Internal derangement of the temporomandibular joint (TMJ) is one of the most common temporomandibular disorders. In 1983, Dolwick defined it as an abnormal relation between the temporomandibular disc with respect to the mandibular condyle, the temporal fossa, and the temporal eminence of the TMJ. Anterior disc displacement, with or without reduction, perforation of the retrodiscal tissue or the articular disc, and degenerative changes of the disc and/or the joint surfaces, may be present. Clinically, it may be accompanied by pain, limitation of mouth opening, clicking, and locking. In 1989, Wilkes first established a classification to correlate clinical and radiological signs with surgical findings. The Wilkes classification consists of 5 stages based on clinical, radiologic, and intraoperative findings, varying from a slight forward displacement with symptom-free normal joints to degenerative arthritic changes with severe clinical symptoms. In 1992, with the advent of minimally invasive surgical approaches, Bronstein correlated Wilkes stages with arthroscopic findings.
Different alternatives have been proposed to treat this entity, beginning with conservative approaches. Occlusal splint therapy, medical treatment based on nonsteroidal anti-inflammatory drugs (NSAIDs) and muscle relaxants, and physical treatment are the most common options among conservative methods. Those refractory cases in which no effective improvement in terms of pain and mandibular function is obtained are amenable to further surgical treatment, such as arthroscopic lysis and lavage (ALL) of the superior joint space.
In 1975, Onishi first used an arthroscope in Japan to treat dysfunction of the human TMJ. ALL is the simplest and the most frequently used arthroscopic technique. The term lysis was first used by Sanders in 1986, meaning to sweep with a blunt probe to eliminate the suction cup effect of the disc to the fossa and to lyse adhesions. The technique consists on performing a lysis or the breaking of adherences between the articular surfaces, lavage with abundant serum, and intraoperative mandibular movements or sweeping. In a multicentric study among most experienced centers in the United States, ALL was performed in 85% of almost 5000 arthroscopies of the TMJ.
Macroscopic anatomy of the TMJ
The TMJ is a synovial joint between the temporal bone and the mandibular condyle, which presents both superior and inferior spaces with an interposed disc between them. The superior joint space is cranially limited by an articular surface that covers the articular eminence and the mandibular fossa. Inferiorly, it is limited by the superior surface of the articular disc, and laterally and medially by the synovial membrane. The inferior joint space is limited superiorly by the inferior aspect of the articular disc. The disc is biconcave in shape with a length of approximately 12 mm and a width of 16 mm. It is firmly attached to the lateral and medial poles of the condyle. It is inferiorly limited by the articular surface of the mandibular condyle, and laterally and medially by the synovial membrane. The inferior joint space contains approximately 0.9 mL of synovial fluid, whereas the superior joint space contains approximately 1.2 mL. The lateral pterygoid muscle is inserted in the anteromedial aspect of the TMJ, whereas some muscular fibers insert in the fibrous connective tissue of the anterior aspect of the disc. The lateral aspect of the capsule is reinforced by the lateral ligament, whereas the medial aspect of the capsule is thin and covers a narrow area. The synovial membrane covers the entire inner surface of the TMJ. The retrodiscal tissue attachment consists of synovial cells, collagen fibers, nerves, blood vessels, and elastic fibers.
Functionally, the superior joint space is responsible for gliding or translation motion, whereas the inferior joint space is responsible for hinge opening or rotation. The shape of the synovial membrane around the disc changes during mandibular movements. The elasticity of the retrodiscal tissue and the posterior attachment of the disc allows for these movements. During maximal protrusion, the pterygoid muscle pulls the condyle and disc anteriorly while the posterior band of the disc moves anterior to the peak of the articular eminence. If the muscle contracts on the right, lateral excursion to the left is observed, and vice versa.
Arthroscopic anatomy of the TMJ
Superior Joint Space
Seven areas of the superior joint space can be examined ( Fig. 1 ). These areas are:
- 1.
Medial synovial drape
- 2.
Pterygoid shadow
- 3.
Retrodiscal synovium:
- a.
