Classification of malocclusions
Lars Bondemark
Key topics
- Normal occlusion and malocclusions
- Discrepancies between the jaws – sagittal, vertical and transversal malocclusions
- Anomalies within the jaws – crowding, spacing, variations in number and malpositions of teeth
- Frequency of malocclusions
- Orthodontic treatment need
Learning objectives
- To be able to distinguish between normal occlusion and malocclusions
- To be able to classify malocclusions between and within the jaws, as well as categorise different malpositions of teeth
- To understand different malocclusions and their frequencies
- To understand what orthodontic treatment need means and what type of malocclusions should or should not be treated
Normal occlusion and malocclusion
Normal, or ideal, occlusion is a concept constructed by the orthodontic profession. More than 100 years ago, Edward H. Angle introduced the first clear and simple definition of normal occlusion:
The upper first molars are the key to occlusion and the upper and lower molars should be related so that the mesiobuccal cusp of the upper molar occludes in the buccal grove of the lower molar. If the teeth are arranged on a smoothly curving line of occlusion and this molar relationship exists, then normal occlusion would result (Angle, 1900).
The opposite condition is malocclusion, which was once defined as:
The nature of malocclusion, not a disease, but rather a variation from accepted societal norm that can lead to functional difficulties or concerns about dento-facial appearance for a patient (Brook and Shaw, 1989).
Deviation from normal or ideal occlusion does not necessarily mean that the malocclusion needs to be treated. Assessment of treatment requirement is based on an evaluation of the risk, short or long term, for disturbances in oral health, function, aesthetics or patient satisfaction.
Usually, an occlusion or malocclusion is classified according to terms of discrepancies between the jaws, for example sagittal (anterior-posterior), vertical and transversal relationships including functional abnormalities between the maxillary and mandibular dental arches. In addition, anomalies within the jaws, for example crowding and spacing, variations in number of teeth and malpositions of teeth are considered. Some malocclusions, for example increased overjet, crowding and spacing. may be classified by range in millimetres. This implies that normal occlusions may have minor variations within a range and so is not a fixed condition. Furthermore, in sagittal, vertical and transversal discrepancies, skeletal deviations can be involved, combining both dental and skeletal discrepancies.
Discrepancies between the jaws
Sagittal plane
In the sagittal classification, the basis for assessment is the intermaxillary positions of the first molars. There exist three characteristics: normal, postnormal (Angle Class II) and prenormal (Angle Class III) occlusion.
Normal occlusion
In a normal sagittal occlusion, also called Angle Class I, the mesio-buccal cusp of the maxillary first molar occludes with the mesio-buccal groove of the mandibular first molar (Figure 2.1). The maxillary canine cusp tip occludes between the mandibular canine and first premolar (Figure 2.1). In principle, deviations of up to half a cusp width in a mesial or distal direction are considered a normal occlusion. The overjet in normal occlusions is usually between 2 and 5 mm. Sometimes the first molars have migrated because of early extraction of primary teeth due to, for example, caries. In such cases, the position of first molars prior to migration has to be estimated, and the intermaxillary canine position can provide guidance (Figure 2.2).

Figure 2.1 Angle Class I occlusion (normal occlusion).

Figure 2.2 Normal sagittal molar relation because of mesial movement of the mandibular molar (arrow). However, the intermaxillary canine relationship indicates a Class II malocclusion, and thus this case shows a Class II malocclusion.
Angle Class II occlusion
In an Angle Class II, or postnormal, occlusion, the mandibular first molar has a posterior position compared with normal occlusion, i.e. behind the normal position or in a distal relationship (Figure 2.3). In about 90% of the Angle Class II occlusions, the maxillary incisors are proclined, i.e. Angle Class II division 1 (Figure 2.4a), while approximately 10% show retroclined maxillary central incisors, i.e. Angle Class II division 2 (Figure 2.4b). In an Angle Class II division 1 occlusion, the overjet is often enlarged, and if the overjet is over 6 mm, it is counted as great, and anything above 9 mm is considered extreme.

