Fig. 13.1
A nutrition assessment is more comprehensive than screening and includes a medical history, a nutrition focused physical examination including oral examination, anthropometric measurements, and laboratory values. This assessment provides the RD the means to diagnose nutrition problems and identify and address nutritional problems and potential deficiencies prior to treatment initiation, throughout the course of treatment and following treatment. The Patient-Generated Subjective Global Assessment (PG-SGA) (Fig. 13.2) is a nutrition assessment tool that has been validated for use in adults with cancer [8]. The patient generated portion (PG) of the PG-SGA is a self-administered four-item questionnaire which includes weight history, symptoms, food history, and activity level. The practitioner completes the remainder of the worksheet and calculates a score based on the physical examination, diagnosis, metabolic demand, and comorbidities. Although nutrition screening would be the initial component identifying those at nutrition risk in all healthcare settings, a healthcare organization must determine what tool is utilized, who is at risk, and how often reassessment is to take place [5]. A referral process is necessary to ensure patients who are identified at-risk are seen by the RD in a timely manner.
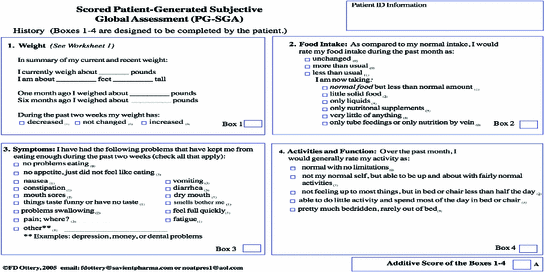

Fig. 13.2
Patient generated subjective global assessment (PG-SGA) for cancer http://www.accc-cancer.org/oncology_issues/supplements/pgsga.pdf
Head and Neck Cancer Treatment and Nutrition Impact Symptoms
Treatment options selected determine the immediate, intermediate, and long-term impact on nutrition status (see Table 13.1). HNC treatment approaches are chosen based upon disease factors (site, extent of disease, pathologic findings), presence or absence of comorbid conditions, and patient preference. Treatment is often aggressive involving surgery, chemotherapy, radiation therapy, or a combination of modalities. Potential nutrition complications resulting from the tumor, surgery, chemotherapy, and radiation therapy in the treatment of HNC are identified in Table 13.1 [4, 12, 20–25]. The size and location of the tumor may affect oral function, particularly if involving the oral tongue, base of tongue, and oropharynx. In addition to mass effects and affect on function of the involved site, pain may affect oral intake. Localized oral lesions (Stages I and II) are primarily treated surgically, whereas those of the oropharynx are primarily treated by radiation therapy. For locally advanced cancer and those with locoregional disease (Stage III/IV disease) multimodality therapy is required.
|
Nutrition complications after head and neck cancer surgery
|
||||||||
|---|---|---|---|---|---|---|---|---|
|
Surgery
|
Compromised swallowing and aspiration potential
|
Delayed swallow (>10 seconds)
|
Dysphagia, odynophagia, postoperative swelling
|
Dental extractions/altered dentition
|
Dry mouth/altered taste
|
Inability to meet energy needs
|
||
|
Base of tongue resection
|
X
|
X
|
X
|
X
|
||||
|
Total glossectomy
|
X
|
X
|
X
|
X
|
X
|
|||
|
Partial glossectomy
|
X
|
X
|
||||||
|
Floor of mouth resection
|
X
|
X
|
X
|
X
|
||||
|
Hypopharyngeal resection
|
X
|
X
|
X
|
X
|
||||
|
Total laryngectomy
|
X
|
X
|
X
|
|||||
|
Partial laryngectomy
|
X
|
X
|
X
|
|||||
|
Total maxillectomy
|
X
|
X
|
X
|
X
|
||||
|
Pharynogo-laryngectomy
|
X
|
X
|
X
|
|||||
|
Oropharyngeal resection
|
X
|
X
|
X
|
X
|
X
|
|||
|
Mandiblectomy
|
X
|
X
|
X
|
X
|
||||
|
Buccal/mucosal resection
|
X
|
X
|
X
|
|||||
|
Loss of 7th cranial nerve
|
X
|
X
|
X
|
X
|
||||
|
Thyroidectomy
|
X
|
X
|
||||||
|
Oral complications related to chemotherapy
|
||||||||
|---|---|---|---|---|---|---|---|---|
|
Complication
|
Direct risk factor
|
Indirect risk factor
|
||||||
|
Oral mucositis
|
Mucosal cytotoxicity
Physical/chemical/microbial irritation
|
Decreased local/systemic immunity
Local infections, reactivation of herpes simplex virus
|
||||||
|
Oral infections
|
||||||||
|
Viral
|
Decreased systemic immunity
|
|||||||
|
Fungal
|
Antibiotics, steroids, salivary gland dysfunction, and local immunity
|
Decreased systemic immunity
Altered oral flora
|
||||||
|
Bacterial
|
Inadequate oral hygiene
Mucosal breakdown
Acquired pathogens
|
Decreased systemic immunity
Salivary gland dysfunction
|
||||||
|
Taste dysfunction
|
Taste receptor toxicity, neural toxicity
|
Salivary gland dysfunction
Mucosa and taste receptor damage
|
||||||
|
Xerostomia
|
Salivary gland toxicity
|
Xerogenergin medications: (e.g.,: anti-hypertensive, anticholinergic, antianxiety drugs, opioids)
|
||||||
|
Neuropathies
|
Vinca alkaloid drug use; specific drug toxicity (platinum, taxanes, etc.); surgical neuropathy, radiation toxicity
