37 White lesions: Candidosis (candidiasis)
Figure 37.1 Causes of white lesions.
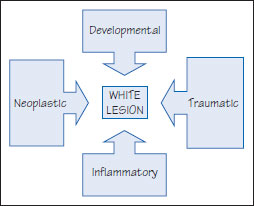
Figure 37.2 White patch diagnosis.
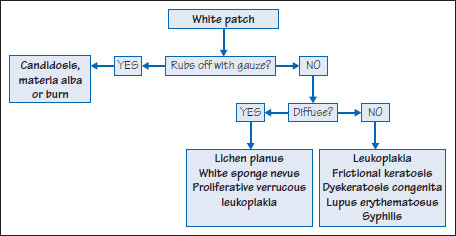
Figure 37.3 Factors predisposing to candidosis.
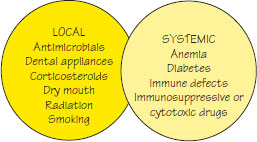
Figure 37.4 Pseudomembranous candidosis.
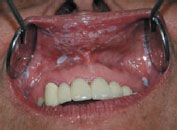
Figure 37.5 Candidosis.
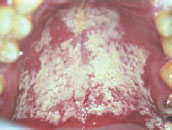
Figure 37.6a Candidosis in HIV/AIDS before wiping with gauze.
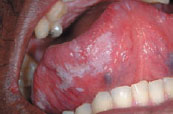
Figure 37.6b Candidosis after wiping with gauze.
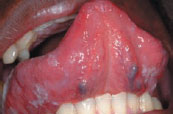
Table 37.1 Causes of oral white lesions.
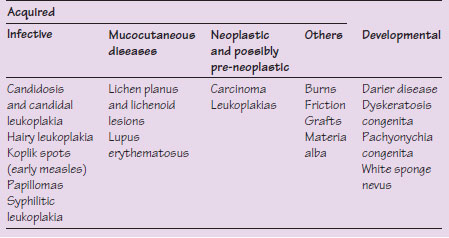
White patches may be produced by epithelial debris (e.g. “material alba” – white debris which accumulates where oral hygiene is lacking), sloughing (e.g. burns), or epithelial thickening – rarely inherited but more commonly acquired (Figure 37.1) (Table 37.1). Superficial conditions such as debris or candidosis can be wiped away with a dry gauze (Figure 37.2).
Acute pseudomembranous candidosis
(Also called “thrush” in UK and some other countries.)
Definition: Lesions consist of white flecks, plaques or nodules, which will wipe off with gauze.
Prevalence (approximate): Uncommon.
Age mainly affected: Neonates and adults.
Gender mainly affected: M = F.
Etiopathogenesis: Candida albicans is a harmless commensal yeast in the mouths of nearly 50% of the population (carriers). Oropharyngeal candidosis may be seen in healthy neonates as they have yet to acquire immunity. Local ecological changes such as a disturbance in the oral flora (e.g. by antibiotics, xerostomia), or a decrease in immune defences (e.g. by immunosuppressive treatment or immune defects (HIV/AIDS, leukemias, lymphomas, cancer, diabetes)), can allow Candida to become an opportunistic pathogen (Figure 37.3). There is also an increase in/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


