Introduction
Very few studies have addressed long-term development and risks associated with untreated malocclusion. The purpose of this study was to examine changes in occlusion in a lifelong perspective and to compare oral health and attitudes toward teeth among persons with malocclusion with those having normal occlusion.
Methods
In 1950 an epidemiologic survey of 2349 8-year-olds was conducted and included 4 intraoral photographs. Three selected samples with different malocclusions (deep bite, crossbite, or irregular teeth) and 1 sample with normal occlusion (a total of 183 subjects) were, 57 years later, invited for examination and an extensive interview about dental experiences and attitudes. Sixty-nine responded (38%) and constitute the subjects studied.
Results
Malocclusion remained the same or worsened except in subjects having deep bite in childhood, which in some improved and in others became worse. Crowding generally increased. Sixteen persons reported moderate or severe temporomandular joint (TMJ) problems, and of these 7 belonged to the group with crossbite in childhood. With few exceptions, the subjects in all samples had good oral hygiene, visited the dentist regularly, and had well-preserved dentitions. Mean number of missing teeth was significantly lower among those with normal occlusion compared with the malocclusion groups. Individuals with normal occlusion responded favorably to all questions related to attitudes and experiences about their teeth, while responses in the malocclusion groups varied.
Conclusions
Persons with the particular malocclusions examined experienced more problems related to teeth later in life compared with those having normal occlusion in childhood.
A number of longitudinal investigations have examined long-term changes in the occlusion, as these changes are of vital importance for orthodontic treatment planning and the stability of treatment results. Some of these studies address incisor relationship, dental arch crowding, or dental arch dimensions from childhood to adulthood applying metric variables. Most of these studies are, however, based on follow-up of individuals with normal occlusion or only minor malocclusion, and are with very few exceptions not supplemented with information about the examined individual’s own reports of how they perceive these changes.
Another perspective on long-term changes and their impact on the individual relates to the effect of malocclusion on oral health and quality of life. In countries with third-party payment for orthodontic treatment, the funding agencies may question the rationale for treatment of certain malocclusions and request documentation for the need for treatment. For ethical reasons, it is very difficult today to collect data in order to study long-term effects of untreated malocclusion.
Data from an epidemiologic study of malocclusion in 8-year olds from 1950 were available in the archives at the Department of Orthodontics, University of Oslo. From this material, selected patients with specific malocclusions as well as normal occlusion were invited for a follow-up examination. The purpose of the study was to examine long-term changes in occlusion and to compare oral health and attitudes toward teeth among persons with malocclusion in childhood with those having normal occlusion.
Material and methods
In 1950, an epidemiologic study of malocclusion and orthodontic treatment need was conducted and included 2349 of the 2546 first-grade schoolchildren in one county (Hedmark) in Norway. Most of the children were born in 1942, with a few born in 1941 and 1943. Eighty-one morphologic and functional variables were recorded on punch cards. Four standardized intraoral photographs were obtained from each child: the occlusion from the right and left sides and occlusal views of both dental arches. The variables applied at the initial examination were recorded by the use of diagnostic terms and not by measurements. The photographs thus provided more precise information and were used to identify the specific malocclusion traits present at 8 years of age.
On the basis of the photographs, 420 individuals were selected, as they belonged to one of the following groups at the age of 8:
- •
Deep bite: (1) at least 1 lower incisor not visible because of total overlap by upper incisors or (2) contact between at least 1 lower incisor and the palatal mucosa apparent in the intraoral photograph (D group)
- •
Crossbite: anterior and/or posterior crossbite on 1 or more teeth (C group)
- •
Irregularity: pronounced irregularity of upper incisors (I group)
- •
Normal occlusion: no or only minor deviation in occlusion or alignment (N group, a reference group to the malocclusion groups)
After excluding those already deceased, emigrants, and persons living in remote areas, 183 individuals were invited for a follow-up examination and an interview. Sixty-nine persons (37.7%) accepted the invitation: D group = 20, C group = 21, I group = 10, N group = 18.
In 2007 these persons were examined and interviewed in their homes (n = 50) or in public dental clinics (n = 19) according to their own preference. The clinical examination included recording of number of teeth and prosthodontically restored or replaced teeth, oral function, and oral hygiene. In addition, intraoral photographs similar to those obtained in 1950, were taken, as well as extraoral photographs in frontal and profile views. The interviews followed a structured pattern and allowed for comments and follow-up questions and lasted from 0.5 to 1 hour. Issues addressed were attitudes and opinions about the subject’s own teeth in childhood and at present, experiences related to teeth and occlusal function, as well as attitudes toward teeth and dental appearance in general. The study was approved by the Ethical Committee for Medical Research (S-06208) and the Norwegian Social Science Data Services (14858).
Results
Occlusion
Of the 69 persons, 14 had received orthodontic treatment: 1, 8, 5, and 0 in the D, C, I, and N groups, respectively. For the 8 persons with crossbite, treatment had been provided with simple appliances in the early mixed dentition, which in 6 had resulted in correction of inverted incisors ( Fig 1 ).
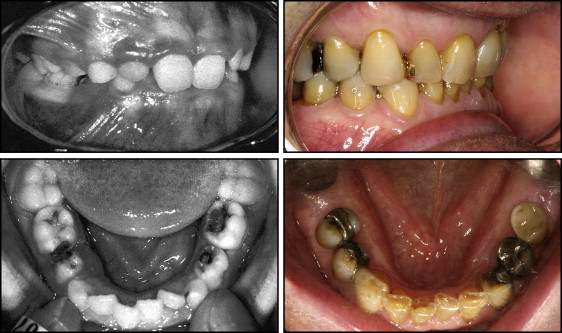
In the deep-bite group, changes in the anterior occlusion could not be assessed in 4 individuals because of comprehensive prosthodontic restorations. No change was observed in 2 persons, whereas 9 showed a decrease ( Fig 2 ) and 5 an increase in the deep bite. Deepening of the bite could be observed in combination with increased mandibular crowding ( Fig 3 ) but could also be seen with maxillary crowding ( Fig 4 ). Four persons complained about impingement of the palatal soft tissue.
Among individuals with posterior crossbite in childhood, the crossbite persisted and had in 4 persons developed into Class III malocclusions ( Fig 5 ). Changes in incisor irregularity (I group) could not be assessed in most individuals, as comprehensive restorative work probably camouflaged tooth displacement in 3 in addition to the 5 who had been orthodontically treated. In the group who initially had normal occlusion, no change ( Fig 6 ) or only small changes (increased anterior crowding) were observed in most of them. Only one person in this group had developed a significant malocclusion ( Fig 7 ).
Oral health and behavior
All but 3 persons reported that they visited their dentist once or twice annually. Table 1 shows the number of persons with excellent oral hygiene, the average number of missing and prosthodontically restored or replaced teeth, and the number of persons reporting TMJ problems in the various groups. Only small differences between the groups appeared for oral hygiene and restorations. On average, fewer teeth were missing in the N group, and relatively fewer persons in the N and D groups reported TMJ problems.



