Introduction
Our aim was to compare the time required to complete the alignment of crowded maxillary anterior teeth (canine to canine) between Damon MX (Ormco, Glendora, Calif) and In-Ovation R (GAC, Central Islip, NY) self-ligating brackets.
Methods
Seventy patients from the first author’s office were included in this randomized controlled trial by using the following inclusion criteria: nonextraction treatment on both arches, eruption of all maxillary teeth, no spaces in the maxillary arch, no high canines, maxillary irregularity index greater than 4 mm, and no therapeutic intervention planned involving intermaxillary or other intraoral or extraoral appliances including elastics, maxillary expansion appliances, or headgear. The patients were randomized into 2 groups: the first received a Damon MX bracket; the second was bonded with an In-Ovation R appliance, both with a 0.022-in slot. The amount of crowding of the maxillary anterior dentition was assessed by using the irregularity index. The number of days required to completely alleviate the maxillary anterior crowding in the 2 groups was investigated with statistical methods for survival analysis, and alignment rate ratios for appliance type and crowding level were calculated with the Cox proportional hazard regression. An analysis of each protocol was performed.
Results
No difference in crowding alleviation was found between the 2 bracket systems. Higher irregularity index values were associated with the increased probability of delayed resolving of crowding.
Conclusions
The use of passive or active self-ligating brackets does not seem to affect treatment duration for alleviating initial crowding.
The last decade has witnessed unprecedented progress in the development of new appliances with alternative ligating features. Passive and active self-ligating appliances with many ligating mechanisms were introduced to presumably allow for efficient sliding mechanics. This feature was linked with several presumed effects including lower forces and moments and higher rates of tooth movement, because of the reduced friction and absence of binding of ligatures on wire. Nonetheless, for most of these appliances, there is little evidence about the characteristics and capabilities claimed by the manufacturers, and, in some cases, it seems that marketing-derived principles rather than scientific evidence is used to substantiate their well-advertised clinical performance. Thus, the resultant turmoil in this specialty has no support in the literature, since most published trials do not show superior efficiency of self-ligating brackets regardless of type or ligating mechanism.
The available evidence on the efficiency of self-ligating brackets derives from a few prospective and randomized clinical trials, with most prospective and randomized controlled trials (RCTs) demonstrating no difference in treatment duration between conventional and self-ligating brackets.
Recently, the relatively low validity and reliability of retrospective studies as opposed to prospective and especially RCTs have switched investigators’ interests to the latter type of studies. RCTs are preferred because of the elimination of selection and outcome biases of retrospective studies. Currently, there is little evidence from this type of study on the potential differences between passive and active self-ligating brackets in tooth movement rates.
The purpose of this study was to compare the time required to complete the alignment of crowded maxillary anterior teeth (canine to canine) between passive and active self-ligating brackets.
Material and methods
Seventy patients were included in this RCT, selected from a large pool of patients from the first author’s office. The following inclusion criteria were used: nonextraction treatment in both arches, eruption of all maxillary teeth, no spaces in the maxillary arch, no high canines, maxillary irregularity index greater than 4 mm, and no therapeutic intervention planned involving intermaxillary or other intraoral or extraoral appliances including elastics, maxillary expansion appliances, or headgear. The patients were selected and treated between March 2007 and May 2009. Their demographics are shown in Table I .
| Total (n = 70) mean or % | SD | Damon MX (n = 35) mean or % | SD | In-Ovation R (n = 35) mean or % | SD | P value ∗ | |
|---|---|---|---|---|---|---|---|
| Demographic characteristics | |||||||
| Age (y) | 13.8 | 1.8 | 13.8 | 1.8 | 13.8 | 1.7 | NS |
| Sex (%) | |||||||
| Girls | 58.6 | 60.0 | 57.0 | NS | |||
| Boys | 41.4 | 40.0 | 43.0 | ||||
| Clinical characteristics | |||||||
| Crowding (irregularity index, mm) | 7.5 | 2.1 | 8.0 | 2.1 | 7.0 | 2.0 | NS |
| Angle class (%) | |||||||
| I | 48.6 | 51.4 | 45.7 | NS | |||
| II | 47.1 | 42.9 | 51.4 | ||||
| III | 4.3 | 5.7 | 2.9 |
∗ P value for comparison of group means by t test or differences in proportions by chi-square test and Fisher exact test.
