Oral health disparities refers to the existence of differences in the incidence, prevalence, mortality, and burden of oral diseases and other adverse health conditions, as well as the use of health care services, among specific population groups in the United States. Existence of disparities in oral health status, accessing and using the oral health care delivery system, and receiving treatment depending on gender, race or ethnicity, education, income, disability, geographic location, and sexual orientation have been documented. Different states have initiated a series of steps as tools to document, assess, develop strategies, and monitor progress in efforts to eliminate or reduce oral health disparities in the United States.
Research into health disparities has grown tremendously since welfare economic studies associating poverty and health outcomes gained world-wide recognition: “… the poor should not be regarded as an undifferentiated mass, but that one should rather identify particular groups which have been struck by a catastrophic imbalance between needs and resources. Small-holders, farm laborers, tenant farmers and herdsmen may well all be poor, but the ways in which they are affected by famine can differ greatly” .
Essentially, disparity is the occurrence of differences between any two or more groups. As a dispassionate term, it is devoid of any qualifications and denotes existence of differences. However, health or social awareness and activism impart a qualification to health disparities, underlining a need to change status quo and remove disparities to improve health of those whose health status lies below that of the chosen reference. The National Institutes of Health has defined disparities as the “differences in the incidence, prevalence, mortality, and burden of diseases and other adverse health conditions that exist among specific population groups in the United States” . Other entities, such as the National Cancer Institute and Minority Health and Health Disparities Research and Education Act of 2000 , have defined disparities slightly differently, although the major focus is on the existence of differences between groups.
In the United States, disparities have been observed in oral health outcomes by gender, race or ethnicity, education, income, disability, geographic location, and sexual orientation . The National Institute for Dental and Craniofacial Research (NIDCR) has set up a Health Disparities Research Program, with “a plan to eliminate craniofacial, oral and dental health disparities,” in response to the growing awareness that despite improvements in some oral health status indicators, the burden of disease is not evenly distributed across all segments of societies .
Equality, equity, and disparity
Oral health equality implies the existence of equal oral health attributes among different groups, whereas the term “equity” incorporates an ethical quality to equality or disparity. Therefore, when we state, for example, that the burden of periodontal disease is greater in non-Hispanic Blacks, compared with non-Hispanic Whites , we just make a statement about existent disparity. However, when we make an ethical qualification stating that the above disparity is unacceptable and should be eliminated or reduced, then we choose to a stand in favor of oral health equity. Merely documenting oral health disparity in the absence of oral health equity does not allow us to take considered action toward the betterment of population oral health status.
As identified by NIDCR, disadvantaged and underserved population subgroups that fit within the research activities supported by the Health Disparities Research Program to eliminate or reduce disparity include:
-
All race and ethnic populations with health disparities, including African American, Hispanic (Mexican, Puerto Rican, Cuban, Central or South American, or other Spanish culture or origin, regardless of race), American Indian or Alaskan Native, and Asian or Pacific Islanders;
-
Low income rural (eg, Appalachian) or urban dwellers;
-
Special needs populations (eg, physically or mentally disabled);
-
People living with HIV/AIDS;
-
The elderly; and
-
Home-bound and institutionalized individuals
Existing oral health disparities
The first ever report on oral health, by the Surgeon General of the United States in the year 2000, brought into focus the profound oral health disparities existing in the country . Not only are there profound differences in the population in accessing the oral health care delivery system, but it has also been shown that even after accessing this system, there are substantial differences in clinical condition, awareness of treatment options, treatment discussions, treatment recommendations, and treatment received by different social groups .
Disparities in oral health status
Dental caries
Despite remarkable reduction in the prevalence of dental caries in the United States, childhood dental caries are still highly prevalent among the socially disadvantaged (racial or ethnic minority, poor, rural, immigrants) sections of United States society. According to the National Health and Nutrition Examination Survey (NHANES), caries experience in primary teeth in children aged 2 to 5 years has increased from the periods of 1988–2004 (NHANES III), to 1999–2004 (NHANES 1999–2004) . Although the overall prevalence of dental caries status of permanent teeth has decreased over the last 15 years (since the 1988–1994 NHANES III survey), profound disparities in disease prevalence, treatment received, and treatment outcomes continue to remain between various social groups .
