetic solution into the chosen area until the blood disappeared.
- • Ligmaject/peripress (Figure 3.3): This is a gun-shaped syringe that injects small amounts of anaesthetic under high pressure. A very short needle is used in conjunction with it to introduce/force the anaesthetic solution between the tooth and the bone into the periodontal ligaments.
- • Ultra-safety-plus disposable sterile syringe (Figure 3.4): These sterile injectable systems are single-patient-use only. They have an integral protective sheath needlestick injury-prevention device.

Figure 3.3 Ligmaject/peripress.
Source: Hollins, C. 2013 Levison’s Textbook for Dental Nurses, 11th edition, p. 394. Reproduced with permission of John Wiley & Sons.

Figure 3.4 Ultra-safety-plus disposable sterile syringe.
Types of local anaesthetic
- • Lignocaine (xylocaine) 2% and adrenaline 1 in 80,000. The half-life in the body is approximately 1.5–2 hours.
- • Prilocaine (citanest) 3% and octopressin (felypressin) (Figure 3.1). The half-life of prilocaine is approximately 1–1.5 hours.
- • Prilocaine 4% plain which is rapidly taken up into the system and will therefore not provide pain relief for long maxillofacial procedures or those where post-operative numbness will be beneficial.
- • Articaine 4% solution with epinephrine 1:100,000 or 1:200,000. Articaine is also known as septocaine and is one of the most widely used local anaesthetic agents in many European countries. It has a half-life of approximately 20 minutes.
Typical contents of a local anaesthetic cartridge
- • Anaesthetic agent.
- • Vasoconstrictor.
- • Reducing agent (sodium metabisulphate), which prevents oxidisation of the anaesthetic solution resulting in discolouration.
- • Fungicide (thymol) which prevents clouding.
- • Sterile water.
Complications that can occur during and after the administration of a local anaesthetic
When a local anaesthetic is administered complications can occur, such as:
- • The patient could experience a medical emergency with the most common being a faint, especially when an inferior dental block has been given. This could be attributed to some of the local anaesthetic being accidently injected into a blood vessel, the patient being sat upright during the administration of the local anaesthetic, the patient feeling nervous, lack of food or too much clothing being worn.
- • The needle could break during administration of a local anaesthetic.
- • The patient could experience an allergic reaction to the local anaesthetic used.
- • A blood vessel could be accidentally nicked and a haematoma or ‘blood blister’ could occur. This would eventually heal.
- • If the needle is positioned too posteriorly during the administration of an inferior dental block (Figure 3.5), anaesthetic may penetrate the parotid gland causing transient facial paralysis. This would affect the facial nerve or the VIIth cranial nerve. As the patient will experience a temporary loss of their facial muscles, they would not be able to close their eyelid. If the needle is positioned too medially the medial pterygoid muscle can be injected, resulting in trismus (limited mouth opening).
- • Nerve damage can occur during an injection. If this occurs the patient will experience paresthesia (numbness) which can take weeks or even months to return to normal; on occasions, the patient is left with permanent nerve damage.
- • Following the procedure the patient could accidently self-inflict trauma by either biting their lip, tongue or sustaining a thermal burn caused by drinking hot fluids. This commonly occurs in children or those with learning difficulties.
- • The clinician or dental nurses could accidently sustain a needlestick injury. One could also occur by not following protocol when dealing with sharps.

Figure 3.5 Inferior dental block technique.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


