Chapter 5
Oral Mucosal Microbes
Abstract
This chapter describes the cell and colony morphology, cultural and biochemical characteristics of oral microbes that are mainly isolated from oral mucosal plaques, including bacteria of the genera Staphylococcus, Streptococcus, Escherichia, Haemophilus, Moraxella, and Neisseria, as well as several representative Mycoplasma, fungi, and viruses.
Keywords
Candida; Escherichia; Haemophilus; Herpes simplex virus; Moraxella; Mucosal; Mycoplasma; Neisseria; Staphylococcus; Streptococcus
5.1. Gram-Positive Bacteria
5.1.1. Staphylococcus
5.1.1.1. Staphylococcus aureus
S. aureus is a gram-positive species of bacteria. Its peptidoglycan structure is L-Lys-Gly5-6 and the cell wall teichoic acid is formed by ribitol polymerization. Cellular morphology is shown in Figure 5.1(A) and (B). The genomic GC content is 32–36% and the type strains are ATCC126000, NCTC8352, and CCM885.
S. aureus is a facultative anaerobe but also grows well under aerobic conditions (Figure 5.1(C), (D), and (E)). After incubation on semisolid thioglycollate medium, colonies grow rapidly and are uniform and dense. The final pH of glucose broth incubated with S. aureus is always between pH 4.3 and 4.6.
S. aureus is associated with human infections, such as facial furuncle and carbuncle, loose connective tissue inflammation, and tumor postoperative wound infections.
S. aureus is able to produce golden pigments on common agar plate. The colonies are round, raised, shiny opaque, and have a smooth surface and a whole edge. The diameter is 2–3 mm. A β-transparent hemolytic zone surrounds the colony when S. aureus is incubated on blood BHI agar.
5.1.2. Streptococcus
5.1.2.1. Streptococcus mitis
S. mitis cells are gram-positive and spherical or elliptical in shape (about 0.6–0.8 μm in diameter). They can form long chains in broth culture (Figure 5.2(A)). The GC content of the S. mitis genome is 38–39%, and its type strain is NCTC3165.
Streptococcus mitis cells grow variably at 45 °C, and the final pH value of a culture in glucose broth is around pH 4.2–5.8. Cells in broth culture change from rough to smooth following subculture, and cells that are grown under aerobic conditions can be smooth or rough. TPY agar is the common medium on which S. mitis is grown (Figure 5.2(B)). Significant α-hemolytic reaction can be observed when S. mitis is grown on blood agar plates (Figure 5.2(C)). S. mitis forms small broken-glass-like colonies on sucrose agar plates, and very few strains can form the typical sticky colonies. Colonies observed by stereomicroscope are shown in Figure 5.2(D).
Biochemical reactions. S. mitis can ferment glucose, maltose, sucrose, lactose, and salicin to produce acid, and some strains can also ferment raffinose and trehalose to produce acid. However, inulin, mannitol, sorbitol, glycerol, arabinose, and xylose cannot be fermented by S. mitis.
Colonization characteristics. S. mitis can be detected in human saliva, oral mucosa, sputum, or excrement. It is a common oral Streptococcus and a member of the oral microflora.
5.1.2.2. Streptococcus pyogenes
S. pyogenes belongs to Lancefield group A and is gram-positive (Figure 5.3(A)). Cells of this species have a diameter of 0.5–1.0 μm and are usually spherical. However, cells from old cultures may be oval. Moreover, S. pyogenes cells are often arranged in short, medium, or long chains, but most cells in broth culture form long chains. Cells of clinical isolates are usually arranged in pairs. S. pyogenes cells observed by stereomicroscope are shown in Figure 5.3(B). The GC content of the S. pyogenes genome is 34.5–38.5% (Tm method), and its type strain is ATCC12344.
S. pyogenes is a facultative anaerobe, and the optimal temperature for growth is 37 °C. A nutrient-rich medium is required for S. pyogenes growth, and both blood and serum can promote its growth. Colonies growing on MS agar are shown in Figure 5.3(C). Cells from overnight blood agar plate culture have three different colony types: (1) colonies with β-hemolytic zone; (2) mucoid colonies; (3) lackluster colonies. In fact, the type of colony is mainly related to the growth condition and production of hyaluronidases.
