A new classification system for periodontal diseases was published in Annals of Periodontology in 1999. It was approved by the American Academy of Periodontology and was elaborated in accordance with the principles of evidence-based medicine.
This classification was intended to integrate epidemiologic, etiologic, and pathogenic data, and aimed at creating a rational classification system based on sound evidence rather than on clinical impressions. Only chronic and aggressive forms of periodontitis will be discussed in this book.
Gingivitis
Dental-plaque-induced gingival diseases
• Gingivitis associated with dental plaque only:
– without other local contributing factors
– with local contributing factors
• Gingival diseases modified by systemic factors
• Gingival diseases modified by medications
• Gingival diseases modified by malnutrition
Non-plaque-induced gingival lesions
Chronic periodontitis
Localized
Generalized
Aggressive periodontitis (Formerly juvenile, or precocious, or rapidly progressing periodontitis)
Localized
Generalized
Periodontitis as a manifestation of systemic diseases
Associated with hematological disorders (eg, leukemias)
Associated with genetic disorders (eg, Down syndrome, Papillon-Lefèvre syndrome)
Necrotizing periodontal diseases (eg, HIV infection)
Abscesses of the periodontium
Periodontitis associated with endodontic lesions
Developmental or acquired deformities and conditions
Localized and generalized forms of chronic periodontitis, while still referred to as adult periodontitis, are also observed in adolescents. However, there is little reason to associate these disease subtypes with a specific age category. Hence, a nonspecific terminology was preferred, and chronic periodontitis was deemed better-suited to describe the slow progression of the disease, though some patients may exhibit short periods of accelerated progression (Armitage 1999) .
Clinical Signs and Symptoms of Periodontal Disease
An adequate evaluation of the clinical signs of periodontal disease is crucial not only for disease detection but also for recognition of disease type and severity. The collection of data leads to a diagnosis, orients treatment strategies, and allows for a prognosis to be made. This evaluation involves finding evidence of:
• Signs of inflammation
• Tissue damage
The usual parameters of destruction—attachment loss, pocket depth, bone loss, tooth mobility, and dental migrations—represent the historic aspects of disease progression. They help in appreciating severity but do not necessarily reflect the degree of pathologic activity. Pathologic activity is characterized by objective signs, such as the intensity of inflammation and presence of suppuration, and subjective signs, such as discomfort, tenderness, pain, and halitosis. However, the most significant sign is bleeding on probing. Again, periodontitis is known to progress discontinuously, and most of these clinical signs are present whether the disease is in an active or inactive phase. Taken together, these considerations emphasize the importance of developing better diagnostic and prognostic tests (Griffiths et al 1988). Microbiologic analysis seems a particularly powerful tool for proper evaluation of periodontal disease. This is discussed in the next chapter.
The readings recorded during periodontal probing are inaccurate if they are evaluated on inflamed tissue, because the probe can penetrate the inflamed connective tissue of the periodontal ligament. Correct scores are obtained only after reduction of inflammation.
The main treatment objective is to arrest periodontal destruction by eradicating inflammatory processes. Tissue repair, including attachment gain, reduction of pocket depth, mobility reduction, and bone repair, occurs once favorable biologic conditions have been established (Figs 3-1a and 3-1b). This naturally poses the problem of defining criteria necessary for periodontal stability in the four following situations:
• Healthy periodontium
• Pathologic periodontium (periodontitis)
• Treated periodontium
• Periodontium undergoing periodontal maintenance
The most reliable criterion in assessing the stability of periodontal health is the absence of inflammation; this is generally demonstrated through the absence of bleeding on probing.
Criteria to evaluate periodontitis can be divided into four categories:
• Criteria used to assess the degree of inflammation
– gingival appearance
– presence of bleeding on probing
– tooth mobility
• Criteria used to assess infectious etiology, as well as host susceptibility
– presence of bacterial plaque
– presence of pathogens
– risk factors
• Criteria used to assess degree of severity
– amount of bone destruction
– amount of attachment loss
– presence of deep periodontal pockets
– tooth mobility
– tooth displacement
• Criteria used to assess complexity
– associated local factors
– functional factors
– esthetic factors
A treatment is considered successful when it changes the intensity of all features of disease. Some signs are totally reversible, others are not.
The purpose of elaborating evaluation criteria is for the assessment of treatment success. Treatment is considered successful when all reversible signs of disease have disappeared.
• Reduced plaque indices indicates reduced plaque loads and change in flora composition.
• Absence of bleeding on probing indicates reduced inflammation.
• Attachment gain indicates tissue response and initiation of reparative processes.
• Probing depth reduction indicates gingival retraction and attachment gain.
These criteria also help in assessing whether conditions suitable for periodontal stability have been achieved or not. These conditions are as follows:
• Host-bacteria balance has been reestablished.
• Conditions favorable to efficient plaque control have been attained.
• Risks factors are controlled.
Periodontium undergoing periodontal maintenance
The goal of supportive therapy is to prevent disease recurrence. Recurring inflammation is reversed by professional supportive therapy and does not systematically lead to a new period of destruction.
A site displaying repeated bleeding on probing more than likely presents attachment loss (Baderston et al 1985). The only reliable criterion for periodontal site stability is complete and sustained absence of bleeding on probing.
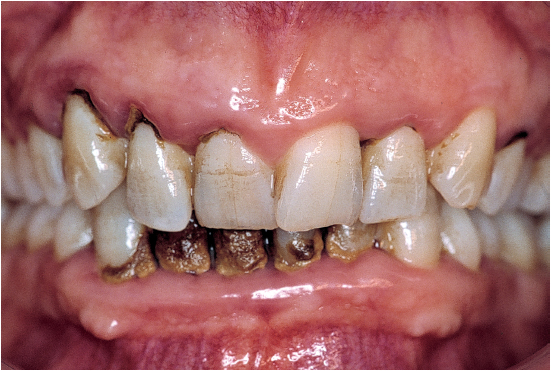
Fig 3-1a Periodontitis left untreated is characterized by a number of clinical and radiographic signs. These signs reflect the presence of inflammation (redness, swelling, bleeding), the level of severity (gingival recession, pockets, dental mobility and migrations, destruction), and infection (plaque deposits).
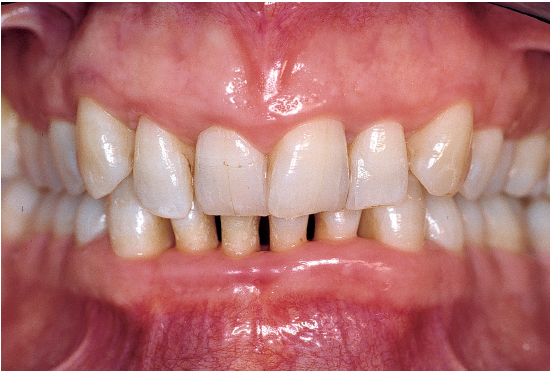
Fig 3-1b Clinical signs of inflammation are completely reversible; bleeding on probing disappears last. Successful management is characterized by progressive reversal of these clinical signs. Signs of destruction, on the other hand, are never totally reversible. At best, some amelioration can be observed (attachment gains, reduced migrations and mobility).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses