Recognizing a potentially difficult airway is important in avoiding a life-threatening emergency. There are 2 separate scenarios for considering the difficult airway: difficult mask ventilation (DMV) and difficult tracheal intubation (DTI). DMV can be described as lacking the ability to maintain oxygen saturation or lacking the ability to reverse signs of inadequate ventilation with positive-pressure mask ventilation under general anesthesia. DTI remains constant among anesthesia-related patient injuries, and is the third most common respiratory-related episode leading to death and possible brain damage. It is important to preoperatively assess every patient by completing a full history and physical. A thorough history can provide clues in detecting a possible difficult airway. Airway impairment has been further subdivided into the anatomic regions that affect the airway, namely above the larynx, supraglottic, glottic, subglottic, and tracheobronchial. This article discusses the factors that can result in a difficult airway.
The American Society of Anesthesiologists (ASA) has stated there is not a standard definition of the difficult airway in the literature. However, they recognize the difficult airway to be one in “which a conventionally trained anesthesiologist experiences difficulty with face mask ventilation of the upper airway, difficulty with tracheal intubation, or both.” Furthermore, the ASA Difficult Airway Task Force in 2003 defined the following: difficult face mask ventilation, difficult laryngoscopy, and difficult and failed intubations. A difficult face mask ventilation is a situation in which the clinician is unable to provide adequate tidal volumes due to one or more of the following problems: inadequate mask seal, excessive gas leak, or excessive resistance to the ingress or egress of gas. A difficult laryngoscopy is defined as not being able to see any part of the vocal cords with a direct laryngoscopy. A difficult intubation refers to the situation in which multiple intubation attempts are required in the presence or absence of tracheal pathology. Lastly, a failed intubation is defined by multiple attempts whereby the clinician fails to secure the airway. Any of these difficulties can lead to unfavorable outcomes such as hypoxic brain injuries, airway injuries, and even death.
There are 2 separate scenarios for considering the difficult airway. The first is difficult mask ventilation (DMV) and the second, difficult tracheal intubation (DTI). DMV can be clarified as lacking the ability to maintain oxygen saturation (pulse oximetry >92%), or lacking the ability to reverse signs of inadequate ventilation with positive-pressure mask ventilation under general anesthesia. There are several risk factors associated with DMV. These factors include body mass index (calculated as the weight in kilograms divided by height in meters squared) of more than 26 kg/m 2 , the presence of a beard, edentulism, a history of snoring, and an age older than 55 years.
The second category, DTI, remains constant among anesthesia-related patient injuries, and is the third most common respiratory-related episode leading to death and possible brain damage. Many factors are helpful in recognizing a DTI patient, and these predictors include decreased mouth opening, Mallampati classification, restricted head and neck movement, a retrognathic mandible, protrusive maxillary incisors, decreased thyromental distance, decreased sternomental distance, obesity, and a previous history of difficult intubation. The experience of the intubator and the equipment used obviously may play a role in the DTI.
It is worth noting that DMV and DTI can be encountered either together or separately from one another. Rose and Cohen stated that the incidence of DMV is 0.9%, whereas other studies by Asai and colleagues reported 1.4%. One study by Williamson and colleagues showed that the incidence of DMV increased significantly when difficult intubation was encountered, and the incidence rose to 15% in their retrospective study of 2000 reports.
Recognizing a potentially difficult airway is important in avoiding a life-threatening emergency. Therefore, it is critical to preoperatively assess every patient by completing a full history and physical. A thorough history can provide clues in detecting a possible difficult airway. Does the patient have any c-spine pathology that limits their neck’s range of motion? Does the patient have any temporomandibular dysfunction that limits their maximal incisal opening? Has the patient ever been told that he or she was a difficult intubation after undergoing a general anesthetic? These are just some of the basic, but key elements that could provide valuable details of the patient’s history.
A key aspect to the physical examination is the airway assessment, which takes only minutes to complete. This assessment provides crucial information, which could mean the difference between a safe and successful anesthetic and a life-threatening emergency situation. Normal head extension is in the range of 35°. An adult should have a maximal incisal opening of approximately 40 mm, or 2 to 3 fingerbreadths. The patient’s thyromental distance should be evaluated. Anything less than 6 cm might suggest a difficult airway. Mallampati’s classification of the relationship between the size of the base of the tongue, faucal pillars, soft palate, and base of the uvula provides yet another clue. Classes I and II have adequate hypopharyngeal views and typically are easier intubations, whereas classes III and IV tend to be more difficult intubations. Again, these parameters could mean the difference between life and death for a patient undergoing general anesthesia.
It has been estimated that difficult direct laryngoscopy and difficult intubation present anywhere from 1.5% to 8.5% of all airway cases. The reasons why clinicians encounter difficult airways are numerous. The spectrum of reasons ranges from congenital syndromes to malignancies to odontogenic infections, to name but a few. Regardless of the etiology, clinicians must recognize it and prepare for the worst-case scenario. Airway impairment has been further subdivided into the anatomic regions that affect the airway. These classifications were described by Liess and colleagues as above the larynx, supraglottic, glottic, subglottic, and tracheobronchial. The following sections discuss the factors that can result in a difficult airway.
Tumors
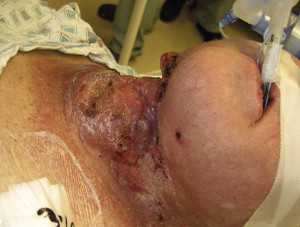
Tumors of the maxillofacial region can present with either a direct or indirect impingement on the airway. A mass may be of significant size and directly make the exchange of oxygen difficult, as it can lead to tracheal deviation, or the tumor itself may be situated on the larynx ( Figs. 1–5 ). As Moorthy and colleagues showed with their clinical experience of 801 cases, patients with laryngeal tumors present an obvious challenge to securing the airway, and therefore it is pertinent that the clinician be extremely prepared and follow a set of guidelines to reduce the number of emergency situations. Second, the impingement can present itself as an adverse outcome from treatment. Following any procedures in the maxillofacial region, a patient is susceptible to developing a hematoma. Whether the hematoma is a result of a resection, fine-needle aspiration, or even placement of a dental implant during the reconstruction phase, a hematoma may lead to a crisis needing immediate intervention (see Fig. 5 ). Patients who undergo surgery for a head and neck tumor may also undergo radiation treatment that could potentially lead to fibrotic scarring of the tissues in the neck. This fibrosis could lead to a reduced range of motion or a distortion in the tissue of the upper airway, both of which could prevent securing an airway.