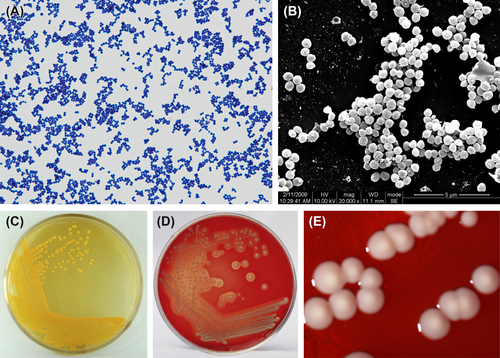
Figure 5.1 (A) Staphylococcus aureus cells (Gram stain). (B) S. aureus cells (SEM). The cells of S. aureus are characterized as being spherical (0.5–1.5 μm in diameter), gram-positive cocci arranged as single cells, pairs, tetrads, and clusters. (C) Golden pigment of S. aureus incubated on common agar plate. (D) β-hemolytic zone of S. aureus incubated on blood BHI agar plate. (E) Colonies of S. aureus (stereomicroscope).
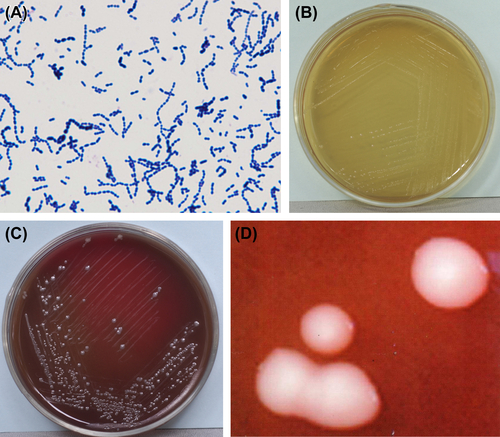
Figure 5.2 (A) Cells of S. mitis (Gram stain). (B) Colonies of S. mitis (TPY agar plate). (C) Colonies of S. mitis (BHI agar plate). (D) Colonies of S. mitis (stereomicroscope).
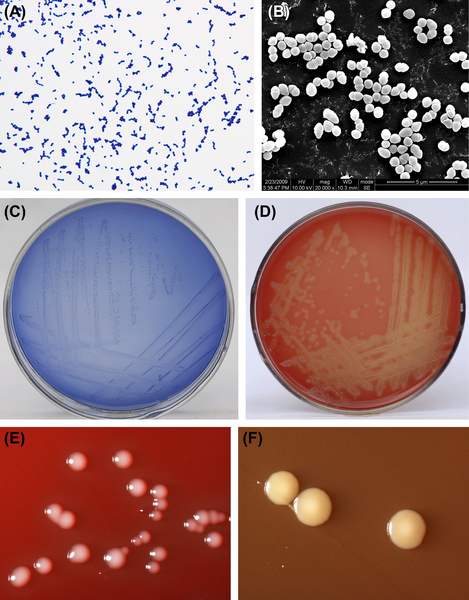
Figure 5.3 (A) Cells of S. pyogenes (Gram stain). (B) Cells of S. pyogenes (SEM). (C) Colonies of S. pyogenes (MS agar plate). (D) Colonies of S. pyogenes with β-hemolytic zone (BHI-blood agar plate). (E) Mucoid colonies of S. pyogenes (BHI-blood agar plate, stereomicroscope). (F) Lackluster colonies of S. pyogenes (BHI-blood agar plate, stereomicroscope).
S. pyogenes can produce several pathogenic virulence factors, including bacteriocins, hemolysin O, streptokinase, NADH enzyme, hyaluronidase, and M protein. The main sites of colonization for S. pyogenes are the dental plaque, hypopharynx, and the upper respiratory tract. Clinical samples can be isolated from skin lesions, inflammatory secretions, or blood. S. pyogenes can also be found in loose connective tissue inflammation in the maxillofacial region, pulpitis, or infection after exelcymosis.
5.1.2.3. Streptococcus pneumoniae
S. pneumoniae cells are spherical or elliptic (about 0.5–1.25 μm in diameter) and mostly arranged in pairs. They can occasionally be found in short chains or as single cells. Typical cells of this species are lanceted and arranged in pairs, and the extracellular capsule can be observed by capsule staining. However, cells can easily form chains after continuous culture. Cells of S. pneumoniae are gram-positive but can change to be gram-negative when aged (Figure 5.4(A) and (B)). S. pneumoniae cells observed by SEM are shown in Figure 5.4(C). The GC content of the S. pneumoniae genome is 30% (by Tm method) or 42% (by Bd method), and its type strain is NCTC7465.
