Introduction
The goals of this study were to evaluate (1) the reliability and accuracy of cone-beam computed tomography (CBCT) for assessing adenoid size compared with nasoendoscopy and (2) the influence of clinical experience on CBCT diagnosis.
Methods
Adenoid size was graded on a 4-point scale for CBCT and nasoendoscopy by a pediatric otolaryngologist. Reliability was assessed with intraobserver and interobserver agreement. Accuracy was assessed with agreement between CBCT and nasoendoscopy, plus sensitivity and specificity analyses. The CBCT assessments were completed by a team of 4 evaluators: an oral and maxillofacial radiologist, an airway orthodontist who participates in the multidisciplinary team, an academic orthodontist whose primary research is in 3-dimensional imaging, and a highly experienced private practice orthodontist comfortable with CBCT imaging. Each evaluator was specifically chosen to represent a unique set of clinical and radiographic experiences. All evaluators were blinded to the subject’s identity and clinical history, and they evaluated the images in a unique random order and evaluated each image 3 times separated by a minimum of 7 days. The same computer hardware and software were used.
Results
Thirty-nine consecutively assessed, nonsyndromic subjects (ages, 11.5 ± 2.8 years) were evaluated. The CBCT demonstrated excellent sensitivity (88%) and specificity (93%), strong accuracy (ICC, 0.80; 95% CI, ± 0.15), and good reliability, both within observers (ICC, 0.85; 95% CI, ± 0.08) and between observers (ICC, 0.84; 95% CI, ± 0.08). The clinical experience of the CBCT evaluator did not have a statistically significant effect.
Conclusions
CBCT is a reliable and accurate tool for identifying adenoid hypertrophy.
Highlights
- •
Cone-beam computed tomography images are accurate for evaluating adenoid size compared with nasoendoscopy (ICC, 0.80; 95% CI, ± 0.15).
- •
Cone-beam computed tomography evaluations are reliable between repeated evaluations from 1 person (intraobserver ICC, 0.85; 95% CI, ± 0.08) and among several observers (interobserver ICC, 0.836; 95% CI, ± 0.084).
- •
Cone-beam computed tomography can accurately identify clinically relevant adenoid hypertrophy with 88% sensitivity and 93% specificity.
- •
In the hands of orthodontists trained to look at adenoid size in relation to postnasal space, cone-beam computed tomography approaches the accuracy and reliability of nasoendoscopy.
Adenoid hypertrophy is a common etiology of nasopharyngeal obstruction. Nasopharyngeal obstruction has been associated with mouth breathing and sleep disordered breathing. Both mouth breathing and sleep disordered breathing are significant conditions that orthodontists should be prepared to identify and collaboratively manage with a pediatric otolaryngologist.
Mouth breathing has been proposed as a significant factor for altered craniofacial growth. The description of this pattern includes narrow maxillary arch, posterior crossbite, long face height with clockwise mandibular growth rotation, anterior open bite, and mandibular retrognathia. Each of these anatomic presentations is considered an esthetic or a functional indication for orthodontic treatment and can be ameliorated by early intervention.
Sleep disordered breathing can cause systemic problems such as reduced systemic growth, systemic hypertension, pulmonary hypertension that might cause right or left ventricular hypertrophy, hyperactivity and attention deficit, aggression, and reduced grades in school.
Diagnosis of upper airway dysfunction starts with the clinical history: chronic snoring, breathing interruption during sleep, sleep bruxism, slower growth rate, tendency to fall asleep during the day, behavioral difficulties, and chronic runny nose. The current reference standard for assessing the patency of the nasal cavity and nasopharynx is nasoendoscopy (NE) with a standardized grading system for evaluation. However, NE must be conducted by a otolaryngologist and is outside the scope of orthodontic practice.
Traditionally, orthodontists have used lateral cephalograms to supplement their clinical evaluations of hypertrophic adenoids. However, a previous systematic review could not identify a highly reliable 2-dimensional assessment of the adenoids from a lateral cephalogram, whereas a recent systematic review concluded that lateral cephalograms have only a fair diagnostic value for adenoid evaluation. It was recommended that orthodontists should seek an alternative low-risk, simple, and valid diagnostic tool to better screen for potential upper airway constriction.
Cone-beam computerized tomography (CBCT) provides a comparatively low-cost, easily accessible, and relatively low-radiation 3-dimensional (3D) evaluation of craniofacial structures and is increasingly being used for diagnosis and treatment planning of more complicated orthodontic cases. In phantom studies, CBCT volumetric measurement errors have been reported from 0% to 5% compared with known physical airway phantoms. In vivo, the dimensions of the nasopharyngeal airway in CBCT imaging are highly comparable with those from multirow detector computed tomography ; however, recent systematic reviews have suggested that further work is needed to confirm the validity of CBCT airway assessments. Although preliminary investigations of adenoid hypertrophy with CBCT are promising, clinically relevant interpretation of CBCT diagnosis has not yet been validated against an accepted reference standard.
