Chapter 4
The Contribution of Periodontics to Orthodontic Therapy
Periodontally Accelerated Osteogenic Orthodontics (PAOO)
The innovative combination of selective alveolar periodontal decortication surgery and augmentation grafting with orthodontic treatment results in an acceleration of orthodontic treatment, enhanced stability of orthodontic results, and long-term improvement of the periodontium (Wilcko 2003). The purposes of this section are to describe the Periodontally Accelerated Osteogenic Orthodontics technique and to explain how and why this advanced periodontal surgical technique contributes to orthodontic treatment.
Decortication or corticotomy means simply the intentional cutting or injury of cortical bone. While the bony jaws are composed of both cortical and medullary bone in various combinations depending on site and patient demographics, the periodontal surgery of interest in contemporary selective alveolar decortication involves only surgical injury of alveolar cortical bone.
The application of corticotomy surgery to correct malocclusion was first described in 1892 by L. C. Bryan, but it was Heinrich Köle in 1959 who reintroduced alveolar corticotomy to resolve malocclusion (Köle 1959). He combined interdental alveolar corticotomy surgery with a through-and-through osteotomy apical to the teeth. Generson et al. in 1978 offered a modification of the Köle protocol and eliminated the subapical osteotomy portion of the surgery.
In 2001, Wilcko et al. described selective alveolar decortication with augmentation grafting combined with orthodontic treatment. They patented and trademarked their technique as Periodontally Accelerated Osteogenic Orthodontics (PAOO). Full-thickness labial and lingual alveolar flaps were laid adjacent to the teeth intended for movement, and selective decortication surgery was performed. Given that the surgery was done only in the area of desired tooth movement, it was the thickness of cortical bone that dictated where and how the cortical bone was injured. The depth of the decortication cuts barely penetrated into medullary bone and bleeding was promoted; care was taken not to injure any tooth or encroach on the periodontal ligament. An allograft of resorbable grafting material plus antibiotic was applied directly over the bleeding bone, and the surgical site was closed using Gore-Tex suture material. A frequently used grafting mixture was equal portions of demineralized freeze-dried bone (DFDBA) and bovine bone (Osteograf/N-300 or Bio-Oss) wetted with clindamycin phosphate (Cleocin) solution.
Wilcko et al. observed rapid orthodontics following PAOO and active treatment times of 6 to 8 months were common. They questioned Köle’s precept of “bony block” movement and offered an alternative hypothesis that rapid tooth movement resulted from marked but transient decalcificationrecalcification of the alveolus. Frost, an orthopedic surgeon, had described a direct correlation between degree and proximity of bone trauma and intensity of physiological healing response, which he coined Regional Acceleratory Phenomena, or RAP (Frost 1983), and the decalcification-recalcification described by Wilcko et al. (2001, 2003) was consistent with RAP.
- Increased alveolar volume and enhanced periodontium (i.e., correction of dehiscences and fenestrations)
- Accelerated treatment (i.e., 3 to 4 times more rapid active orthodontic treatment)
- Greater stability of clinical outcomes and less relapse
- Enhanced scope of malocclusion treatment (i.e., avoiding orthognathic surgery and extractions in selected cases)
- Enhancement of patient’s profile when indicated
- Rapid recovery of impacted teeth (i.e., canines)
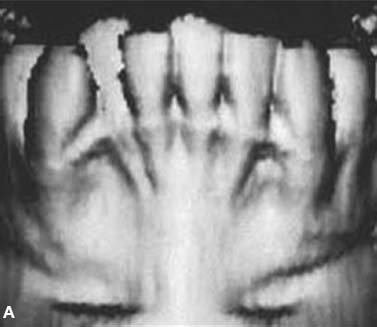
The initial decortication protocol used by the Wilcko brothers did not include augmentation alveolar grafting. Computed Tomography (CT) scans were taken on the first series of patients to compare pretreatment status with immediate post orthodontics and at least 1-year retention conditions. The CT scans of the alveolus immediately after braces were removed showed a paucity of alveolar bone in the areas where decortication surgery was performed. However, the retention images demonstrated that a minimally adequate amount of mineralized alveolar bone would return if the soft tissue periodontal envelope remained intact (Fig. 4.1).
