Figure 2.30 Anterior open bite developed during the last 6 months due to bilateral TMJ cartilage and bone tissue destruction by rheumatoid arthritis.
C. Medical History
- Rheumatoid factor (RF)-positive and anti-citrullinated antibodies (ACPA)-positive rheumatoid arthritis diagnosed 3 years ago, but symptoms from the fingers since 6 years ago. Joint areas most affected: fingers, feet, and wrists.
- Systemic inflammatory activity: in general low the last 2 years after beginning current medication regime. Before that, high systemic inflammatory activity as assessed by inflammatory markers in blood (ESR, CRP, RF, and ACPA).
- The systemic inflammatory activity increased dramatically during 2 months a year ago, with increased pain in most joints, when the patient had to stop medication due to a severe bronchitis. The patient restarted medication after that and the systemic inflammatory activity returned to low.
- Previous smoker, stopped 4 years ago.
- Medication: methotrexate, Humira® and Folacin®.
D. Psychosocial History
- Married, two children (8 and 12 years of age).
- Works 80% as a secretary. Few sick-leave days in general. Enjoys work and home life very much. Spends as much time as possible together with the family. Likes travel, cycling, and walks.
- Describes herself as a stable person. Normal scores for depression (PHQ-9) and anxiety (GAD-7). Some physical symptoms (PHQ-15), but low level of stress (PSS-10). Good sleep quality (PSQI).
- GCPS grade I; that is, low pain intensity, low disability.
- No smoking, almost no alcohol consumption.
E. Previous Consultations and Treatments
- Her rheumatologist has treated her the last 3 years, since diagnosis, regarding her rheumatoid arthritis in general. Treatment has included pharmacology, physiotherapy, and counselling. No specific treatment of the TMJ.
- Regular annual visits to her dentist, but no specific assessment or treatment of the TMJ.
F. Extraoral Status
Asymmetries
- No apparent swelling or other facial asymmetries. No redness.
Somatosensory abnormalities
- Normal findings regarding touch, cold, and pinprick, except for extraoral cold hypersensitivity in the left maxillary branch of the trigeminal nerve.
Temporomandibular joint
- Bilateral and TMJ familiar pain on mouth opening, laterotrusion to the left, and on protrusion.
- Bilateral familiar palpation pain.
- Bilateral reduced translatory movement.
- Palpable crepitus from both TMJs.
Masticatory muscles
- Bilateral and familiar palpation pain masseter and temporal muscles. No referred pain.
- No masticatory muscle pain on mandibular movement.
Jaw movement capacity
- Maximum mouth opening without pain is 15 mm, maximum unassisted opening is 28 mm, and maximum assisted mouth opening is 45 mm.
- Right laterotrusion 10 mm, left laterotrusion 9 mm, and protrusion 8 mm.
Neck examination
- Normal range of motion, familiar neck pain on movement or palpation but no spreading of the pain toward the orofacial region.
G. Intraoral Status
Soft tissues
- Normal.
Hard tissues and dentition
- Complete dentition with few and minor fillings (Figure 2.30).
Occlusion
- Dentition: 17–27, 37–47. Hard occlusion shows contacts on the following teeth in the upper jaw: 17, 16, 26, 27 (Figure 2.30).
H. Additional Examinations and Findings
- The occlusal changes motivate a radiographic examination. The purpose would be to identify structural changes due to an inflammatory processes in both TMJs that may explain the anterior open bite and signs of ongoing inflammatory activity.
- The radiographic examination was performed by a radiologist using a bilateral CBCT of both TMJs. This examination showed substantial structural changes in both TMJs with signs of condylar erosions and loss of compact bone on both condyles, bilateral condyle bone loss, condylar flattening, and sclerosis, as well as bilateral osteophytes (Figure 2.31).
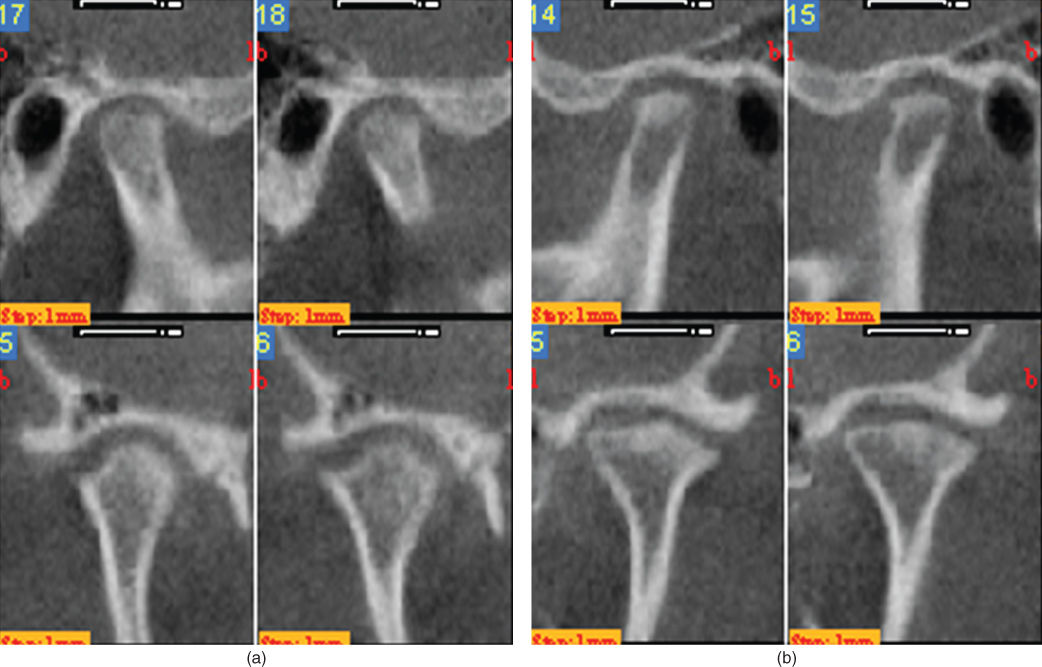
Figure 2.31 Bilateral CBCT of the TMJs showed substantial structural changes in right (a) and left (b) TMJs with signs of condylar erosions and loss of compact bone on both condyles, bilateral condyle bone loss, condylar flattening, and sclerosis, as well as bilateral osteophytes.