NE is the accepted reference standard and the primary method that an otolaryngologist will use to determine adenoid hypertrophy management. Therefore, the clinical usefulness of CBCT imaging for evaluating hypertrophic adenoids should be determined by comparing it with NE with a similar diagnostic scale used by otolaryngologists. The objective of our study was to evaluate the accuracy and reliability of CBCT imaging for evaluating adenoid obstruction by comparing CBCT diagnosis with NE diagnosis on a 4-point scale.
Material and methods
CBCT diagnostic efficacy for adenoid hypertrophy was evaluated with a prospective cross-sectional agreement study. Protocol approval was granted by the appropriate ethics committee. The subjects were recruited from a tertiary referral center, a multidisciplinary upper airway dysfunction clinic.
The inclusion criteria were (1) male and female patients aged 6 to 15 years; this age range was chosen because it represents ages typically seen in orthodontic practices, and during this age range orthodontic interventions can impact airway function (eg, rapid maxillary expansion); and (2) orthodontic patients with upper airway concerns or ear, nose, and throat patients with suspected orthodontic or craniofacial development concerns.
The exclusion criteria were (1) subjects with confirmed syndromes or neurologic disorders and (2) subjects with any previous treatment for airway obstruction.
Recruitment began in September 2011 and continued until October 2012. The sample size was not determined a priori, but the goal was to include as many participants as possible in the defined period. All consecutively evaluated patients meeting the criteria were included in the study. By recruiting subjects evenly throughout an entire calendar year, the effects of confounders such as seasonal allergies were most likely accounted for.
At the examinations, an orthodontist (M.P.M.) and an otolaryngologist (H.E.) assessed all patients on the same day, each using CBCT imaging and NE, respectively. CBCT images were taken for orthodontic diagnosis, not singularly for adenoid evaluation. Because many subjects had complex craniofacial problems (transverse, vertical, and anteroposterior concerns), CBCT imaging was obtained instead of panoramic radiographs, lateral cephalograms, and posteroanterior cephalograms. Evaluations were postponed for any subject experiencing acute nasal symptoms, such as a cold or an active allergy flare-up, to ensure accurate baseline assessments.
NE was performed in the upright position using a 2.2-mm flexible tube endoscope (vs rigid endoscopy). In addition to nasal and adenoid evaluations, the endoscope was passed beyond the adenoids into the oropharynx to view the epiglottis. Topical decongestion (0.05% xylometazoline) and anesthesia (4% lidocaine) were applied using a cotton-tipped applicator. The examinations were prospectively recorded on a digital image-capturing unit and electronically archived. The otolaryngologist documented the size of the adenoids and other findings using a patient information sheet. This formed the basis for dictation of the clinical data in a standard format.
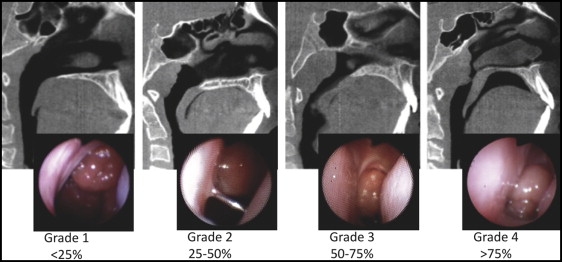
The severity of adenoid obstruction was evaluated on the video endoscopy images using a previously validated subjective 4-point scale. In the 4-point scale, grade 1 is less than 25% obstruction, grade 2 is 25% to 50% obstruction, grade 3 is 50% to 75% obstruction, and grade 4 is more than 75% obstruction ( Fig 1 ). When a report was not clear regarding adenoid size classification, the archived NE video documentation was reevaluated to clarify the diagnosis.
CBCT images were taken in the upright position with a 12-in field of view, 300-μm voxel, and a scan time of 8.9 seconds. These images were acquired within 2 to 3 hours after the NE; the decongestant delivered by the otolaryngologist was still effective during the CBCT evaluation, thus ensuring consistency of the nasal tissues during evaluation.
All CBCT images were coded and blinded for randomized prospective evaluation. An independent consultant retained the code’s key until all evaluations were complete. The severity of adenoid obstruction was evaluated on the CBCT images using the same 4-grade scale as for the NE evaluation. Specifically on the CBCT images, adenoid size was evaluated using slices in all 3 planes of space (as opposed to 3D volume rendering), allowing the evaluator to freely scroll through any plane he or she wished to use. The midsagittal slice was used as the starting point of assessment and frequently provided the most diagnostically useful information, but in the final diagnosis slices from the axial and coronal planes were considered as well. All DICOM visualizations were made using OsiriX 64-bit imaging software (OsiriX, Geneva, Switzerland).
CBCT assessments were completed by a team of 4 evaluators: an oral and maxillofacial radiologist, an airway orthodontist (M.P.M.) who participates in the multidisciplinary team, an academic orthodontist whose primary research is in 3D imaging, and a highly experienced private practice orthodontist comfortable with CBCT imaging. Each evaluator was specifically chosen to represent a unique set of clinical and radiographic experiences. All evaluators were blinded to the subjects’ identities and clinical history; they evaluated the images in a unique random order and evaluated each image 3 times separated by a minimum of 7 days. All evaluators reviewed the CBCT images using the same computer hardware and software.
