Case• 45. A white patch on the tongue
SUMMARY
A 52-year-old woman has a white patch on her tongue. Make a diagnosis and decide on appropriate treatment.
History
Complaint
The patient has no complaint.
History of complaint
You have just noticed the lesion in a patient attending for the first time for several years. There is no written record of the white patch in her notes. The patient had noticed the lesion but has ignored it. She thinks it has probably been there for several years.
Medical history
The patient is otherwise fit and well. She smokes 4 cigarettes a day and drinks 4–8 units of alcohol each week.
Examination
Extraoral examination
No lymph nodes are palpable in the neck and there are no abnormal findings on extraoral examination.
Intraoral examination
Apart from this lesion, the remainder of the oral mucosa is normal.
▪ The appearance of the lesion is shown inFigure 45.1. What do you see?
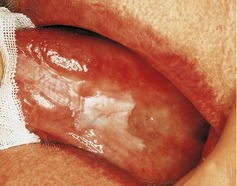 |
| Fig. 45.1 |
There is a flat and homogeneous white patch on the left lateral border and ventral tongue mucosa. It is well defined and varies slightly in whiteness.
If you were able to feel the lesion you would find that it is soft and feels no different from the surrounding mucosa.
Differential diagnosis
▪ What are the common or important white patches in the mouth? How are they caused?
Almost all oral white patches are caused by increased keratinization of the epithelium. Keratin absorbs water and appears white, brighter white where it is thicker. The exception is a chemical burn where the white surface layer is caused by necrosis or ulceration.
| Type of lesion | White lesion(s) |
|---|---|
| Normal mucosal variants |
Leukoedema
Fordyce spots/granules
|
| Inherited epithelial disorders |
White sponge naevus
Pachyonychia congenita
|
| Traumatic lesions |
Frictional keratosis
Chemical burn
Cheek and tongue biting
|
| Infections |
Thrush (acute hyperplastic candidosis)
Chronic hyperplastic candidosis (candidal ‘leukoplakia’)
Chronic mucocutaneous candidosis
Hairy leukoplakia
Syphilitic leukoplakia
|
| Lichen planus and similar conditions |
Lichen planus
Lichenoid reaction (topical and systemic)
Lupus erythematosus
|
| Unknown or smoking-related |
ldiopathic keratosis (leukoplakia), including:
Homogeneous leukoplakia
Verrucous/nodular leukoplakia
Sublingual keratosis
Smoker’s keratosis
Speckled leukoplakia
Stomatitis nicotina (smoker’s palate)
|
| Neoplastic | Squamous cell carcinoma |
Likely diagnoses:
— ldiopathic white patch (leukoplakia)
Sublingual keratosis
Smoker’s keratosis
— Frictional keratosis.
Less likely diagnoses:
— Chronic hyperplastic candidosis
— Lichen planus or lichenoid reaction
— Tongue biting
— Squamous cell carcinoma.
▪ What is a leukoplakia?
The literal meaning of leukoplakia is white patch. The term is correctly defined as a white patch which cannot be characterized as any other lesion. This term can only be used correctly after all possible known causes have been eliminated, using whatever investigations are required. Unfortunately the term leukoplakia is often used very loosely in a clinical context, either for a white patch of any cause or for the small minority of white patches which have a risk of malignant transformation. This has led to great confusion. Now that the term has also been incorporated into the names of several lesions for which the cause is known (such as candidal leukoplakia, hairy leukoplakia and syphilitic leukoplakia) the term has become so inconsistently used as to be unhelpful.
▪ Justify your differential diagnosis.
ldiopathic white patch. Although many causes of well-defined white patches are known, the largest single group is that for which no cause can be identified. This is therefore a likely diagnosis and there are no clinical features which suggest a specific cause for the present lesion. The group of idiopathic white patches includes some more specific terms which might be applied to this lesion.
• Sublingual keratosis is a white patch affecting the floor of the mouth or ventral tongue and lesions here are considered to have a high risk of malignant transformation. The typical lesion is bilateral and may be extensive in the floor of the mouth, often with a wrinkled surface of ‘ebbing tide’ parallel corrugations. However, sublingual keratosis is defined only by its site and any white patch affecting the ventral tongue or floor of mouth could be termed a sublingual keratosis. The present lesion only just extends to the ventral tongue mucosa.
• Smoker’s keratosis is a white patch in the mouth of a smoker for which no other cause can be found. The type of lesion usually called smoker’s keratosis is a flat homogeneous white patch, sometimes with a finely wrinkled surface, on nonkeratinized mucosa. The smoking is assumed to be the cause, though there is rarely any evidence to support this unless the lesion arises where a pipe or cigarette is habitually held. This patient’s lesion could be called a smoker’s keratosis but this is not a particularly useful label and does not imply that it should be treated any differently from an idiopathic white patch. Smoker’s palate (stomatitis nicotina) is a separate condition and is discussed below.
Frictional keratosis is common along the occlusal line, on edentulous alveolar ridges and the lateral tongue. It may be associated with sharp teeth or restoration(s) and be unilateral or bilateral. Frictional keratosis usually merges gradually with the surrounding normal mucosa and is not as sharply defined as the present lesion. Tongue biting also causes keratosis but the surface is often shredded and there may be similar lesions on the buccal mucosa, usually just behind the commissure. Unless lesions are associated with clear evidence of habitual biting, sharp teeth, or resolve on removing a cause, it can be very difficult to identify them from their clinical appearance. Frictional keratosis should be included in the differential diagnosis.
Chronic hyperplastic candidosis causes white plaques, sometimes called candidal leukoplakia. These arise most commonly on the postcommissural buccal mucosa and dorsal tongue and may be associated with red areas. This lesion is more common in smokers. Unless the site is typical it is almost impossible to make the diagnosis clinically. Biopsy or resolution on antifungal treatment are the most useful investigations. The present lesion is not typical, but this cause cannot be confidently excluded on clinical grounds.
Lichen planus and lichenoid reactions may cause homogeneous white patches. This more unusual presentation seems to be more common in smokers and it is not at all clear whether these so-called plaque-type lichen planus lesions are a genuine presentation of lichen planus or are smoking induced. To be sure of the diagnosis it is desirable to find evidence of more typical lichen planus elsewhere, either on the skin, the buccal mucosa or in the form of desquamative gingivitis. There is no evidence to suggest that the current lesion is caused by lichen planus but the plaque type cannot be completely excluded on clinical grounds alone.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