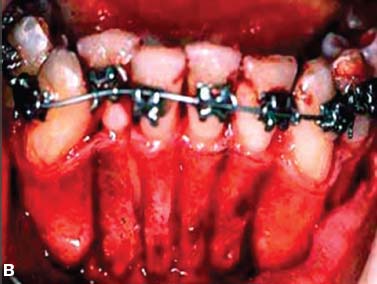
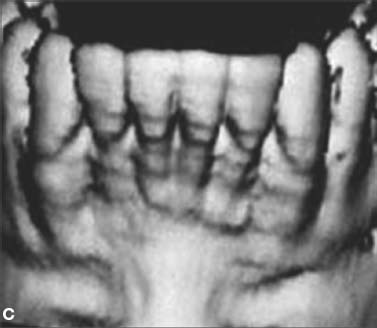
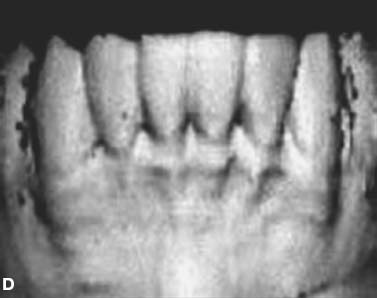
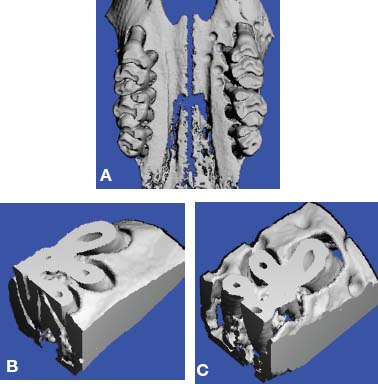
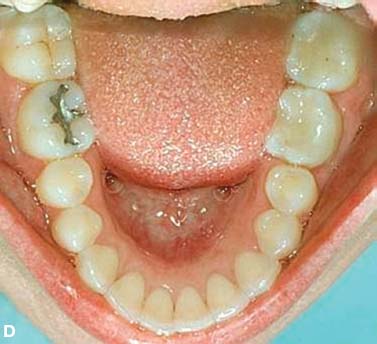
Fig. 4.1. CT and surgery images of patient treated with selective alveolar decortication without augmentation grafting demonstrating lack of calcified cortical plate at post orthodontic treatment but return of cortical plate volume by 1 year retention. A: CT image at pre-treatment showing root prominences; B: view of labial cortical bone at the time of selective alveolar decortication surgery; C: CT image at immediate post orthodontic treatment showing lack of calcified labial cortex; D: CT Image at 1 year after active orthodontic treatment showing adequate but minimal calcified labial cortex.
Since 1996, the PAOO technique has included augmentation grafting to increase alveolar volume (Fig. 4.2). Results of research showed no change in alveolar cortical bone thickness at an average of 1.5 years following immediate post orthodontic treatment (Twaddle 2002). A recent study of attached gingival levels in PAOO patients resulted in significantly more attached gingiva evident at least 1 year after active orthodontic treatment. Increases in attached gingiva were consistent in the lower dental arch and inconsistent in the maxillary arch (Kacewicz 2007).
Fig. 4.2. CT and surgery images of patient treated with selective alveolar decortication and augmentation grafting demonstrating ample cortices post grafting. A: CT image at pre-treatment showing root prominences; A-1: view of labial cortical bone at the time of selective alveolar decortication surgery; A-2: view of surgery area after grafting; B & C: CT images at post orthodontic treatment (B) and 2.5 years retention (C) showing increased volume of labial cortical bone.
