3 Pre-operative Analysis and Prosthetic Treatment Planning in Esthetic Implant Dentistry
W.C. Martin, D. Morton, D. Buser
The goal of risk assessment is to identify patients whose implant therapy carries a high risk of a negative outcome. Therefore, for each patient, a detailed preoperative analysis should be performed to assess the individual risk profile and the level of difficulty of the planned therapy.
Consensus Statement B.1
Planning and Execution:
Implant therapy in the anterior maxilla is considered an advanced or complex procedure and requires comprehensive preoperative planning and precise surgical execution based on a restoration-driven approach.
Consensus Statement B.2
Patient Selection:
Appropriate patient selection is essential in achieving esthetic treatment outcomes. Treatment of high-risk patients identified through site analysis and a general risk assessment (medical status, periodontal susceptibility, smoking, and other risks) should be undertaken with caution, since esthetic results are less consistent.
The initial examination of the patient requiring dental implants in the anterior maxilla should commence with a general treatment risk assessment. Risk assessment in the anterior maxilla of potential implant patients includes several aspects. The patient’s past medical history, current medications, allergies, smoking habits, periodontal status and occlusal function should be examined (Buser and coworkers, 2004). Table 1 lists the superordinate, general risk factors in implant patients:
With regard to implant success, high-risk patients should be informed of the challenges associated with the treatment. Alternative restorative methods should be duly considered before planning for dental implant therapy. Patients who qualify for surgical implant procedures from a medical point of view and whose esthetic demands are high should always undergo a detailed examination not only of the edentulous space, but also of the supporting hard and soft tissues. Adjacent teeth, periodontal support, and existing hard and soft tissues are all critical factors when planning for a predictable esthetic result. Together, these factors constitute an assessment of esthetic risk.
In simple terms, the esthetic quality of implant-supported restorations should not differ from that of restorations supported by teeth. They should be in harmony with perioral facial structures, be associated with a healthy surrounding dentition and represent a successful imitation of the missing tooth or teeth with regard to color, form, texture, size, and optical properties (Belser and coworkers, 2004). Achieving such an outcome presupposes a clear understanding of dental esthetics and general esthetic principles, and depends on the treatment team developing an acute diagnostic acumen.
Consensus Statement C.1
Standards for an Esthetic Fixed Implant Restoration:
An esthetic implant prosthesis was defined as one that is in harmony with the peri-oral facial structures of the patient. The esthetic peri-implant tissues, including health, height, volume, color, and contours, must be in harmony with the healthy surrounding dentition. The restoration should imitate the natural appearance of the missing dental unit(s) in color, form, texture, size, and optical properties.
| General Risk Factors in Candidates for Implant Therapy | |
| Risk Factor | Remarks |
| Medical |
|
| Periodontal |
|
| Oral Hygiene/Compliance |
|
| Occlusion |
|
3.1 Diagnostic Factors for Esthetic Risk Assessment
Diagnostic factors of significance to the pre-treatment examination of the esthetic risk to the treatment outcome include:
-
Patient’s treatment expectations
-
Patient’s smoking habits
-
Height of the lip line on smiling
-
Gingival biotype in the treatment area
-
Shape of the missing and surrounding teeth
-
Infection at the implant site and bone level at adjacent teeth
-
Restorative status of the teeth adjacent to the edentulous space
-
Character of the edentulous space
-
Width of the hard and soft tissues in the edentulous space
-
Height of the hard and soft tissues in the edentulous space
These criteria can be used to create an Esthetic Risk Profile that will help the clinician and patient determine the potential of achieving esthetic results through dental implant therapy.
3.1.1 The Patient’s Treatment Expectations
The recent rise in public awareness of the benefits of dental implant therapy has had both positive and negative effects on daily clinical practice. We benefit from the increasing numbers of patients who desire dental implant treatment, but most patients are unaware of what the process entails. Access to the Internet has helped educate patients on how dental implants are used to replace missing teeth. Unfortunately this education may lead to unrealistic expectations that the treatment team cannot attain. During the consultation visit, it is imperative to determine the patient’s ultimate desires. Discussion of the oral rehabilitation project should focus on three aspects: form, function, and esthetics (Garber and coworkers, 1995; Morton and coworkers, 2004). Reviewing these areas with the patient may help generate an initial risk profile for the esthetic outcome and patient acceptance.