Sequelae of dental caries (such as pain and complex dental treatment needs), therefore, also are more prevalent among children from these socially disadvantaged groups . Children from these groups experience the greatest amount of oral disease, the most extensive disease, and the most frequent use of dental services for pain relief .
Dental diseases in early childhood impact the growth, function, behavior, and comfort of the affected children. The twin disparities of poor oral health and lack of dental care are most evident among low-income preschool children, who are twice as likely to have cavities as are higher income children . These disparities continue into adolescence and young adulthood, although to a lesser degree. Disparities in oral health status and access to dental care are also evident when comparing African American, Hispanic, and Native American children to Caucasian children, and when comparing children of parents with low educational attainment to children of parents with higher educational attainment. The fastest growing populations of children are those that currently have the highest disease rates and the lowest amount of dental care .
Tooth loss
Race and socio-economic disadvantage are strong determinants of tooth loss . Cunha-Cruz and colleagues examined whether socio-economic disparities in edentulism had changed over time, by investigating the socio-economic disparities in edentulism between 1972 and 2001 using NHANES data for those years. They reported that overall, prevalence of edentulism remained approximately stable over the three decades, being 10.6% in 1972, 12.1% in 1991, and 11.3% in 2001. Furthermore, although the absolute difference in prevalence of edentulism between low and high socio-economic position groups remained unchanged, disparity was substantial for those who did not visit a dentist in the previous year when compared with those who did .
The Florida dental care study found that tooth loss was associated with certain practice characteristics, such as the racial mix of the practice’s patient population . This study reported that persons who attended practices with higher percentages of African Americans were more likely to receive a dental extraction, regardless of the individual patient’s race or ethnicity. These effects remained even after adjusting for several other factors .
Periodontal disease
Disparities in periodontal health status in the United States follows the similar general description in that those with lower socio-economic position and minorities tend to have more and more advanced disease burden than the rest . Progression of periodontal disease may be a function of several factors, including the disease status at the initial stages and factors that determine ability to use the oral health care delivery system.
A study of 53 Asian, 69 African, and 62 Hispanic Americans assessing periodontal disease progression found that the rate of attachment loss for the entire population was 0.24 mm per year, but did not find any differences among the three ethnic or racial groups. Although in bivariate analyses the study reported greater progression of disease for several factors (older study participants, professionally unskilled personnel, men, mean whole-mouth plaque, erythema, bleeding upon probing, suppuration, attachment loss, and probing depth), most of these associations disappeared on multivariable analyses to develop a final logistic regression model .
It is possible that observed disparities in periodontal diseases are the products of more complex interaction of two or more factors. Extracting such information hidden in data might require clear hypothesis testing and well thought-out study designs that have adequate statistical power to detect the differences hypothesized. In another study with a somewhat larger sample size (232 non-Hispanic Blacks and 199 Whites), subjects from a disproportionate probability sample of community-dwelling adults were interviewed regarding demographic, psychosocial and enabling factors, dental health-related behaviors, and other risk factors, and had a comprehensive in-home dental examinations . This study reported that prevalence of established periodontitis was greater among non-Hispanic Blacks (29.8%) than Whites (17.7%), with non-Hispanic Blacks having almost double the risk of established periodontitis than Whites (crude odds ratio or OR: 1.98; 95% confidence index or CI 1.43, 9.24). However, this study also reported an effect-modification of this association by dental check-up visit frequency . Blacks with dental check-ups at least once a year had almost a fourfold higher odds of established periodontitis (OR 3.64; CI 1.43, 9.24), compared with Whites with similar check-up experience, whereas Blacks with a dental check-up once every 2 years or less often were more than fourfold less likely to have established periodontitis (OR 0.22; CI 0.08, 0.59) than their White counterparts in the referent group.