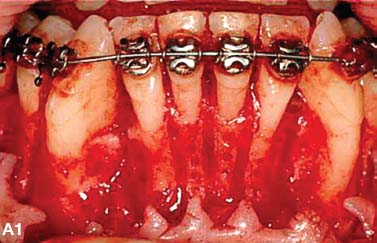
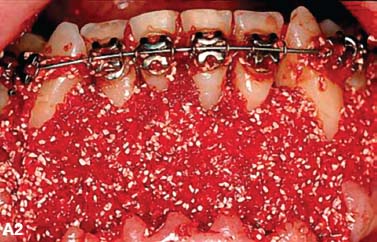
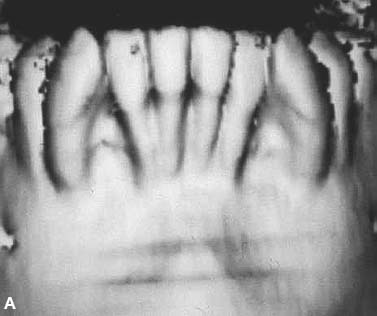
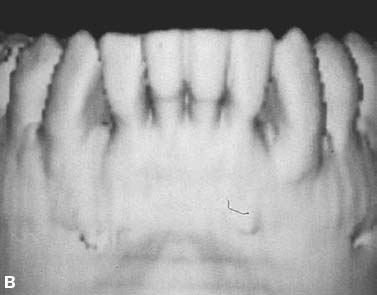
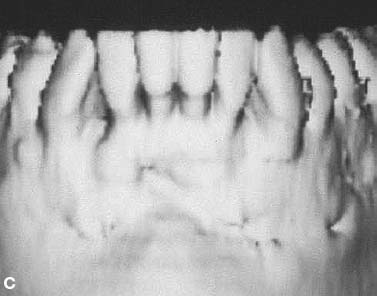
An additional benefit of augmentation bone grafting is the repair of alveolar cortical bone fenestrations and dehiscences (Fig. 4.3). The grafting procedure is done without membranes because full-thickness flaps are used followed by primary closure in a healthy periodontium. Under these circumstances, migration of the epithelial attachment is not likely to occur, and the intact periosteum serves as a natural “membrane.”
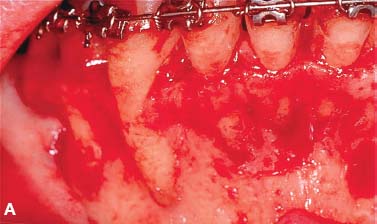
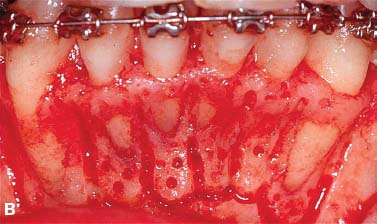
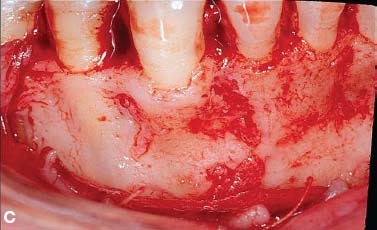
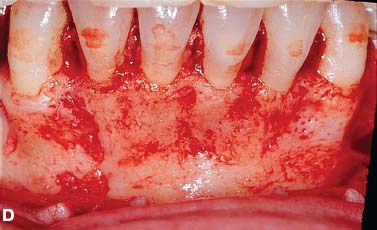
Fig. 4.3. Augmentation alveolar grafting repairs bony dehiscences and fenestrations. A: evidence of bony discrepancies after full thickness flap, B: decortication prior to grafting with dehiscences and fenestrations outlined; C-D: absence of dehiscences and fenestrations 7.5 years post PAOO decortication and grafting.
PAOO has contributed greater stability of orthodontic clinical outcomes and less relapse. Stability of orthodontic clinical outcomes was analyzed by Nazarov in 2003 using the Objective Grading System (OGS) sanctioned by the American Board of Orthodontics (ABO). While no differences were observed in nonextraction therapies at immediate post treatment between PAOO and non-PAOO groups, three of the nine OGS variables (alignment, marginal ridges, and total score) were significantly better in the PAOO group at retention. O’Hara (2005) compared nonextraction orthodontic treatment of moderate malocclusions and found no differences in the OGS alignment variables at post treatment. But at retention, alignment had improved in the PAOO group, whereas in the two non-PAOO groups, fixed and removable appliance retention, alignment had relapsed. In summary, immediate post orthodontic treatment results following nonextraction therapy are statistically the same with or without PAOO. However, during retention, the clinical outcomes of PAOO patients improved and did not demonstrate relapse.