Form
Can the edentulous span be restored at all? An evaluation of the restorative space in relationship to adjacent or contralateral teeth will determine if orthodontic or restorative procedures are necessary before or along with implant therapy (Figs 1a, b). Visualizing the planned restoration will also provide information on the available hard and soft-tissue support, whether deficient, adequate, or excessive. Accepted dental procedures, including diagnostic wax-ups and photographs, are important to this visualization.
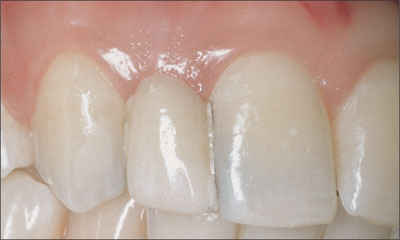
Fig 1a Pre-treatment examination. Too little restorative space for a dental implant at site 12.
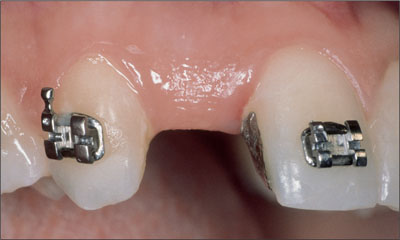
Fig 1b Post-orthodontic treatment. Ideal space for a dental implant and restoration.
Function
An occlusal evaluation is necessary to incorporate the implant-supported restoration into a harmonious and functional environment. In the case of long-standing edentulism, supereruption of the opposing dentition into the free space may make restoration of the implant(s) difficult (Fig 2).
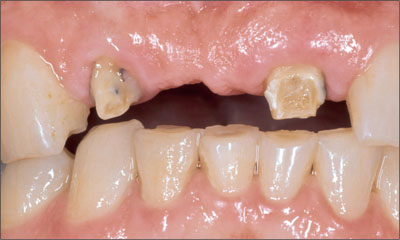
Fig 2 Pre-treatment examination. A lack of available interocclusal space for restoration using dental implants. Treatment of the opposing dentition may be required to achieve long-term implant success.
Diagnostic wax-ups help establish a plan for modifying the positions of those teeth and will often be a mandatory component of pre-treatment esthetic analysis.
Esthetics
What are the patient’s esthetic expectations? And are they realistic? A detailed discussion with the patient concerning the potential outcome may help avoid disappointing outcomes for patients with high esthetic expectations. Such patients should be considered “high esthetic risks.”
Consensus Statement C.2
Definition of the Esthetic Zone:
Objectively the esthetic zone was defined as any dentoalveolar segment that is visible upon full smile. Subjectively the esthetic zone can be defined as any dentoalveolar area of esthetic importance to the patient.
3.1.2 Patient’s Smoking Habits
When determining the potential for the esthetic success of a given course of implant treatment, potential complications secondary to the local and general factors should also be considered. Smoking habits may have deleterious effects on grafting procedures, implant integration, or long-term peri-implant tissue health (Buser and coworkers, 2004). Several clinical studies have shown smoking to have a negative impact on the short-term and long-term integration of dental implants (Bain and Moy, 1993; De-Bruyn and Collaert, 1994; Lambert and coworkers, 2000; Wallace, 2000). Patients who smoke should be educated on or directed to cessation programs before implant therapy is initiated. Heavy smokers (>10 cig/d) should be considered “high esthetic risks.”
3.1.3 Height of the Lip Line on Smiling
The lip line is associated with the amount of tooth substance and supporting tissues visible when the patient chews, speaks, or smiles.
Low Lip Line
Patients who exhibit a low lip line display a predominance of mandibular teeth or an equal mix of maxillary and mandibular teeth. For these patients, the quality of the esthetic outcome is related mostly to the appearance of the incisal half of the maxillary teeth (Fig 3).
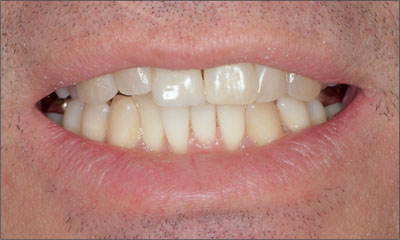
Fig 3 Low lip line.
Here the “esthetic risk” is reduced as the lips effectively mask sub optimal outcomes associated with the appearance of the gingival tissues, tooth proportions, and the apical aspects of the restoration.
Medium Lip Line
Patients who exhibit a medium lip line typically display most of their anterior maxillary teeth and only very little, if any, of the supporting periodontal structures (Fig 4). Here the esthetic risk is increased and is associated with factors affecting the appearance of these teeth and restorations, such as tooth size, color, shape, texture, optical properties, relative proportions, as well as the shape and appearance of the incisal and gingival embrasures and the presence of convexity in the teeth and the surrounding structures.