It has also been reported that periodontal treatment needs vary with socio-economic position, and that although most American adults need some type of periodontal treatment, these are usually within the clinical skill range of dental hygienists . However, the proportion of need for complex periodontal treatment among those with lower socio-economic position is disproportionately higher than the rest. Assessing NHANES III data of 11,339 persons aged 20 to 79, Dye and Vargas estimated that overall, 3% of the adult United States population required complex periodontal treatment, 90% needed scaling and prophylaxis, and nearly 5% did not need periodontal treatment or oral hygiene instruction. Using multiple logistic regression analysis, the investigators were able to report that being older, male, non-Hispanic Black (OR 2.51; CI 1.98, 3.18), having lower education or no high school (OR 2.10; CI 1.60, 2.77), smoking (current smoker, OR 2.02; CI 1.76, 2.33), or not having had a dental visit in the past year increased the likelihood of needing more complex periodontal treatment.
Oral cancer
The oral cancer story mimics that of other oral disease: despite overall decreases in oral cancer incidence and mortality rates, the disparities associated with socially disadvantaged groups have continued to exist. From 1975 through 2004, age-adjusted incidence rates ( Fig. 1 ), age adjusted mortality rates ( Fig. 2 ), and survival rates ( Fig. 3 ) from oral and pharyngeal cancers are higher for men than women, being highest for Black men.
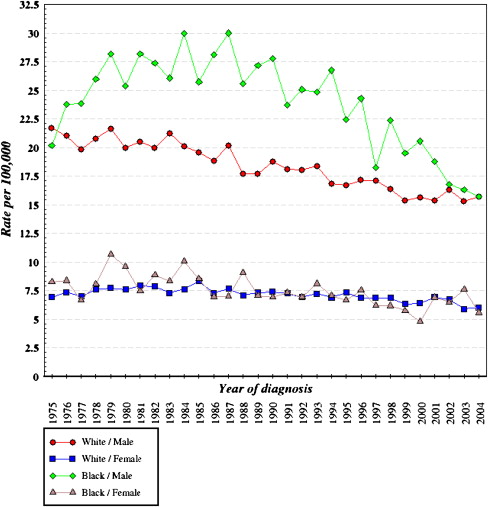
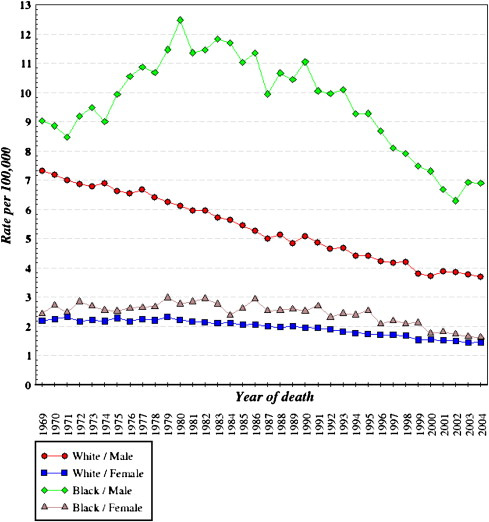
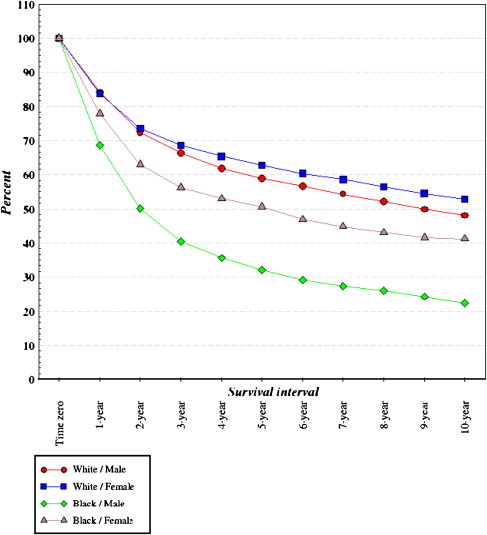
These figures suggest that overall, the Black–White disparity in oral and pharyngeal cancer can be broken into three parts.
- 1.
Roughly similar incidence rates for Black and White women, being generally stable over the years, albeit occasional fluctuations for Black women in incidence. However, the survival and mortality rates have consistently been in favor of White women compared with Black women.
- 2.
Substantial and prolonged disparity in incidence rates between Black and White men, which seem to have found a meeting point in the early 2000s. Incidence rates in Black men seem to have started to decline steadily from the mid 1980s, and current data suggests that the disparity with White men in age-adjusted incidence has been eliminated. However, age adjusted mortality rates and survival rates tell a very different story, with substantial disparities in favor of White men.