PAOO increases the scope of orthodontic tooth movement and the positions of the teeth after decortication and augmentation grafting are stable long-term. Sarver and Proffit (2005) offered guidelines as to the limits of central incisor tooth movement in the adult patient with orthodontic treatment alone. Ferguson et al. (2006) suggested that these limits can be expanded 2-fold to 3-fold in all dimensions except retraction following PAOO (see Fig. 4.4) and that the stability of these positions is probably due to loss of tissue memory from high turnover of the periodontium as well as increased thickness of the alveolar cortices from the augmentation grafting. Rothe et al. (2006) found that patients with thinner mandibular cortices were at increased risk for having dental relapse—hence the necessity for osseous grafting during the PAOO procedure.
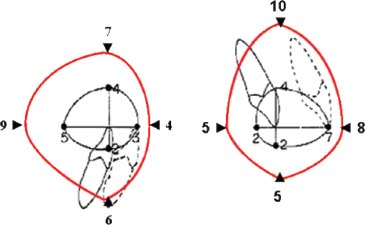
Fig. 4.4. PAOO enables a greater amount of tooth movement into stable positions. Limits of adult orthodontic tooth movement (in millimeters) into stable positions using orthodontics only is represented by the inner black-color envelope (after Proffit); limits of tooth movement for orthodontics combined with PAOO is represented by the outer red-color envelope. For example, protraction of the lower incisor into a stable position is 9mm if tooth movement is combined with PAOO compared to a 5mm limit without PAOO. Note that limits are about 2 to 3 times greater for central incisor protraction, extrusion and intrusion but not for incisor retraction. (Reprinted with permission from Bell 2006)
Periodontics, through PAOO therapy, contributes to orthodontic treatment by reducing active orthodontic treatment time. Claims of rapid orthodontic treatment times were first validated in research by Hajji in 2000; average active ortho-dontic treatment times were 6.1 months for nonextraction PAOO and 18.7 and 26.6 for nonextraction and extraction therapies without PAOO, respectively. In 2001, Fulk compared mandibular arch decrowding in nonextraction orthodontics following PAOO and non-PAOO; active treatment times were 3.1 times more rapid (6.6 versus 20.7 months) following PAOO and post treatment outcomes were statistically the same as judged by cephalometric and study cast variables. Similar results were reported in 2003 by Skountrianos for maxillary arch decrowding, wherein active orthodontic treatment time was 3.0 times more rapid when combined with PAOO than when not combined (7.0 versus 21.2 months).
In summary, the contributions of periodontal therapy to orthodontic treatment vis-à-vis PAOO is to increase alveolar volume and enhance the periodontium, enhance the stability of orthodontic clinical outcomes (less relapse), increase the scope of malocclusion treatable without orthognathic surgery, and reduce active orthodontic treatment time over 3-fold. These benefits are realized for two reasons: (1) tissues lose memory due to high hard and soft tissue turnover induced by the periodontal decortication, and (2) augmentation bone grafting increases alveolar volume and thickness of the alveolar cortices.
The clinical technique involving selective alveolar decortication is a form of periodontal tissue engineering resulting in a transient osteopenia and high turnover adjacent to the injury site. Alveolar decortication initiates a healing response, the degree of which is directly related to the intensity and proximity of the surgical insult. In healthy tissues, bony healing is synonymous with high osseous turnover, calcium depletion from the hydroxyappatite crystal lattice, and diminished bone density but not bone matrix volume (Frost 1983). Bogoch et al. (1993) made a penetrating surgical incision into the head of the tibia in rabbits and studied the healing response adjacent to the surgical wound. They found a 5-fold increase in medullary bone turnover adjacent to the corticotomy site. Buchanan et al. (1988) documented a similar observation in alveolar bone following tooth extraction, as did Yaffe et al. (1994) after alveolar periosteal flap elevation and Verna et al. (2000) after tooth movement.