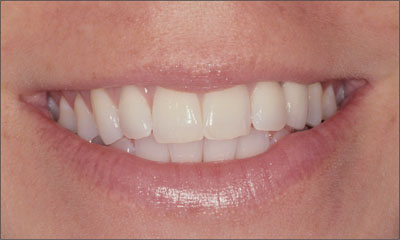
Fig 4 Medium lip line.
High Lip Line
Patients characterized by a high lip line often display their maxillary anterior teeth in their entirety, as well as a significant portion of the supporting soft tissues (Fig 5). The esthetic risk for these patients is greatly increased, mostly associated with the gingival tissue display. It can be difficult to develop healthy, symmetric, and contoured soft tissues, and any failures will be readily visible—particularly when restoring adjacent missing teeth (Buser and coworkers, 2004). Moreover, the display of gingival structures increases the relevance of tooth proportions and their emergence profile. The esthetic contours of the gingival margins are also critical to the outcome in patients with high esthetic demands.
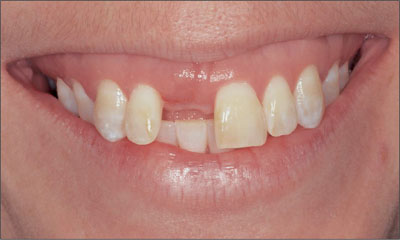
Fig 5 High lip line.
3.1.4 Gingival Biotype in the Treatment Area
Thick-Gingiva Biotype
A thick-gingiva biotype can be low-risk when replacing single missing teeth in the anterior area. The gingival tissues in these patients are characterized by a predominance of a thick, broad band of attached gingiva, typically resistant to recession (Cardaropoli and coworkers, 2004; Kan and coworkers, 2003; Kois and coworkers, 2001; Weisgold, 1977) (Fig 6).
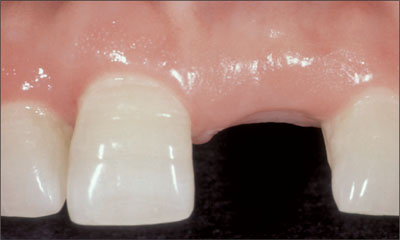
Fig 6 Thick-gingiva biotype characterized by a broad band of thick keratinized tissue and blunted papillae.
The thickness of the gingival tissue effectively masks the color of the implant(s) and any subgingival metallic components, reducing the risk of not achieving a pleasing esthetic result. This biotype clearly favors the long-term stability of esthetic peri-implant soft tissues. Special surgical consideration should be given to thick-gingiva biotype patients, as they are more prone to post-surgical scarring subsequent to augmentation procedures.
For patients with multiple adjacent missing anterior teeth, a thick-tissue biotype can be both favorable and detrimental. Thick gingiva remains predictable in terms of position and appearance and resistant to recession. However, the character of the tissue reduces the likelihood of papillae developing when multi-tooth edentulous areas are present (Fig 7).
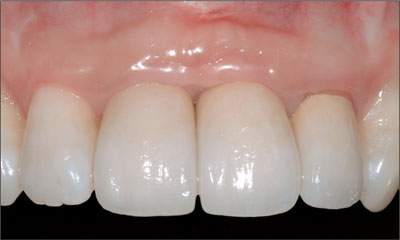
Fig 7 Restoration of adjacent spaces 11 and 21 with crowns supported by dental implants in a patient with a thick-gingiva biotype.
Medium-Gingiva Biotype
For patients with a medium-gingiva biotype, esthetic restoration of missing teeth is more challenging in the long term, and the esthetic risk is increased. Medium-gingiva biotypes display some characteristics of a thick biotype—most often the presence of thick attached gingival tissues. In addition, however, they can display characteristics of a thin-gingiva biotype, including long, thin, and blunted dental papillae (Fig 8).
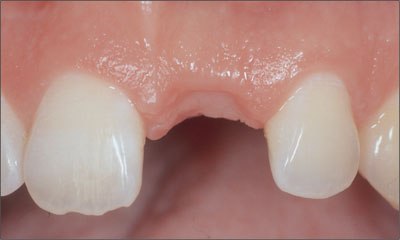
Fig 8 Medium-gingiva biotype characterized by a broad band of thin keratinized tissue with blunted papillae.
In these cases, esthetic restorations ar/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


