This purpose of this article was to report the clinical case of a patient with Eagle’s syndrome. She was referred to the orthodontic clinic by her general clinician, with the complaint of temporomandibular dysfunction. The orthodontic records showed a styloid process elongation accompanied by calcification and fracture on the right side. Eagle’s syndrome was diagnosed, and the patient was referred to a buccomaxillofacial surgeon for surgical correction.
The styloid process is a slender bony projection that originates in the inferior portion of the temporal bone, medially and anteriorly to the stylomastoid foramen. The stylopharyngeal, stylomandibular, and stylohyoid ligaments are inserted in it.
Styloid process elongation is an anomaly that can be accompanied by calcification of the stylohyoid and stylomandibular ligaments, capable of causing a series of symptoms such as dysphagia, odynophagia, facial pain, otalgia, headache, tinnitis, and trismus. This set of symptoms associated with an elongated styloid apophysis is known as Eagle’s syndrome.
Eagle’s syndrome, or styloid-stylohyoid syndrome, is characterized by styloid process elongation or stylohyoid ligament ossification. Described in 1937 by the otorhinolaryngologist with the same name, this syndrome can be associated with various syndromes, none of them pathognomonic: dysphagia, sore throat, otalgia, and vague facial pain. The symptoms are based on the length of the styloid process, which originates from the temporal bone and proceeds between the internal and external carotid arteries.
The objective of this article was to describe a clinical case of a patient with Eagle’s syndrome, who sought treatment at the orthodontic clinic of Southwest Bahia University UESB with a complaint of temporomandibular dysfunction caused by occlusal maladjustment.
Case report
The patient, a 33-year-old woman, was referred to the orthodontic clinic by her prosthodontist with the complaint of temporomandibular joint dysfunction and malocclusion.
The intraoral clinical examination showed a Class II right subdivision dental relationship with exaggerated vertical overlap (overbite) and absence of the maxillary left canine and the mandibular right first molar. She reported discomfort on opening her mouth, pain when swallowing, and pain and limitation in lateral movements of the head ( Fig 1 ).
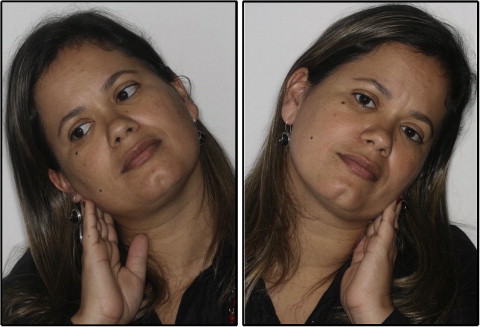
Complementary records were collected, including photographs ( Fig 2 ), radiographs ( Fig 3 ), and orthodontic impressions. The panoramic radiograph showed elongation of the styloid process and a fracture in the calcified ligament on the right. In the infra-auricular region, the patient complained of pain on palpation, particularly on the right side.
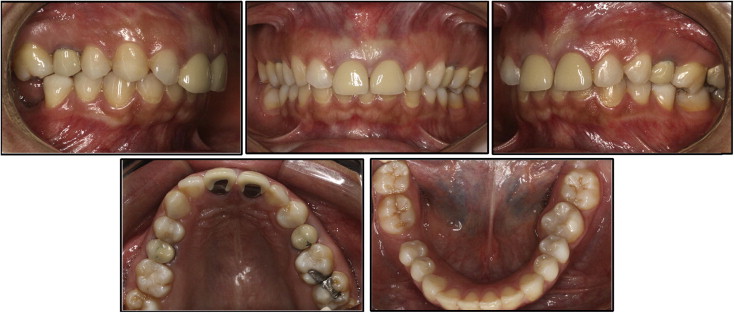
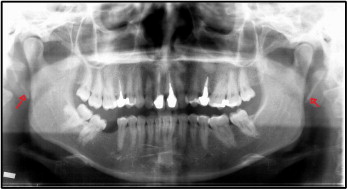
Starting from this observation, the patient was referred to a buccomaxillofacial surgeon for evaluation. The surgeon decided to perform a surgical intervention to remove the calcified process.
Thirty days after the surgical intervention, the patient returned to the clinic to begin orthodontic treatment, reporting improvement in the painful symptomatology.
Discussion
This article describes the clinical case of a patient who sought orthodontic treatment, complaining of pain in the temporomandibular joint region and difficulty with mouth opening and making lateral movements of the head. The patient had been referred by her prosthodontist, who attributed the pains to her malocclusion, and, according to him, he was faced with a temporomandibular dysfunction caused by poor dental positioning.
Molina, in a study on occlusion and the temporomandibular joint, considered that temporomandibular joint dysfunction could be present with greater frequency in patients with the following characteristics of occlusion: unilteral or bilateral posterior reverse articulation (crossbite), Class II malocclusion, mutilated occlusion, or an exaggerated Spee curve, combined with gross interference on the balancing side. This patient had some of these characteristics: Class II dental relationship, exaggerated curve of Spee, several missing teeth, and occlusal interferences. Thus, her symptoms could well fit the condition of temporomandibular dysfunction.
However, since orthodontic diagnosis is not based on clinical evaluation only, it was necessary to request intraoral and extraoral radiographs, photographs, and orthodontic impressions. Stylohyoid ligament ossification was diagnosed, verified by the panoramic radiograph.
To Phillips and Shawkat, the diagnosis of Eagle’s syndrome is made with adequate clinical and radiographic examinations, without which the patient would be subject to incorrect diagnosis and treatment.
The symptoms associated with styloid process elongation are more common than one would imagine; nevertheless, this syndrome is unknown to most general clinicians. Consequently, they overlook it during differential diagnosis with an extensive variety of dental, temporalmandibular joint diseases, and facial and oral neuralgias, as occurred with this patient.
To Prasad et al, elongated styloid processes could be the source of cervical and craniofacial pain, and diagnosis continues to be a challenge to many clinicians.
The clinical diagnosis of Eagle’s syndrome can be made during the physical examination, by means of palpation in the region of the styloid process in the tonsillar fossa, thereby stimulating and triggering painful symptomatology, as in this patient.
The treatment of Eagle’s syndrome depends on the degree of the patient’s discomfort, and, in most cases, it is surgery. Several studies have reported this to be the only effective treatment in symptomatic patients; nevertheless, treatments with analgesics, anti-inflammatory and psychotropic medications, and physiotherapy have been reported, in addition to alternative therapies that control the algic syndrome.
In this patient, the chosen therapy was surgical removal of the calcified area. About 30 days after the surgery, the patient reported improvement in her symptomatology.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