Sebaoun (2005) studied the effect of decortication without tooth movement on alveolar turnover in the rat in a split mouth design using multiple approaches. Maxillary buccal and lingual full-thickness periosteal flaps were elevated adjacent to the upper left first molar, and decortication was performed with five palatal and five buccal bur marks (0.2 mm) under sterile irrigation. The following was observed adjacent to the decortication site at 3 weeks after surgery: (1) a 2-fold increase in decalcified trabecular bone (histomorphometric analysis using hematoxylin and eosin staining; see Fig. 4.5),(2) a 1.5-fold increase in new trabecular bone formation (vital staining ad libitum), (3) a 4-fold increase is osteoclast count (osteoclast count after TRAP staining), and (4) a 2-fold increase in lamina dura apposition (vital stain injection series; see Fig. 4.6). These findings collectively indicate high tissue turnover immediately adjacent to the decortication site.
Fig. 4.5. Cross section of the dentoalveolus of the rat showing 4 of the 5 upper first molar roots at 3 weeks control (A), 3 weeks decortication (B), and 11 weeks decortication (C). Testing of histomorphometric data resulted in significantly less calcified trabecular bone volume at 3 weeks on the decortication side except for 7 weeks decortication (not shown).
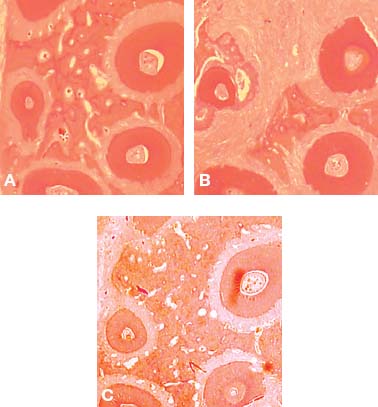
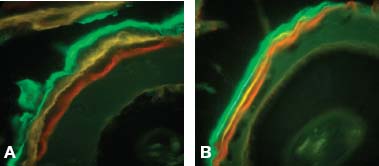
Fig. 4.6. Amount of apposition of the lamina dura is shown in cross section of the dentoalveolus of the rat at 4 weeks, the end of the first series of vital stain injections. Total width of apposition as revealed by the three stains together was statistically greater on the decortication side (A, 0.051mm) at 3 weeks than the control side (B, 0.037mm) at 3 weeks.
Pham-Nguyen (2006) studied the three-dimensional volume of periodontal tissues surrounding the upper first molar in the rat model following buccal and lingual selective decortication. Using micro-CT technology, a significant decrease in alveolar mineralization was evident by 7 days post decortication (Fig. 4.7).
Fig. 4.7. Micro-CT analysis of osteopenia at 7 days following selective alveolar decortication showing gross specimen #602 (A), control side (B) and decortication side (C).On the decortication side, osteopenia was demonstrated as the bone volume (BV) to total volume (TV) ratio decreased to 45% (note the wide spaces surrounding the roots, C) compared to 57% on the control side (B). (Pham-Nguyen K, et al. 2006)
Conceptually, increased tissue turnover (osteopenia) is a condition that favors rapid tooth movement. This tenet was demonstrated by Verna et al. (2000) using a rat model by moving teeth after pharmacologically inducing high and low bone turnover. They showed significantly greater tooth movement in the high turnover group compared with normal and low bone turnover groups. In our laboratory rat studies (Pham-Nguyen 2006, Sebaoun 2005), surgical injury to the alveolus induced a dramatic increase in tissue turnover that was expressed both spatially and temporally. The effect of alveolar decortication was localized to the area immediately adjacent to the injury. It is obvious that considerable medullary bone demineralization occurs immediately adjacent to the decortication site. Although induced osteopenia is a transient condition in the functionally normal alveolus, it was surmised that tooth movement perpetuates the decalicified condition of the trabecular bone (Fig. 4.8).