|
Anemia, dental hypersensitivity
|
||||||
|
Gastrointestinal mucositis causing secondary changes in oral status including taste, hygiene, and dietary intake
|
Mucosal cytotoxicity: radiation and chemotherapy
|
Nausea and vomiting
|
||||||
|
Hemorrhage
|
Oral mucositis
Physical trauma
Infections
|
Thrombocytopenia
Decreased clotting factors
|
||||||
|
Oral complications related to radiation therapy
|
||||||||
|---|---|---|---|---|---|---|---|---|
|
Acute complications
|
Chronic complications
|
Results of significant toxicities caused by radiation to the head and neck region
|
||||||
|
Anorexia
Dysgeusia
Dysosmia
Dysphagia
Infection—fungal or bacterial
Odynophagia
Oral mucositis
Salivary gland dysfunction
Sore mouth and throat
Taste dysfunction
Xerostomia
|
Ageusia/dysguesia/dysosmia
Cachexia
Dental demineralization/caries
Infection—fungal or bacterial
Mucosal fibrosis and atrophy
Muscular/cutaneous fibrosis
Osteonecrosis
Soft tissue necrosis
Trismus
Xerostomia
|
Dehydration
Dental complications
Discontinuation of treatment
Dose limitations
Extreme fatigue
Hospitalization
Oral complications and pain
Taste alterations
Treatment interruptions
Weight loss
Ultimately poor outcome
|
||||||
Oral toxicities, those symptoms that occur secondary to cancer treatments often coexist and are interdependent; they may be classified as acute or late effects. An acute toxicity typically occurs early in the course of treatment and generally resolves by treatment completion. For example, patients who undergo concurrent chemoradiation therapy experience acute effects that create nutritional challenges. However, it is possible that an acute toxicity may fail to resolve and may persist as a late effect toxicity [26]. Early nutrition screening and assessment and prevention and management of oral complications in patients with HNC are essential. The Vanderbilt Head and Neck Symptom Survey 2.0 (VHNSS) allows practitioners to assess, qualify, and quantify symptom burden and duration in a timely manner [27, 28]. Symptom burden is a concept that refers to the combination of both the severity of symptoms and the patient’s perception of the impact of the symptom. The VHNSS was designed for use in a clinic setting by health professionals to identify specific symptoms associated with HNC including acute and late stage toxicities and to help guide clinical care. There are 50 questions within 13 domains that are specific to the HNC population. Questions are ranked on a scale of 0–10 with 0 indicating no issue and 10 indicating severe symptom issues. The VHNSS 2.0 addresses the possible adverse effects of treatment such as mucosal sensitivity, dental health, and trismus [27, 28]. OHCPs and RDs as well as other health professionals can use this tool during initial and periodic patient visits to determine symptoms impacting the ability to eat and drink and quality of life. The value of its use lies in the information gleaned that can be used to guide changes in treatment plans and management strategies.
In dentate, patients with xerostomia, the frequency of fermentable carbohydrate (carbohydrates that can be metabolized by salivary amylase) (e.g., fruits and juices, sugar-sweetened foods and beverages) intake must also be considered because they can increase the caries risk in already at-risk patients [29]. Some suggestions are to complete appropriate oral hygiene procedures (e.g., brushing teeth) before or immediately following consumption of sugar-sweetened foods and fluids including those with natural sugars such as fruits and juices/sweetened beverages, limiting these foods to mealtimes, and to maintain caries prevention strategies on a daily basis. In addition, acidic products in liquid form (e.g., citrus beverages including sugar-sweetened and sugar-free: fruit drinks, carbonated beverages, and ice tea) and in foods should be limited as they can irritate soft tissue and increase risk of tooth demineralization and caries. Common nutrition impact symptoms resulting from treatment and recommendations for management of diet and nutrition for individuals with acute toxicities are described in Table 13.2 [12, 20, 22, 30–32].
|
Common nutrition impact symptoms during treatment
|
Nutrition management
|
Comments for healthcare professional (RD)
|
|---|---|---|
|
Anorexia
|
• Consume small, frequent meals or snacks
• Fortify food and fluids versus increasing the volume (i.e., add protein powder to foods, smoothies)
• Drink nutrient-dense beverages (drink between meals to avoid feeling too full)
• Make the most of eating when energy is greatest
• Incorporate light exercise to stimulate appetite as feasible
|
• Identify symptoms that contribute to anorexia (i.e., pain, constipation, taste, etc.)
