Key points
- •
Salivary lesions of the neck comprise a variety of neoplastic and nonneoplastic processes. The determination of the involved gland and the exact pathologic process depends on a physical examination and a review of computed tomography (CT) scans or magnetic resonance imaging (MRI) of the neck.
- •
Once the salivary gland of origin of the neck mass is determined by physical examination and imaging review, the surgeon should determine whether fine-needle aspiration biopsy is required in preparation for removal of the pathologic entity.
- •
Benign parotid tail tumors are surgically managed by partial parotidectomy including facial nerve dissection and preservation; benign inferiorly located parotid tail tumors can occasionally be managed by extracapsular dissection without facial nerve identification.
- •
Malignant parotid tail tumors are typically managed with partial parotidectomy; malignant submandibular gland tumors are commonly managed with at least a 3-level prophylactic neck dissection that sacrifices the submandibular gland and tumor within the neck dissection.
- •
Fluid-filled lesions of the submandibular triangle are most commonly diagnosed as plunging ranulas and are typically managed by transoral excision of the etiologic sublingual gland; close scrutiny of the CT or MRI scans may reveal the presence of a submandibular gland mucocele that is managed by excision of the etiologic submandibular gland with or without associated sublingual gland excision.
- •
Chronic sialadenitis or sialolithiasis of the submandibular gland requires an assessment of the chronicity of the sialadenitis, the location of the sialoliths, and the likelihood of recovery of submandibular gland function when considering isolated excision of the submandibular sialoliths without excision of the submandibular gland.
Introduction
The diagnosis and management of masses of the neck require strict attention to obtaining a history and performing a physical examination so as to establish a differential diagnosis for the mass under consideration. The development of a differential diagnosis of a neck mass frequently includes neoplastic and nonneoplastic salivary lesions that are considered as a function of the age of the patient, the patient’s history, and the clinician’s physical examination of the patient. This exercise is particularly important because the surgeon must consider the role of fine-needle aspiration biopsy and imaging studies of the neck before providing definitive surgical therapy for the mass. The anatomic region of the mass of the neck also permits the surgeon to include or discard certain diagnoses. For example, most salivary lesions of the neck occur in the lateral upper neck region, and specifically in level IB (submandibular gland) and level IIA (parotid tail). While placing salivary lesions on the differential diagnosis of a neck mass, it is important to understand that incisional biopsies of such neck masses have no role to play in their management. It is therefore essential that surgeons rely on available preoperative measures, including the development of a comprehensive and orderly differential diagnosis, obtaining structural imaging studies, and performing a fine-needle aspiration biopsy as indicated so as to execute the proper surgical treatment plan. This article reviews salient features and the surgical management of the most commonly encountered salivary lesions of the neck, including the plunging ranula and submandibular gland mucocele, the parotid tail tumor, the submandibular gland tumor, and sialadenitis/sialolithiasis of the submandibular gland.
Introduction
The diagnosis and management of masses of the neck require strict attention to obtaining a history and performing a physical examination so as to establish a differential diagnosis for the mass under consideration. The development of a differential diagnosis of a neck mass frequently includes neoplastic and nonneoplastic salivary lesions that are considered as a function of the age of the patient, the patient’s history, and the clinician’s physical examination of the patient. This exercise is particularly important because the surgeon must consider the role of fine-needle aspiration biopsy and imaging studies of the neck before providing definitive surgical therapy for the mass. The anatomic region of the mass of the neck also permits the surgeon to include or discard certain diagnoses. For example, most salivary lesions of the neck occur in the lateral upper neck region, and specifically in level IB (submandibular gland) and level IIA (parotid tail). While placing salivary lesions on the differential diagnosis of a neck mass, it is important to understand that incisional biopsies of such neck masses have no role to play in their management. It is therefore essential that surgeons rely on available preoperative measures, including the development of a comprehensive and orderly differential diagnosis, obtaining structural imaging studies, and performing a fine-needle aspiration biopsy as indicated so as to execute the proper surgical treatment plan. This article reviews salient features and the surgical management of the most commonly encountered salivary lesions of the neck, including the plunging ranula and submandibular gland mucocele, the parotid tail tumor, the submandibular gland tumor, and sialadenitis/sialolithiasis of the submandibular gland.
Plunging ranula and submandibular gland mucocele
Most ranulas of the floor of mouth are large extravasation mucoceles that arise from the sublingual gland and are lined by granulation tissue rather than epithelium. The ranula was first described in the sixteenth century and its curative surgical treatment was subsequently discussed in the seventeenth century. The exact tissue of origin of the ranula was elucidated in the nineteenth century, and its pathophysiologic mechanism was first clearly described in 1956. A lengthy treatise on the surgical management of the ranula with sublingual gland excision was published in 1969. Clinical observation shows that some ranulas may descend into the submandibular triangle through a posteriorly located mylohyoid hiatus, or a herniation in the mylohyoid muscle, and are therefore referred to as plunging ranulas. Such plunging ranulas develop discrete neck masses that are appreciated on physical examination. Some investigators have indicated that repeated aspirations or conservative drainage procedures of oral ranulas encourage the development of scar tissue in the mucosa of the floor of mouth such that a plunging ranula develops in the neck as the path of least resistance. The anatomy of the mylohyoid muscle and its hiatus or cleft, and herniations within the mylohyoid muscle, have been studied to explain the development of plunging ranulas. In their study of 23 adult cadavers, Harrison and colleagues identified that a bilateral mylohyoid hiatus existed in 10 of their 23 specimens (43%), with the hiatus being unilateral in 6 (26%) and bilateral in 4 (17%) cadavers. The median anteroposterior dimension of the hiatus was 7 mm, with a range of 2 to 11 mm, and the median mediolateral dimension was 14 mm with a range of 7 to 20 mm. The investigators identified sublingual gland tissue in 9 hernias and fat in 6 hernias.
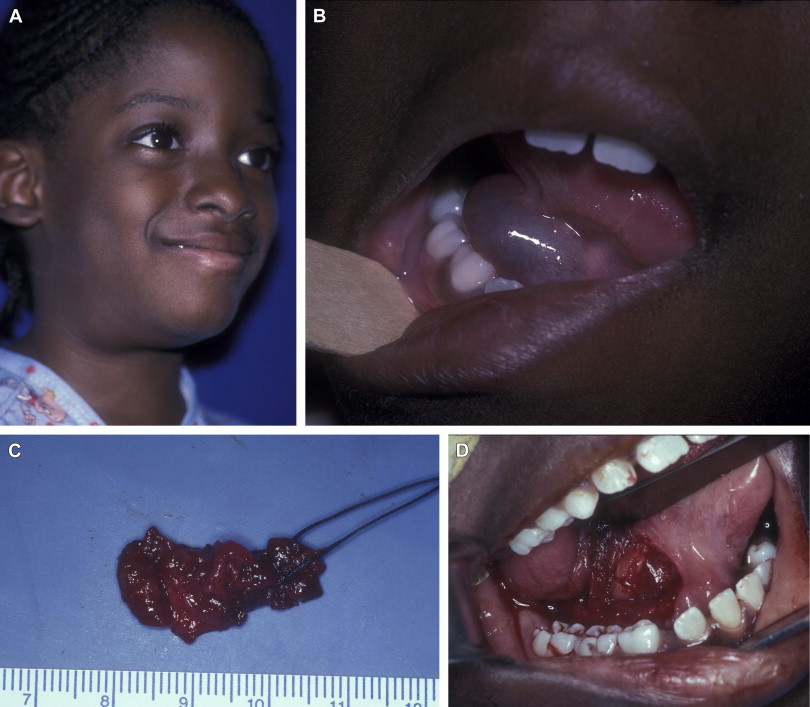
Although the diagnosis of the conventional, nonplunging ranula remains straightforward, its management has historically been variable and controversial, ranging from incision and marsupialization to sublingual gland excision. Most mucoceles are located in the lower lip and are treated with an excision of the mucocele and associated causal minor salivary gland tissue of the lower lip. Although the ranula of the floor of mouth is the second most common type of mucocele, removal of the ranula and the associated salivary gland (in this case, the sublingual gland) has not been uniformly accepted as standard treatment of the ranula as it is for the lower lip mucocele. The management of the plunging ranula has also been variably described, ranging from sclerotherapy to excision of the sublingual gland with or without ranula excision/submandibular gland excision. Excision of the etiologic sublingual gland with or without removal of the plunging ranula represents curative treatment in most cases ( Fig. 1 ). A thorough knowledge of floor of mouth anatomy and its precise surgical dissection results in an uncomplicated surgical procedure and expedient cure of the plunging ranula. In terms of the specific dissection of the floor of mouth, the inferior surface of the sublingual gland is carefully separated from the underlying Wharton duct while the posterior-lateral surface of the gland is separated from the lingual nerve. The identification of these structures and their careful dissection is associated with little morbidity when performing this surgical procedure. Any procedure less than excision of all or part of the sublingual gland is speculative in terms of a curative result of this diagnosis.

Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