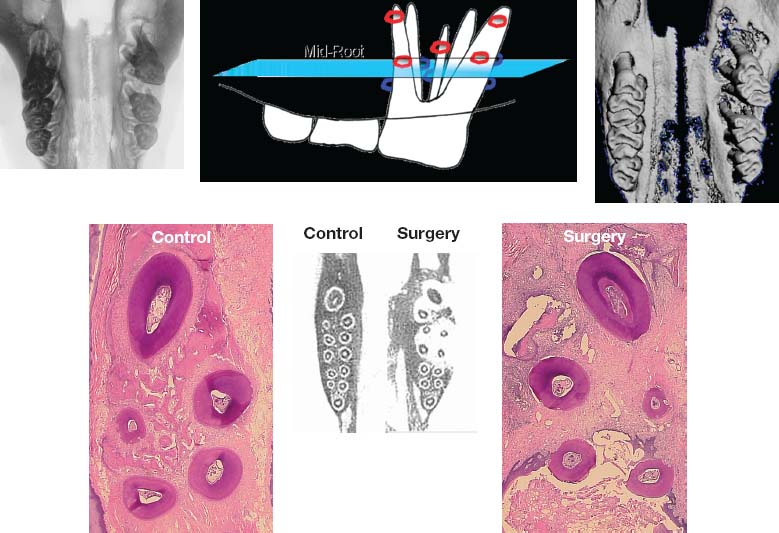
Fig. 4.8. Demonstration of trabecular bone osteopenia following decortication and 6 weeks of tooth movement in the rat. Clockwise from upper left image: faxitron cephalogram of animal > maxilla showing direction of 1st molar tooth movement; upper center: diagram indicating buccal (red) and lingual (blue) corticotomy cuts and histological cut through roots at mid-root level; upper right: gross 3D image of maxilla showing movement of 1st molar; lower right: H&E stain on surgery side showing lack of calcified trabecular bone surrounding the roots of the 1st molar; lower center: CT slice at mid-root level through 1st, 2nd and 3rd molars showing evidence of osteopenia (white) on surgery side compared to control side with rectangles representative of area covered in H&E stained images; lower left: H&E stain on control side showing ample calcified trabecular bone surrounding the roots of the 1st molar.
PERIODONTALLY ACCELERATED OSTEOGENIC ORTHODONTICS IN THE TREATMENT OF CROWDING
Using the PAOO technique, cases of moderate dental arch crowding are routinely completed in 4 to 6 months instead of 18 to 24 months of active orthodontic treatment, and the results have been shown to be remarkably stable (Figs. 4.9 and 4.10).
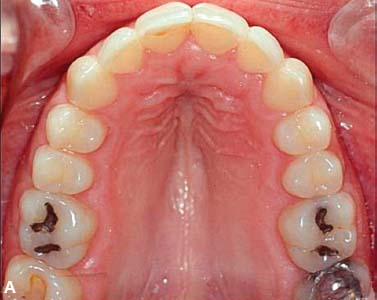
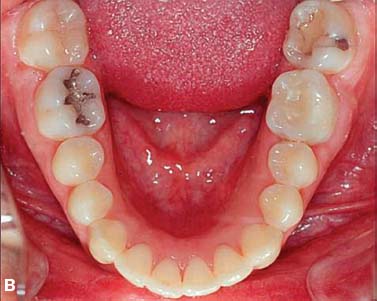
Fig. 4.9. Adult female patient with moderate upper and lower dental arch malocclusion (A,B) treated by PAOO (A-1, A-2, B-1, B-2) showing immediate post treatment outcome after 7 months of active orthodontic therapy (C,D).
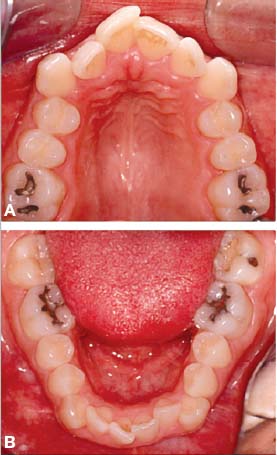
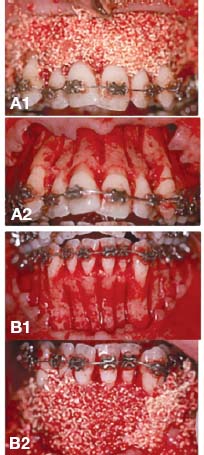
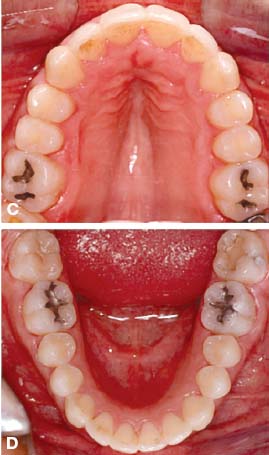
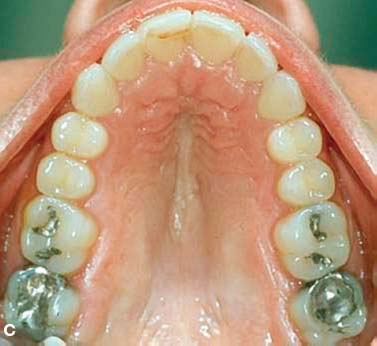
Fig. 4.10. Retention outcome at 2 years (A,B) and 9 years (C,D) after the completion of PAOO treatment. Improvement during retention and long term stability are likely due to high tissue turnover induced by decortication and increase in cortical bone thickness.