I. Diagnosis/Diagnoses
Expanded DC/TMD
- Systemic arthritides.
- Bilateral TMJ arthritis.
DC/TMD
- Myalgia of the masticatory muscles.
J. Case Assessment
- Most probably a bilateral TMJ involvement of rheumatoid arthritis causing TMJ arthritis with pain and tissue destruction. In turn, this has limited the patient’s possibility to enjoy food and reduced her chewing capacity.
- Bilateral TMJ crepitus as well as bilateral radiographic signs of structural changes in accordance with TMJ rheumatoid arthritis and with signs of probable ongoing inflammatory activity (erosions, loss of compact bone).
- There are no indications of other factors that may have caused the bilateral TMJ arthritis.
- Very low psychosocial factors.
- The patient also had myalgia in the masticatory muscles. Myalgia is a common finding in rheumatoid arthritis, especially close to the joints. This seems to be the case also for the TMJ and masticatory muscles. There are no other indications of a muscle tension problem.
K. Evidence-based Treatment Plan including Aims
- The main problem is the bilateral TMJ arthritis due to rheumatoid arthritis. The long-term prognosis for the TMJ is highly dependent on the systemic treatment and the systemic inflammatory activity. It is, however, not uncommon with one or a few joints with active inflammation despite an appropriate systemic medication and in general low systemic inflammatory activity. Our findings and assessment must therefore be communicated with the rheumatologist.
- The initial treatment should be anti-inflammatory with the goal to stop the inflammatory activity in both TMJs. For this, intraarticular corticosteroids are highly indicated. As always, pharmacological anti-inflammatory treatment has to be combined with a treatment modality that has the possibility to reduce the risk of a relapse of the arthritis (e.g., jaw exercise, splint).
- Initial treatment: anti-inflammatory treatment of both TMJs. Treatment options range from intraarticular corticosteroids, NSAIDs per os, de-loading of the joint (splint), and jaw exercise (Kopp and Wennerberg, 1981; Fredriksson et al., 2006).
- When the inflammatory activity is substantially reduced and under control, the occlusal changes should be addressed. The aim for this part should be adequate chewing ability and stable, comfortable occlusion, but only if the patient still experience such problems. Sometimes, the occlusion can normalize by itself in about 2 months if the inflammatory activity in the TMJ can be inhibited properly.
L. Prognosis and Discussion
- The prognosis is very much dependent on how well it will be possible to stop the inflammatory activity and her systemic inflammatory activity.
- The patient is RF-positive and ACPA-positive, which are two strong negative prognostic factors. However, the short-term prognosis for treatment of arthritis must be considered as good.
- The long-term prognosis is unclear and depends to a great extent on how well the systemic inflammatory activity can be controlled by her systemic treatment.
Background Information
- Rheumatoid arthritis is a chronic, autoimmune, autoinflammatory, progressive disorder that can affect and damage joints, but also other tissues. In some people, the condition also can damage a wide variety of body systems, including the skin, eyes, lungs, heart, and blood vessels.
- The worldwide prevalence of rheumatoid arthritis is 0.8–1.2%, with a higher prevalence in the Western Hemisphere. The TMJ is involved in 30–50% of patients with rheumatoid arthritis.
- An autoimmune and autoinflammatory disorder, rheumatoid arthritis occurs when the immune system mistakenly attacks the body’s own tissues. In turn, this causes a strong immune system reaction, including inflammation, in the synovial membranes in the joints.
- This reaction usually causes an intraarticular inflammatory milieu that can eventually result in pain (especially during joint movement and loading), cartilage and bone tissue destruction, and joint deformity.
- The inflammation associated with rheumatoid arthritis is what can damage other parts of the body as well.
- While new types of medications have improved treatment options dramatically, severe rheumatoid arthritis can still cause physical disabilities.
- TMJ involvement of rheumatoid arthritis can have a substantial impact on daily activities and quality of life.
(Tegelberg and Kopp, 1987; Hochberg et al., 2010; Doria et al., 2012; Ahmed et al., 2013)
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