Statistical analysis
The accuracy of CBCT images for diagnosing adenoid obstruction was statistically analyzed in 2 ways. First, agreement between CBCT and NE was evaluated using intraclass correlation coefficient (ICC) statistics based on the 4-point grading system; 95% confidence intervals (CIs) were calculated for all ICC values. Second, the 4-point scale was converted to a binary diagnosis of “yes” or “no” for adenoid hypertrophy. Two-by-two contingency tables for each observer were generated and used to compute sensitivity and specificity. Patients classified as moderate or severe (grades 3 or 4) were considered positively diagnosed with adenoid obstruction.
The reliability of CBCT imaging was determined by quantifying the level of agreement among the 4 evaluators’ assessments. ICC statistics were calculated to quantify intraobserver and interobserver agreement. ICC statistics were computed with the SPSS software package (version 20.0; IBM, Armonk, NY).
Results
In total, 39 consecutively evaluated subjects between the ages of 6.3 and 15.8 years (mean, 11.5 ± 2.8 years) were assessed. With NE, 17 subjects were diagnosed with grade 1 adenoids, 10 subjects with grade 2, 7 subjects with grade 3, and 5 subjects with grade 4 ( Fig 1 ; Table I ). This distribution equated to 12 subjects with clinically significant adenoid hypertrophy, whereas 27 were considered healthy. Intraobserver and interobserver reliabilities were not evaluated for NE.
| NE-1 | NE-2 | NE-3 | NE-4 | |
|---|---|---|---|---|
| CBCT-1 | 54 | 17 | 3 | 0 |
| CBCT-2 | 11 | 17 | 4 | 0 |
| CBCT-3 | 1 | 2 | 11 | 5 |
| CBCT-4 | 1 | 4 | 11 | 15 |
The reliability of repeated CBCT evaluations (intraobserver agreement) on the 4-point scale demonstrated very good agreement ( Table II ). The maxillofacial radiologist, academic 3D orthodontist, and airway orthodontist had very good intraobserver agreement: ie, all were consistent between repeated evaluations (ICC, 0.813-0.819; 95% CI, ± 0.137-0.142). The private practice orthodontist had good intraobserver agreement (ICC, 0.740; 95% CI, ± 0.134). While the private practice orthodontist seemed less accurate than the other evaluators, there was no statistical difference, since the 95% CI values for all evaluators overlapped ( Fig 2 ), although the lower boundary of the 95% CI was only 0.606. Beyond intraobserver agreement, strong interobserver agreement (between observers) further supported CBCT as reliable for adenoid screening (ICC, 0.836; 95% CI, ± 0.084).
| Agreement between repeated CBCT evaluations (ICC ± 95% CI) | |
|---|---|
| Maxillofacial radiologist | 0.886 ± 0.070 |
| Airway orthodontist | 0.892 ± 0.067 |
| Academic 3D orthodontist | 0.896 ± 0.065 |
| Private practice orthodontist | 0.740 ± 0.134 |
| Average intraobserver agreement | 0.85 ± 0.08 |
| Overall interobserver agreement | 0.836 ± 0.084 |
The accuracy of the CBCT evaluations (agreement between CBCT with NE evaluations) was also strong across evaluators (ICC, 0.743-0.819; Table III ). Although the private practice orthodontist again had the lowest level of CBCT agreement with NE (ICC, 0.743; 95% CI, ± 0.183), the 95% CI values of all evaluators comfortably overlapped ( Fig 3 ).
| Agreement between CBCT and NE evaluations (ICC ± 95% CI) | |
|---|---|
| Maxillofacial radiologist | 0.813 ± 0.140 |
| Airway orthodontist | 0.814 ± 0.142 |
| Academic 3D orthodontist | 0.819 ± 0.137 |
| Private practice orthodontist | 0.743 ± 0.183 |
| Average | 0.80 ± 0.15 |
When the evaluations were transformed into clinically relevant binary diagnoses of diseased vs healthy ( Table IV ), the sensitivity and specificity of CBCT imaging for evaluating adenoid hypertrophy was excellent ( Table V ). All evaluators achieved sensitivity values of 83% or more, and specificity values of 88% or better were demonstrated. By the group of evaluators, the CBCT demonstrated 88% sensitivity and 93% specificity for identifying clinically relevant adenoid hypertrophy.
| NE (+) | NE (−) | |
|---|---|---|
| Radiologist | ||
| CBCT (+) | 10 | 2 |
| CBCT (−) | 2 | 25 |
| Airway orthodontist | ||
| CBCT (+) | 10 | 1 |
| CBCT (−) | 2 | 26 |
| Academic 3D orthodontist | ||
| CBCT (+) | 11 | 2 |
| CBCT (−) | 1 | 25 |
| Private practice orthodontist | ||
| CBCT (+) | 11 | 2 |
| CBCT (−) | 1 | 24 |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