The active self-ligating group was bonded with the Roth prescription In-Ovation R bracket (GAC, Central Islip, NY), and the passive self-ligating group received the high-torque version of the Damon MX (Ormco, Glendora, Calif), both with a 0.022-in slot. All first and second (when present) molars were bonded with Speed bondable tubes (Speed System Orthodontics, Cambridge, Ontario, Canada). Bracket bonding, archwire placement, and treatment were performed by the first author.
The amount of crowding of the maxillary anterior dentition was assessed by using the irregularity index described by Little. Measurements were made twice on the initial casts by the first author with a digital caliper (Digimatic NTD12-6”C, Mitutoyo, Tokyo, Japan).
Archwire sequence was the same for both treatment groups: 0.014-in Damon arch form copper-nickel-titanium 35°C (Ormco), followed by a 0.016 × 0.025-in Damon arch form copper-nickel-titanium 35°C (Ormco).
Seventy patients (mean age, 13.8 years) were randomized to either an active or a passive self-ligating appliance. Randomization was accomplished by generating random permuted blocks of variable size; this ensured equal patient distribution between the 2 trial arms. Numbered, opaque, sealed envelopes were prepared before the trial containing the treatment allocation card. After patient selection, the secretary of the practice was responsible for opening the next envelope in sequence.
Based on previous research, it was assumed that a hazard ratio larger than 2 between the bracket groups would be an important clinical finding. Sample size was calculated. Based on this assumption, the required sample size was calculated at 66 (a = 0.05, power = 80%), and it was decided to include 70 subjects in case of any losses.
The date (T1) that each patient was bonded was recorded. All patients were followed monthly. Complete alleviation of crowding was judged clinically by the first author. On visual inspection of correction of proximal contacts, the patient was considered complete, and the alignment date (T2) was determined and recorded on the spreadsheet. Only the alignment of the 6 maxillary anterior teeth was evaluated. In other words, we considered that a patient had reached the T2 stage if the 6 maxillary anterior teeth were aligned, regardless of possible irregularities in posterior segments. The time to alignment (T2 – T1) for each patient was calculated in days. Blinding of outcome assessment was not feasible for this study. To assess the reliability of the method, the irregularity index was remeasured a month later in 20 models, selected randomly, and good agreement was found between the first and the second measurement (ICC >0.95).
Statistical analysis
Demographic and clinical characteristics were investigated with conventional descriptive statistics. Comparisons of these between the 2 appliance groups were conducted with t tests or chi-square tests, depending on the characteristic (parametric or nonparametric). Treatment duration—the time required to resolve crowding in both appliance groups—was investigated with statistical methods for survival analysis; alignment rate ratios for appliance type and crowding level were calculated with the Cox proportional-hazards regression. A 2-tailed P value of 0.05 was considered statistically significant with a 95% confidence interval.
Results
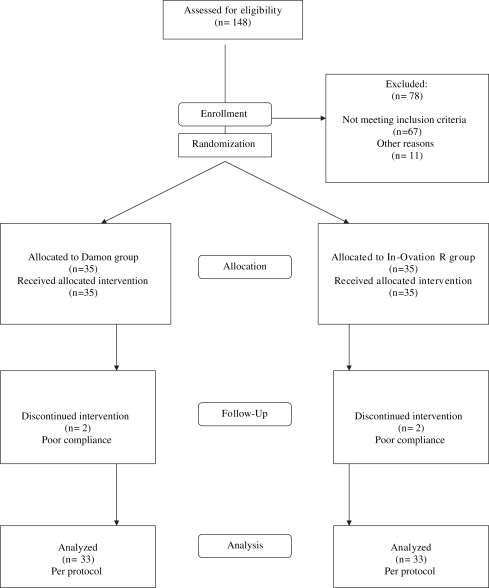
Figure 1 is the CONSORT flowchart. Table I shows the distribution of demographic variables of the groups including age, sex, irregularity index, and Angle classification. There was no discrimination with respect to these factors between the 2 groups, validating the random assignment of appliances to each group. Four patients were excluded from the statistical analysis because of poor compliance, and the statistical analysis was conducted per protocol, since loss to follow-up was not associated with type of treatment.
In Table II , the results of the treatment time to alignment are shown for the 2 bracket groups; no statistical significance was found.
| Total | Mean time to alignment (d) | Minimum (d) | Median (d) | Maximum (d) | P value ∗ | |
|---|---|---|---|---|---|---|
| Wire system | ||||||
| Damon MX | 33 | 107.1 | 56 | 99 | 175 | NS |
| In-Ovation R | 33 | 95.0 | 54 | 92 | 161 | |
| Total | 66 | 101.0 | 54 | 95.5 | 175 |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