- 3.
Despite changes, the disparities in incidence, mortality, and survival between men and women, in favor of women, has remained approximately steady over the years.
A recent study reported that age adjusted mortality rates were 82% higher for Black men compared with White men, but rates were similar for Black and White women. Five-year relative survival rates for patients diagnosed during the period 1995 to 2001 were higher for Whites than for Blacks and lowest for Black males . Interestingly, the survival rates of oral cancer have remained fairly stable over the decades. Similar results have been reported from Florida , Kentucky , North Carolina , and elsewhere.
Table 1 shows the stages of oral and pharyngeal cancer at presentation from the Surveillance Epidemiology and End Results (SEER) data in 5-year groups every 10-years. Whereas the overall trends are similar for Blacks and Whites, the greater proportion of earlier stage presentation among Whites over Blacks stands out. Although the proportion of regional spread presentations increased for all, the proportion of increase is greater for White men compared with Black men (10% versus 18%, respectively) from 1985–1989 to 1996–2003.
| White | Black | |||||
|---|---|---|---|---|---|---|
| All | 1975–1979 | 1985–1989 | 1996–2003 | 1975–1979 | 1985–1989 | 1996–2003 |
| Percent localized | 41% | 40% | 36% | 26% | 18% | 20% |
| Percent regional | 37% | 43% | 50% | 49% | 56% | 60% |
| Percent distant | 12% | 9% | 9% | 17% | 19% | 16% |
| Percent un-staged | 10% | 8% | 5% | 8% | 7% | 4% |
| White men | Black men | |||||
|---|---|---|---|---|---|---|
| Men | 1975–1979 | 1985–1989 | 1996–2003 | 1975–1979 | 1985–1989 | 1996–2003 |
| Percent localized | 41% | 39% | 34% | 25% | 15% | 16% |
| Percent regional | 37% | 44% | 52% | 51% | 57% | 63% |
| Percent distant | 12% | 9% | 9% | 17% | 22% | 17% |
| Percent un-staged | 10% | 8% | 4% | 7% | 6% | 4% |
| White women | Black women | |||||
|---|---|---|---|---|---|---|
| Women | 1975–1979 | 1985–1989 | 1996–2003 | 1975–1979 | 1985–1989 | 1996–2003 |
| Percent localized | 40% | 41% | 42% | 30% | 26% | 29% |
| Percent regional | 39% | 42% | 43% | 46% | 53% | 54% |
| Percent distant | 11% | 8% | 8% | 16% | 13% | 12% |
| Percent un-staged | 9% | 9% | 6% | 8% | 8% | 5% |
Orofacial pain
The Florida dental study, using standardized telephonic surveys assessing 724 dentate adults above 45 years of age, has contributed substantially toward understanding prevailing disparities in self-reported orofacial pain in the United States . This study reported that lower socio-economic position was associated with greater self-reported pain and pain impact at many orofacial sites. This observation suggests that persons with lower socio-economic position are at increased risk for orofacial pain and pain-related behavioral impact, measured as pain having reduced their daily activities or motivating them to take some action in response to it. Furthermore, this association of socio-economic position and orofacial pain varied by sex: only men with lower financial status were at increased risk for orofacial pain-related behavioral impact in at least one site . However, in a study of senior citizens (65 years or older), although prevalence of self-reported orofacial pain did not differ by race or ethnicity, there were differences in behavioral impact associated with pain . This latter study found that Blacks reported greater behavioral impact, even after adjusting for socio-economic status, approach to health care, and intensity of pain.
Persons with special care needs
Oral health related disparities are perhaps most evident and severe when persons with special care needs are assessed against those who do not need special care for management of their oral health problems. The Surgeon General’s report on oral health stated that people living below the poverty level and those with mental retardation or physical disabilities have poorer oral health than the general population . One study examined the oral health status of intellectually disabled persons, with or without a physical disability, by screening 12,099 Special Olympics athletes at 53 sites, including 1,891 people from seven states in the southeastern United States . The examinations were performed by volunteer dentists and dental students. Oral health disparities in this study sample were associated with poverty. Restricting the analysis by age, the study reported that athletes from the very poor southeastern states were 1.6 times (OR 1.64; 95% CI 1.10–2.46) more likely to have restorations and almost one-third as likely (OR 0.35; 95% CI 0.21–0.60) to have sealants than were athletes from the poor states. Adults with developmental disabilities generally have a more sedentary life-style, poorer general health, and multiple comorbidities when compared with those without such disabilities . Nursing home residents, mostly elderly persons who can barely perform or need support for activities of daily living, have poor oral health and inadequate access to oral health care. Further details are discussed in the article by Chalmers and Ettinger elsewhere in this issue.