Zone 1: oblique protuberance
- b.
Zone 2: retrodiscal synovial tissue attached to posterior glenoid process
- c.
Zone 3: lateral recess of retrodiscal synovial tissue
- a.
- 4.
Posterior slope of articular eminence and glenoid fossa
- 5.
Articular disc
- 6.
Intermediate zone
- 7.
Anterior recess:
- a.
Disc synovial crease
- b.
Midportion
- c.
Medial-anterior corner
- d.
Lateral-anterior corner.
- a.
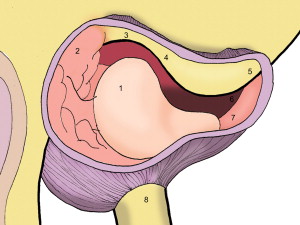
Four classic anatomic landmarks have been described:
- 1.
Medial synovial drape with distinct superior-to-inferior striae
- 2.
Oblique protuberance of the retrodiscal synovium
- 3.
Posterior slope of the articular eminence with distinct anterior-to-posterior striae
- 4.
Anterior disc synovial crease: juncture of anterior synovium and anterior band of disc.
The first area to be arthroscopically examined is the medial synovial drape ( Fig. 2 ), which has a gray-white translucent lining and a tense appearance with distinct superior-to-inferior striae, which serve as the first classic anatomic landmark.
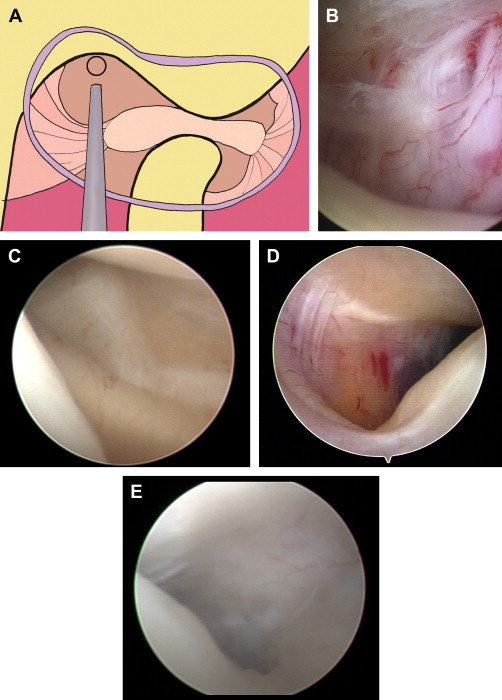
The second area to be examined is the pterygoid shadow ( Fig. 3 ), which is located anterior to the medial synovial drape and frequently well marked. In normal situations, the pterygoid shadow has a purple appearance, because of the pterygoid muscle under the synovial lining.
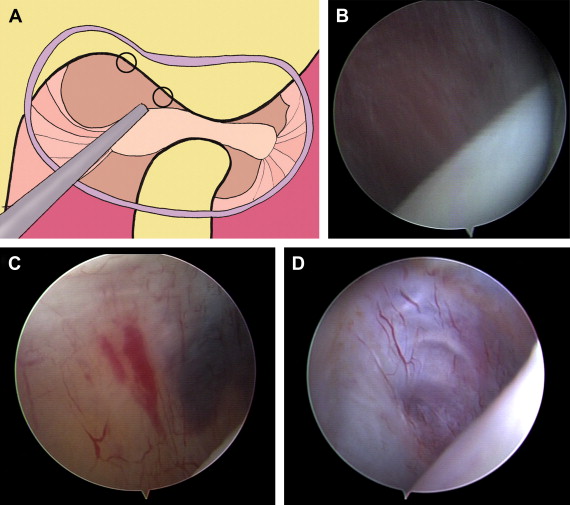
The third area to be examined is the retrodiscal synovium ( Fig. 4 ). A key point within the superior joint space is the synovial membrane with a soft appearance, located in the posterior side of the posterior synovial recess. From the lateral side, several folds on the surface of the synovial membrane appears, and they disappear as long as the disc is displaced anteriorly. The synovial membrane covers the posterior insertion of the disc and is reflected superiorly to the temporal fossa. While the mouth is open, the posterior insertion covered by the synovial lining appears as a crest or crease. This finding is named oblique protuberance. The location of the oblique protuberance is in the middle third of the retrodiscal synovium. The vascular network is observed throughout the normal synovial membrane.