• Discuss pharmacological options with MD (i.e., Megace, Marinol, etc.)
• Monitor weight status
• Monitor hydration status
• Monitor for electrolyte imbalances
|
|
Aversion to food
|
• Use protein sources other than meat (a common aversion) such as cheese, cottage cheese, nut butter, eggs, etc.
• Use low odor food and fluids; cold or room temperature foods and fluids are often better tolerated
• Season foods to increase palatability (i.e., if food is too salty, add a sweet taste)
• Avoid favorite foods to prevent long-term avoidance posttreatment
• Purchase small quantities of any new item (it may be palatable one day, not the next. Taste can change on a daily basis)
• Cleanse the palate using baking soda/salt water rinses
|
• Utilize a dietary recall to identify foods that are tolerated well; offer suggestions to maximize intake
• Monitor weight status
• Monitor hydration status
|
|
Candida
|
• Use medications as prescribed
• Use excellent oral care; soft tooth brush
• Consume soft, moist, non-acidic foods and fluids
• Avoid spicy, dry, course, or rough food
• Avoid alcohol containing mouthwash
• Use a straw to avoid oral cavity (if swallowing function is intact)
• Consider the use of liquid high calorie, high protein oral nutrition supplements
|
• Encourage excellent oral care
• Reinforce the use of mouthwash or medication prescribed by healthcare provider
• Encourage patient to assess oral cavity at home
• Monitor weight status
• Assess for taste changes, decrease in intake
|
|
Constipation
|
• Utilize medications as prescribed
• Consume adequate fluid (8–10 cups/day)
• Eat foods high in fiber if consuming adequate fluid
• Eat at regular intervals
• Consume warm/hot fluids to stimulate bowel
• Try prune juice or prunes
• Integrate physical activity or light exercise as feasible
|
• Reinforce medication prescribed by healthcare provider
• Assess fluid intake; discuss estimated needs
• Determine date of last bowel movement
• Assess for nausea, anorexia
• Monitor weight status
|
|
Dehydration
|
• Consume small, frequent meals and snacks
• Consume fluids as able
• Use foods that are higher in fluids (i.e., soup, gelatin, melons, hot cereal)
• Avoid alcohol and caffeine
• Use Sippy cups or bottles that have a cover if smell is creating an aversion to drinking fluid
• Use lemon, lime, cucumber or mint in water if water tastes “off”
|
• Identify barriers to fluid intake
• Reinforce use of medications (i.e., anti-emetics)
• Assess actual oral intake of fluid
• Offer suggestions to increase fluid intake (i.e., foods that are higher in fluid such as soup, ice cream, gelatin, etc.)
• Consider IV fluids if oral intake goals are not attainable
• Monitor weight status
• Monitor for electrolyte imbalance
• Assess blood pressure, skin turgor, etc., for signs of dehydration
• Discuss signs of dehydration with patient (i.e., dark urine, skin turgor, lightheadedness)
|
|
Diarrhea
|
• Use medications as prescribed
• Use soluble fiber; limit insoluble fiber
• Increase fluid intake
• Consume small, frequent meals
• Consume cool or room temperature food and fluids
• Avoid dairy if lactose intolerant
• Avoid greasy, fried, or fatty foods
• Avoid spicy or rich foods
• Avoid excessive amounts of
sweetened beverages
• Limit foods and fluids containing sorbitol/xylitol or sugar substitutes
|
• Reinforce medication prescribed by healthcare provider
• Evaluate medications
• Monitor weight status
• Monitor hydration status
• Monitor for electrolyte imbalance
• Discuss foods that are high in soluble fiber
• Encourage adequate fluid intake; discuss estimated need and assess barriers to meeting goals
• Consider IV fluids if oral intake goals are not attainable
|
|
Dysphagia
|
• Utilize swallowing exercise/techniques provided by speech language pathologist (SLP)
• Use foods suggested by registered dietitian (dysphagia diet per National Dysphagia Diet guidelines); soft, moist or pureed foods
• Avoid bread, cakes, cookies (dry or crumbly/course foods)
• Avoid temperature extremes
• Use thickened liquids as suggested by SLP
|
• Referral to SLP
|
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