These persons with special needs also have poorer rates of insurance coverage and have substantially lesser rates of use of the health care delivery system. These issues also translate to their poorer oral health as compared with the general population. Current oral health surveillance methods do not cover this population, although the potential of substantially elevated unmet needs among this population are perhaps the greatest.
Elderly persons
Dental caries (coronal and root caries) continue to be a problem requiring public health attention for the noninstitutionalized elderly, especially African Americans who also use the oral health care system less and have poorer insurance coverage. Those elderly persons with lower socio-economic position, living in rural areas, or those who have special care requirements, have greater unmet needs compared with the other elderly Americans. Further details are discussed in an article by Chalmers and Ettinger elsewhere in this issue.
Disparities in oral health service access
Service use
Utilization of available oral health care services is a good marker for how well the current oral health care delivery system is working. Utilization of the oral health care delivery system varies by the socio-economic position and racial or ethnic characteristic of the population. Analysis using a nationally representative sample from the 1996 Medical Expenditure Panel Survey demonstrated that there was an approximate twofold difference in the proportion of persons accessing the oral health care delivery system between the lowest income group (28.1% for persons below 200% of the federal poverty line) and the highest income group (55.8% for persons above 400% of the federal poverty line) . Other findings from the study include: Non-Hispanic Blacks and Hispanics were less likely to access the system than Whites or other race and ethnic groups; men were less likely to access the system than women; and people not in employment were less likely to access the system than those employed .
Assessing the recent expansions in Medicaid and the State Children’s Health Insurance Program (SCHIP), a recent study reported that overall, use of ambulatory dental care has increased dramatically for children over the past two decades . In 1983, more than one in three children (38.5%) had no dental care within the previous 12 months, which decreased to 26.3% in 2001. However, frequency of unmet dental care did not change from 1997–1998 to 2001–2002. The same study did not find any changes in income disparities for unmet dental needs . Even today, as earlier, low income children are less likely to visit the dentist in part because of their family’s competing needs for limited resources, shortage of pediatric dentists, and dentists not taking uninsured or publicly insured patients .
Over the past decade, the proportion of the American population reporting to have visited a dentist in the previous year has remained fairly constant (ie, 69% in 1996, 68% in 1999, 69.5% in 2002, and 69% in 2004) . A New York State survey among minorities found that self-reported visits to a dentist in the previous year was only 63% , 10% lower than the estimated state average. Perhaps it would be safe to assume that these proportions of differences would be substantially higher if undocumented immigrants were accounted for. Therefore, unless some type of immigration reform occurs to bring undocumented immigrants into the legal system with impunity, disparities for this group will continue to be high and perhaps increasing, compared with the rest of the United States population.
Substantial disparities exist in the use of orthodontic services among high school students . This study reported that the odds of being orthodontically treated were 8.7 times greater among those with dental visits within the past year than among those without, and three times greater among Caucasians than among other ethnic groups. Furthermore, ethnic minority groups had 2.6 greater odds of needing orthodontic treatment than Caucasians .
In the adjusted regression models, Black patients and those with unknown race were less likely overall to receive root canal therapy than Whites, whereas Asians were more likely. Among patients with eligibility for continuing and comprehensive dental care, Blacks were less likely and Asians more likely to receive root canals than Whites. For patients covered only for emergency dental care, Hispanics had a higher likelihood of receiving root canal therapy. Among all other types of coverage, there were no significant racial differences in the care received .