S. pneumoniae is a kind of facultative anaerobe, but could generate a substantial amount of H2O2 under aerobic conditions. Growth of S. pneumoniae requires a complex medium rich in nutrients, including blood, serum, or ascites, as well as vitamin B. Cells of this species grow well on BHI-blood agar plates, and form roof-like, reflective and smooth colonies or rugose, mycelium-like, rough colonies (Figure 5.4(D)). Cells of S. pneumoniae can generate a great deal of capsular polysaccharides and therefore often form sticky colonies (Figure 5.4(E)). In fact, this capsular polysaccharide is the species-specific antigen and virulence factor of S. pneumoniae. S. pneumoniae cells observed by stereomicroscope are shown in Figure 5.4(F). The final pH value of a culture in glucose broth is pH 5.0. Compared to other streptococci, the addition of bile or cholate is required for the isolation and identification of S. pneumoniae.
S. pneumoniae carries out metabolic reactions through fermentation. Cells of this species can ferment glucose, galactose, fructose, sucrose, maltose, raffinose, and inulin to produce acid, and some strains can also ferment mannitol but not dulcite and sorbitol. Bacteriolysis of S. pneumoniae cells by bile is positive, and this characteristic is helpful in distinguishing S. pneumoniae from other streptococci.
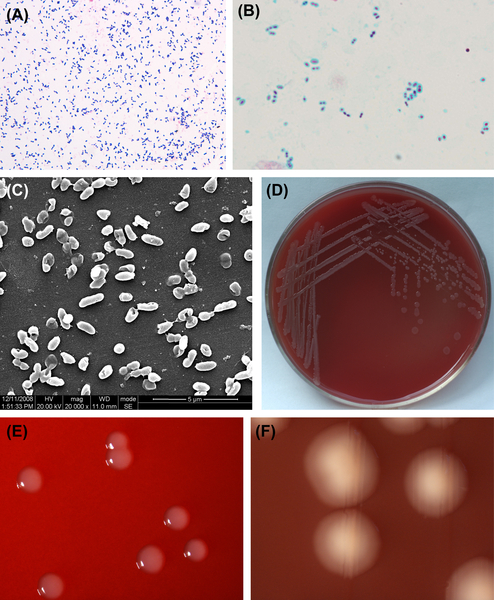
Figure 5.4 (A) Lanceted cells of S. pneumoniae (Gram stain). (B) Capsule of S. pneumoniae cells (capsule stain). (C) Cells of S. pneumoniae (SEM). (D) Colonies of S. pneumoniae (BHI-blood agar plate). (E) Sticky colonies of S. pneumoniae (BHI-blood agar plate, stereomicroscope). (F) Colonies of S. pneumoniae (stereomicroscope).
S. pneumoniae mainly inhabits the upper respiratory tracts of healthy individuals or livestock and can be isolated from clinical samples of amygdalitis, pneumonia, meningitis, and otitis media. However, the colonization, distribution, and pathogenicity of this species in oral cavity are still unknown.
5.1.2.4. Streptococcus vestibularis
S. vestibularis gets its name because this species was first isolated from the vestibule of the human oral cavity. The cells of S. vestibularis are gram-positive, spherical (about 1 μm in diameter), and arranged in chains (Figure 5.5(A)). S. vestibularis cells observed by SEM are shown in Figure 5.5(B). The GC content of the S. vestibularis genome is 38–40%, and its type strain is TC12166 (= MM1).
S. vestibularis is a facultative anaerobe, and the optimal temperature for growth is 37 C, but cells of this species can also still grow at 10–45 C. Except the type strain MM, the majority of strains belonging to this species can grow in media containing 10% bile. However, the species cannot grow in medium containing 4% NaCl, 0.004% crystal violet, or 40% bile. Alpha-hemolysis can be detected for all strains of this species growing on horse blood agar plates. In addition, black blue, lackluster, and umbilicate colonies (about 2–3 μm in diameter) with wavy edges can be observed when cells are grown on MS agar plates under anaerobic conditions (37
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