RAPID RECOVERY OF IMPACTED TEETH
Recovery of impacted teeth typically prolongs active orthodontic treatment time. Impacted tooth recovery combined with selective alveolar periodontal decortication surgery accelerates the recovery and reduces orthodontic treatment time. The purpose of this section is to describe an advanced periodontal surgical technique of recovering impacted cuspids that features the following: (1) complete exposure of the clinical crown, (2) clearing a path for recovery by way of alveolar ostectomy, and (3) selective alveolar decortication or intramarrow penetrations surrounding the impacted tooth root.
With the exception of the third molars, the maxillary canines are the most frequently encountered impaction, with an incidence of approximately 2% according to Ericson and Kurol (1987). The incidence of maxillary canine impaction is 3 times greater in females than in males and is often associated with missing or peg-shaped laterals (Bec et al. 1981, Peck et al. 1994). Maxillary permanent canines are impacted palatally much more frequently than labially (85% palatal compared with 15% labial; Bass 1967, Hitchin 1956, Jacoby 1979). Rayne (1969) has pointed out that labially impacted canines are often associated with inadequate arch space. Interceptive treatment of impacted maxillary canines can often be successful in 10- to 13-year-olds depending on the degree of the impaction (Jacobs 1992). The more severely impacted maxillary canines typically require combined surgical/orthodontic treatment (Bishara 1992).
Previous authors have indicated that details of the recovery technique depend on the type of impaction. When the crown is not covered by bone and there is a broad band of keratinized gingival tissue present, Kokich and Mathews (1993), Shiloah and Kopczyk (1978), and Jarjoura et al. (2002) have suggested a surgical window (gingivectomy) to expose the shallow impaction. In situations where there is only a narrow zone of gingival attachment and a relatively shallow labial or mid-alveolar bony impaction, an open technique consisting of an apically repositioned flap is more suitable according to Wong-Lee and Wong (1985) and Vanarsdall and Corn (1977). When the bony impaction is deep in the vestibule, mid-alveolar, or impacted palatally, Vermette et al. (1965), McDonald and Yap (1986), and Smukler et al. (1987) have suggested erupting the canine through the gingiva following primary surgical flap closure.
RECOVERY OF LABIALLY IMPACTED CANINES
Recovery of labially impacted maxillary canines is illustrated in the treatment of a girl aged 14 years 4 months using selec-tive decortication technique (Figs. 4.11, 4.12, and 4.13). A full-thickness labial flap, using a sulcular incision with vertical releasing incisions mesial to the first premolars, was reflected to reveal upper cuspid crowns labial to the upper permanent lateral incisors. No lingual flap was reflected. The upper primary canines were extracted, and the soft tissue follicle and thin layer of bone surrounding cuspid crowns were removed. A path (trough) was cleared for the forced eruptions by removing the facial cortical plate between the cuspid crowns and extraction sockets including the facial plates over the sockets. In addition, numerous intramarrow penetrations were made to stimulate alveolar bone turnover and to induce RAP or osteopenia. At least 1.5 mm of bone was left undisturbed mesial to the first premolars and distal to lateral incisors. An orthodontic bracket was placed in an optimal position of the upper right permanent canine, but the upper left permanent canine was rotated, which necessitated placing the bracket on the lingual surface. On the right side, the bracket was exposed with a vertical incision in line with the bracket, and then suturing the flap back into the original position. The upper left canine was covered by the flap and sutured back in its original position. Because the upper left canine was covered by the flap, a backup ligature wire was also used. In this case, a resorbable Vicryl suture was used.
Fig. 4.11. Labially impacted maxillary canines showing pre-surgery (
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