Household income plays a major role in a family’s ability to access the oral health care system. It is well established that adults and children from poor households have the most oral health disease and access the system the least. Paradoxically, children in poverty—those living in households with annual gross incomes under $16,500 for a family of four—or near poverty (those in family households with incomes between $16,500 and $33,000), also have the highest rates of dental insurance coverage, primarily through Medicaid programs and SCHIP . Medicaid-eligible children who have cavities have twice the numbers of decayed teeth and twice the number of visits for pain relief, but fewer total dental visits, compared with children coming from families with higher incomes. Fewer preventive visits for services such as sealants increase the burden of disease in low-income children .
Geographic and neighborhood issues
In addition to existing statistical techniques, recent advances in Geographic Intelligent Systems (GIS) software applications have allowed investigators to assess geographic disparities in an easily understandable format, which includes graphic analysis, overlays, and much more. These methods allow a readily appreciable pictorial description of differences of attributes between geographic zones. In conjunction with existing methods, GIS applications strengthen program planning and visual interpretation of information. For example, individual and overlay maps were produced in a study to examine the geographic distribution of New York City adults aged 65 and older, by race or ethnicity and poverty status . This study found that Black race, Hispanic ethnicity, and poverty status tended to occur together geo-spatially among elders in Northern Manhattan and the South Bronx, information that can be incorporated in planning oral health service delivery for elders .
Oral health disparities exist among United States adults living in rural and urban areas. Using NHANES III data, Vargas and colleagues reported that compared with urban residents, rural residents were less likely to report a dental visit in the past year and were more likely to be edentulous. Adults living in rural areas were more likely to report having unmet dental care needs and were less likely to have had a dental visit in the past year, compared with adults living in urban areas . The prevalence of edentulism among rural adults was 16.3%, almost twice that of urban adults. Caries experience also was more likely to be greater among adults residing in rural areas.
A study in Harlem, New York reported that those with low income, unemployed, and uninsured, had poorer oral health status, emphasizing that the privately insured were almost twice as likely to have seen a dentist for oral health problems as were the uninsured . Inability to pay for dental services received (unpaid care) may be a marker for low socio-economic position, and may be adopted as a possible coping strategy for obtaining minimal, but essential services when in need. Data from the 1996 Medical Expenditure Panel Survey suggests that unpaid care was higher for those living in northeast and in west census tract zones when compared with other areas, and for the oldest age groups, women, low income, unemployed, Hispanics, those with Medicaid, and those undergoing more than one dental procedure type . The differences in unpaid care between geographic areas (census tracts zones) persisted even after adjustment for other important variables. Although it may not be easy to explain such differences, ecologic comparison of evidences from other studies may suggest the possibility of some association with the distribution of undocumented laborers who generally live in an “informal-economy.” These individuals may resist accessing the oral health care delivery system out of fear of possible backlash from other sections of the political system, to avoid being discovered and deported. Such possibilities are becoming important for the American health care delivery system, as the system tries ways to provide health care to this vulnerable population.
Neighborhoods may impart unique qualities to oral health status of residents beyond socio-economic position and individual risk factors. An assessment of the relationship between neighborhood effects and the severity of dental caries among low-income African Americans using multi-level methods suggested there is significant variation in the severity of caries between low-income neighborhood clusters . This study demonstrated that caries severity was lower in areas with a higher number of churches, whereas it was greater in areas with a higher number of grocery stores in the clusters, after accounting for several individual characteristics. Only 14% of the interindividual variability in dental caries in this study was explained by classic individual risk factors .
More remote areas of the United States also exhibit profound between-region disparities in oral health. For example, a disproportionately higher proportion of American Indian and Alaska Native children have oral disease, compared with the general population of American children, apart from having limited access to professional oral health care . It is well documented that the Indian Health Service and American Indian and Alaska Native tribal leaders face a significant problem in ensuring care for the oral health of these populations .
Table 2 lists the national oral health attributes from the 2004 Behavioral Risk Factor Surveillance System (BRFSS) and those of the states that reported state-wide surveys to the National Oral Health Surveillance System (NOHSS). The NOHSS is a collaborative effort between the Centers for Disease Control Division of Oral Health and the Association of State and Territorial Dental Directors that was established in 2001. NOHSS is designed to monitor the burden of oral disease, use of the oral health care delivery system, and the status of community water fluoridation on both a national and state level. NOHSS includes eight indicators of oral health, information on state dental programs, and links to other important sources of oral health information.



