8
How to implement lasers in dental hygiene
In this chapter, procedures that can be applied and implemented by the dental hygienist will be discussed. Again, it is the responsibility of the hygienist to ensure which laser applications can legally be performed within the state.
Most patients come in for a cleaning twice a year because their insurance covers it, and they believe they are doing a preventative procedure. However, if bleeding is present in patients’ mouths, then hygienists know that the patient is past the point of prevention. It is vitally important that patients are educated about the signs of gum disease and that the diagnoses made are more aggressive or that hygienists insist on recare. Hygienists can fall into the trap of allowing insurance companies to dictate the amount of care for patients. It is imperative that hygienists examine patients and create a treatment plan that suits their dental needs. In this chapter, laser bacterial reduction (LBR), laser-assisted periodontal therapy (LAPT; de-epilialization of the diseased tissue), herpetic lesion, aphthous ulcer (canker sore), and desensitization of the tooth structure will be discussed.
LASER BACTERIAL REDUCTION
This procedure is used for every patient that comes for a hygiene appointment in the office. Whether they have perfectly healthy gingiva, gingivitis, or periodontal disease, this procedure is beneficial to patients because of the added benefit it can provide.
Figure 8.1 Laser bacterial reduction introduction to the patient. This is used in the patient’s periodontal treatment folder. Courtesy of Jessica Blayden.

It is even recommended for pediatric patients starting at the age of 8; this is when mixed dentitia is present and when children are in orthodontia. Many times orthodontia produces inflammation, redness, poor oral hygiene, and moderate to severe bleeding resulting in gingivitis. This is the ideal use for LBR for these patients, in addition to usual hygiene service.
Each patient can benefit from this procedure because everyone has bacteria present. In addition, as described in Chapter 5, bleeding is the last stage of the pathogenesis of periodontal disease, and most, if not all, patients bleed.
LBR should be performed on every patient for these added benefits (Figure 8.1):
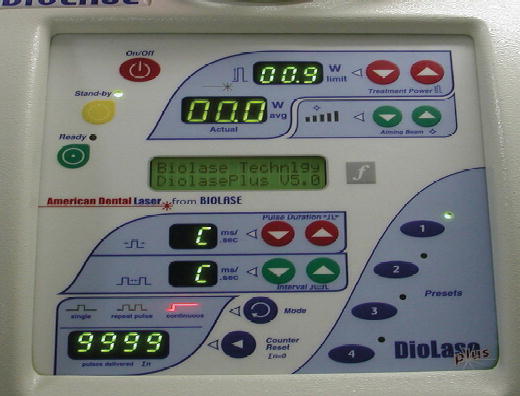
A typical setting for the LBR (Figure 8.2) is:
- Power 1.5 W
- Pulse duration 20 ms/s
- Interval 20 ms/s
- Uninitiated tip
- 10 to 15 seconds per tooth
The laser is used on 1.5 W pulsed (pulsed meaning it is on half the time and off half the time), creating a thermal relaxation period so the patient’s gingiva is more comfortable. This means 0.75 W is being emitted to the tissues and allowed to be absorbed. The laser is placed 0.5 mm into the sulcus and used with an uninitiated tip. An initiated tip is when articulating paper (e.g., Acufilm 2, Plastic is best) is melted on the end of the laser fiber to become pigmented to absorb/attract the diseased/infected tissue while leaving the healthy tissue alone. With an uninitiated tip, the laser fiber is bare (flashlight effect in the sulcus) and without pigment on the end of the fiber.
This procedure is used in an exploratory stroke with a light feather grasp, not a working stroke, taken around each tooth in the sulcus allowing the laser energy to be in a defocused mode because it is uninitiated like a flashlight effect in the pocket. Use the laser for 10 to 15 seconds per tooth, both buccal and lingual, while focusing the laser toward the tissue not the tooth.
There is the possibility that the laser may initiate itself during this procedure. The tell-tale signs are smoke, plume, patient response, and the laser fiber may start coagulating tissue. When diseased tissue is present, even with the laser being placed at 0.55 mm, the laser naturally initiates if bleeding occurs, inflammation is present, or sometimes plaque is present. If this happens, take the cleaving instrument provided by the laser manufacturer and cleave (score lightly) the laser fiber to become a bare freshly cleaved round circle so no spurring occurs and to ensure you are in the correct mode.
LBR lowers the gram-negative bacteria specifically from billions 109 down to hundreds 102 and lasts for 4 to 6 weeks (Moritz et al. 1998). Doing a LBR first on every patient that comes in for a cleaning eliminates bacteria, prevents cross contamination, and prevents periodontal pathogens before loss of attachment. Further, it reduces patient sickness after cleaning (as a result of free-flowing bacteria) and it helps prevent hygienists from being exposed to the same bacteria.
After LBR, the hygienist may consider polishing as another step in reducing bacterial plaque, which also cuts down on the time of scaling and allows the hygienist to focus on calculus.
The cost for this procedure is generally $25 to $40 for the full mouth and most insurance does not cover it. However, if dental hygienists were to implement LBR on every patient, it would increase revenue:
5 patients × $35 = $175 a day increase
× 4 days: $700 a week increase
× 4 weeks/1 month: $2800 a month increase
× 12 months: $33,600 a year increase.
Figure 8.2 Laser set at 1.5 W, pulsed, for laser bacterial reduction.

LASER-ASSISTED PERIODONTAL THERAPY
As a basic premise, the gold standard for successful treatment is defined as maintenance of, or gain in, the clinical attachment level, and initial therapy has a similar widely accepted benchmark in that treatment must include debridement of the accretions on the root surface by means of scaling. These are the settings for laser-assisted periodontal therapy (LAPT; Figure 8.3):
- Power 0.5–1.0 watts
- Continuous wave
- No pulse or interval
- Initiated tip
- 10 to 15 seconds per pocket but no more than 1 minute per tooth
- Nd:YAG 1064-nm settings are as follows: 30 mj, 50 Hz = 1.5 W, 40 s a site, adjust as needed.
To begin LAPT, go over the probe sheet and select a treatment plan. Always start with the deepest pockets because these areas will be retreated with the laser at subsequent appointments. If pockets are more than 7 mm in a particular area, the hygienist may only want to treat two to three teeth a session (not quadrants). Each session is determined by individualizing the treatment plan, and the hygienist dictates that by answering the following questions:
- How much bleeding is present?
- What are the systemic factors/environmental factors?
- How deep are the pockets?
- Is there mobility or suppuration present?
- How much calculus is present?
- How much plaque is present?
- How cooperative is the patient?
Figure 8.3 Laser settings for laser de-epithelization.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