Figure 2.3 Angle Class II malocclusion (postnormal occlusion).

Figure 2.4 Angle Class II division 1 malocclusion (a) with proclined maxillary incisors (red line in a), and Angle Class II division 2 malocclusion (b) with retroclined maxillary central incisors (purple line in b).
Angle Class III occlusion
Angle Class III, or prenormal, occlusion is evident when the mandibular first molar is in a prenormal position compared to the normal occlusion, i.e. in front of the normal position, or in a mesial relationship (Figure 2.5). In cases of Angle Class III occlusion, the overjet is often reversed (<0 mm), implying an anterior crossbite.

Figure 2.5 Angle Class III malocclusion (prenormal occlusion).
Vertical plane
Two possibilities are evident: open bite or deep bite.
Open bite
In open bite, there is no intermaxillary tooth contact, either in the front or laterally from the dental arch (Figure 2.6). To qualify as open bite, the overbite is reversed (<0 mm), and the teeth are assumed to be fully erupted.

Figure 2.6 Open bite in the front between the jaws.
Deep bite
Deep bite is defined as an excessive vertical overlap of the incisors, i.e. vertically, where more than two-thirds of the buccal surfaces of the mandibular incisors are covered by the maxillary incisors (Figure 2.7). Most often, the reason for deep bite is an over-eruption of the incisors or an anterior rotation of the mandible. A deep bite occasionally manifests with contact between the edges of the mandibular incisors and the palatal mucosa behind the maxillary incisors (Figure 2.8). In such cases, the contact between incisors and the mucosa may cause tissue ulceration. Therefore, the classification of deep bite includes evaluating whether contact exists between incisors and palatal mucosa and whether ulcerations occur.

Figure 2.7 Deep bite.
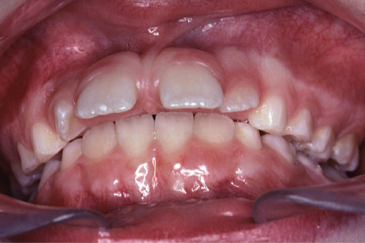
Figure 2.8 A deep bite with contact between the edges of the mandibular incisors and the palatal mucosa behind the maxillary incisors.
Transversal plane
Transversal plane discrepancies relate to the width of the maxilla and/or mandible, and either posterior crossbite or scissors bite can be registered.
Posterior crossbite
In a posterior crossbite, the buccal cusps of the maxillary premolars and/or molars occlude lingually to the buccal cusps of the mandibular premolars and/or molars. The posterior crossbite can be either unilateral or bilateral. Unilateral crossbites of dento-alveolar origin are caused by palatal tipping of the maxillary premolars and molars, and is most often accompanied with a forced guidance of the mandible, thus deviating the midline of the mandible to the crossbite side (Figure 2.9) (Thilander and Myrberg, 1973). The force guidance has to be assessed or diagnosed in a clinical investigation.

Figure 2.9 Unilateral crossbite on the right side of the individual, and there has been a forced guidance of the mandible, deviating the midline to the crossbite side (arrow).
A bilateral crossbite (Figure 2.11) is often caused by a transversal skeletal constriction of the maxilla and without a forced guidance of the mandible.
Scissors bite
In a scissors bite situation, one or more premolars or molars in the maxilla occlude with their lingual cusps buccal to the mandibular buccal cusps of the premolars and/or molars (Figure 2.10). Scissors bite may occur unilaterally or bilaterally and be associated with forced guidance of the mandible, but forced guidance is more infrequent than in posterior crossbites. Bilateral scissors bite is occasionally referred to as the Brodi syndrome.

Figure 2.10 A scissors bite of maxillary left first and second premolar.

Figure 2.11 Bilateral crossbite.
Functional disturbances
When the bite is closing, and if the mandible is guided by an early intermaxillary abnormal contact, the mandible can either move laterally or in a forwards direction. When the mandible is guided laterally, a posterior crossbite is established (Figure 2.9), while if the mandible is forced forwards, an anterior crossbite will be created (Figure 2.12).

Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