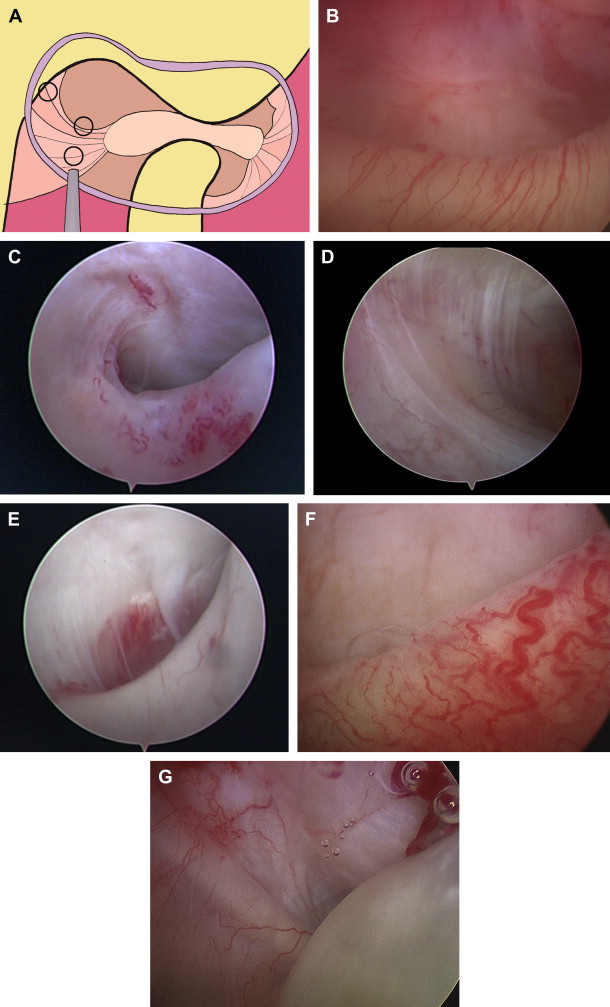
The fourth area of the joint is the posterior slope of the articular eminence ( Fig. 5 ). The fibrocartilage is white and highly reflective with anteroposterior striae. In the back slope of the eminence, the fibrocartilage is thick. Toward the glenoid fossa, the fibrocartilage becomes darker and thinner, and becomes thin without striae over the glenoid fossa.
The articular disc, which is the fifth area to be examined, is milky white, highly reflective, and without striae. In normal conditions, its surface is smooth and without fibrillations. The red-white line is the union between the posterior band of the disc and the synovium ( Fig. 6 A, B). From a posterolateral position of the arthroscope, the disc mobility is examined by smooth movements of the condyle forward and backward. Normally, the disc glides fluently along the articular eminence. The concept of roofing evaluates the covering of the articular disc over the condyle. Roofing is graded arthroscopically according to the posterior band of the articular disc and its position relative to the articular eminence. When it is measured with the condyle forward, the disc is in normal position (roofing 100%) if the posterior band of the disc is lying adjacent to the posterior slope of the articular eminence. With the condyle seated, it is 100% roofed if the posterior band of the disc abuts at approximately the midportion of the glenoid fossa (see Fig. 6 C).
The intermediate zone is the sixth area to be examined ( Fig. 7 ). Without disorders, this area has a white-on-white appearance and the concavity of the disc can be observed.
The anterior recess ( Fig. 8 ) is the seventh area to be examined. It begins with the condyle seated. In this area, the anterior disc synovial crease, which is the fourth classic anatomic landmark, is identified. At the anterolateral site, the union between the lateral synovial capsule and the anterior disc synovial crease can be observed, and this is the ideal place for insertion of the second or working cannula.




