40 Oral ulceration
Summary
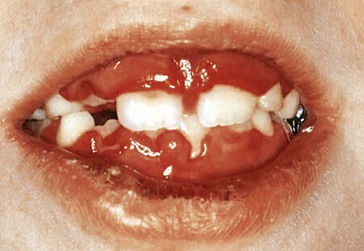
Alan is 8 years old. He has been brought to the surgery by his mother because his mouth is so painful he cannot eat (Fig. 40.1). What could cause this problem? How would you treat it?
History
Medical history
 Describe the appearance of the upper and lower gingivae in Figure 40.1.
Describe the appearance of the upper and lower gingivae in Figure 40.1.
There is erythematous gingival enlargement with small ulcerations of the gingival margin.
 What is the diagnosis?
What is the diagnosis?
Primary herpetic gingivostomatitis.
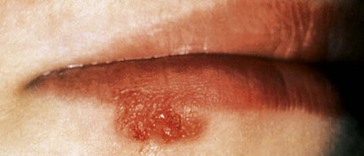
There are two types of herpes simplex virus: herpes simplex type 1 (HSV-1) and herpes simplex type 2 (HSV-2). Classically HSV-1 causes oral disease and HSV-2 causes genital disease. The viruses, however, are very similar and both can cause both oral and genital disease, although there are differences in recurrence rates. Primary exposure to HSV in the mouth causes acute primary herpetic gingivostomatitis (Fig. 40.1). The virus causes a viraemia, fever, malaise and lymphadenopathy. All the surfaces of the mouth including the hard palate and attached gingiva can be involved, initially with a vesicular rash that ulcerates and becomes superinfected. The illness lasts for 10–14 days before resolving spontaneously. Diagnosis is usually made on clinical grounds but can be confirmed by a threefold rise in the convalescent antibody titre over that seen in the acute phase or by direct immunofluorescence of vesicular fluid using specific antisera.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses