Clinical features
i. The posterior region of mandible is more commonly affected than the maxilla due to the microanatomy and reduced vasculature of the mandible.
ii. Intermittent swelling and drainage extraorally.
iii. Intense pain may occur; pain is of severe, boring type, which may continue for weeks or months.
iv. Swelling of face results from secondary infection.
v. Trismus, fetid odour and pyrexia can be noted.
vii. Persistently draining sinuses.
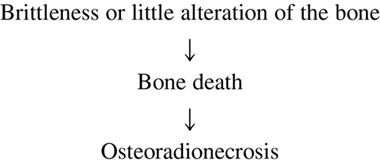
viii. Exposure of bone is the hallmark of osteoradionecrosis.
ix. The exposed bone becomes necrotic as a result of loss of vascularity from periosteum and subsequently it sequestrates.
x. Pathological fractures of bone is common.
xi. Osteoradionecrosis is treated by hyperbaric oxygen therapy.
Q. 2. Describe radiation protection measures.
Or
Discuss radiation protection.
Or
Discuss the methods of radiation safety and protection of the operator, patient and public.
Or
Discuss the different methods of radiation protection of the patient and personnel (operator) in oral radiography.
Ans. Various measures of radiation protection for patient, operator and associated personnel are as follows:
Protection of the patient
Mandatory steps during routine diagnostic radiographic examination are as follows:
• Despite the low risk to the patient from dental radiography, it is always best to keep exposure to ionizing radiation to a minimum. Hence, the ALARA concept should be kept in mind when exposing dental films. This can be achieved by:
i. X-ray machines: Only use good machines by reputed manufacturing companies.
ii. Only radiograph should be taken when required and avoid repeating the radiographic examination.
iii. Film selection: Good quality, highly sensitive films like F and E-speed films should be used.
In dental practice today only the type ‘E’ or the Ektaspeed is recommended, since it reduces the exposure by at least 40% as compared to type D.
iv. Filtration: Filtration removes the low energy X-rays from the beam. These “soft” X-rays are absorbed by the patient and do not contribute to the image; removing them before they reach the patient reduces the radiation exposure.
Units operating at 70 kVp or above should have filtration equivalent to 2.5 mm of aluminium and those operating below 70 kVp should have the equivalent of 1.5 mm of aluminium.
v. X-ray collimation: Collimation should be used to prevent scattering. The beam should be collimated so that it is no more than 7 cm in diameter at the patient’s face. Rectangular collimators further reduce the amount of tissue irradiation.
vi. Intensifying screens: Use of rare earth screens reduces dosage for extraoral films like, lateral cephalogram, OPG, lateral oblique, etc.
vii. Grids: The use of grids reduces the fogginess of the film due to secondary radiation, thereby reducing the need for repeat films. Good consistent processing technique also helps in preventing unnecessary repetitions.
viii. Kilovoltage: X-ray units should be operated using at least 60 to 90 kVp. Using an X-ray beam with low kilovoltage results in higher patient doses, primarily to the skin.
ix. Position-indicating devices:
• The cone-shaped devices should be replaced by long, open-ended, lead-lined cylinders.
Open-ended, circular or rectangular lead-lined cylinders are preferred for directing the X-ray beam.
• A long (12 to 16 inches) position-indicating device (PID) will reduce exposure to the patient better than a short (8 inch) PID, because there will be less divergence of the beam.
x. Lead aprons having lead (Pb) content equivalent to 0.25 mm aluminium should be worn by the patient while taking radiograph.
xi. Use of thyroid collars will protect the thyroid gland from radiations.
Protection of the operator
• hold the film in the patient’s mouth during exposure
• stabilize the X-ray machine during exposure
• stand near or directly in the path of the primary radiation
• stand behind a lead barrier having 0.5 mm lead equivalent during exposure.
• stand 6 feet away from the primary X-ray beam in an area called the zone of maximum safety, which ranges from 90° to 135° with respect to the primary X-ray beam.
• have radiation exposure periodically monitored by using personnel monitoring devices or film badges.
• work on rotation of duties, so that continuous accidental exposure is avoided.
iii. There are exposure limits for occupationally exposed radiation workers. The maximum permissible dose (MPD) is the dose of radiation to the whole body that produces very little chance of somatic or genetic injury. The MPD for whole body exposure per year for occupationally exposed personnel is 0.05 Sv(5 rem).
Protection of other persons
i. Only people whose presence is required should stay in room.
ii. Plan and design maxillofacial radiology department. Conch shell design of the operatory area is recommended to protect people in surrounding areas from radiation.
iii. An X-ray tube should be away from doorways to avoid accidental exposure.
iv. Radiation exposure to the room and to adjacent office premises should be monitored.
v. The walls of the room should be reinforced with barium plaster or the thickness of the walls should be increased by using an additional layer of bricks.
Q. 3. Discuss types of biologic effect of X-rays.
Ans. Biological effects of radiation can be considered under the following headings:
Classification 1
A. Somatic: The effect of radiation,which occurs in exposed individuals during their lifetime, is called somatic effect.
Except reproductive cells, all the cells in the body are known as somatic cells.
a. Stochastic effect: It includes increase in probability of occurrence of biological effect with increasing absorbed dose rather than its severity. They occur as direct effect of dose.
b. Non-stochastic effects or Deterministic effect: It is one in which severity increases with increase in absorbed dose in affected individual.
B. Genetic: The effect, which is manifested in the future generations of the exposed individuals, is known as genetic effect.
The reproductive cells are termed genetic cells.
Classification 2
Somatic effects
• These are the effects in which probability of the occurrence of a change increases, rather than its severity.
• These are effects that are likely to occur and are dose dependent. There is as such no threshold dose for stochastic effect.
• When the body is exposed to any amount of radiation, damaging effect may be induced. Lower the radiation dose, there is less possibility of cell damage.
E.g.: Radiation-induced cancer is a stochastic effect because greater exposure of a person or population to radiation increases the probability of cancer but not its severity.
b. Somatic Deterministic Effects or Non-stochastic Effects
• Effects that have increased probabilities of occurrence increasing with increase in dose and have dose threshold below which the response cannot be seen are known as non-stochastic effects.
• They result from specifically high doses of radiation, e.g. during radiotherapy.
• Ulceration and desquamation of skin resulting in reddening of skin, damage to connective tissue, blood vessels and glands, damage to alveolar bone and formation of cataract are all the examples of this effect.
Genetic effects
• Genetic effects are not seen in the person irradiated but are transferred to future generation.
• Generic cells are germ cells of the reproductive organs. Reproductive cells are prone to damage with comparatively much smaller dose than amount needed to produce radiation effect in somatic cells of the body.
• Radiations cause fragmentation of chromosomes and mutation of genes of sex cells and these mutant genes with altered characteristics pass on to next generation.
• Mutations are the changes in the information carried by the chromosomes within the germ cells, i.e. sperm and egg cells. It is indicative of change in the DNA of the cells.
• It may result in congenital abnormality in the offspring of the person irradiated. There may be retardation of growth rate.
• Doubling dose: This is the dose that causes complete doubling of all gene mutations.
• Damage can be caused to either dominant or recessive genes. The dominant variety effect is seen in next generation, whereas recessive variety effect may be seen after several generations.
• Genetic damage follows non-threshold type of response, i.e. small amount of radiation has the potential to produce lesser number of mutations in chromosomes.
• Genetic damage is cumulative and it cannot be repaired.
• Human embryo is said to be most sensitive especially during 15–42 days of its life, so radiation is avoided during pregnancy.
• Sterility in human beings has been reported on exposure to heavy doses.
• No genetic effect is seen in individuals beyond the age of reproduction.
Acute or short-term effects
• Acute somatic effects will be manifested within few hours to few days of acute irradiation and the severity of the effect will depend upon dose and dose rate.
• Following the latent period, effects are seen within minutes, days or weeks.
• Acute radiation effect is short-term effect. It occurs when large dose of radiation given in short period of time as in atomic bomb explosion and in nuclear accidents.
• Short-term effect is not applicable to the dentistry as dental diagnostic radiographs use less than 5 rads.
Factors modifying the acute effect are as follows:
• Sensitivity: It is determined by the sensitivity of parenchymal cells. If continuously proliferating tissues are irradiated with a moderate dose, cells are lost primarily by mitosis-linked death.
• Proliferative rate: The extent of cell loss depends upon the damage to the stem cell pools, and the proliferative rate of cell population.
Immediate effects of radiation are as follows:
i. Skin: Excessive exposure causes dermatitis. Repeated exposures have a cumulative effect. Dryness, erythema, thickening, desquamation and cracking of hands may also occur.
ii. Finger nails: Fingernails may become brittle, develop longitudinal fissures and ridges, and finally crumbled.
iii. Hair: Radiation causes epilation. It is often seen in association with dermatitis. Hair loss can be permanent.
iv. Blood-forming tissue: The bone marrow and lymph nodes are susceptible to excessive exposure, and it can manifest itself as change in blood count. The usual blood picture is leukopenia.
v. Eyes: Radiation dose can cause cataract and larger doses can cause detached retina.
Chronic or long-term effects
Chronic effects are mainly due to low level of irradiation for longer period, or chronic irradiation.
Pathogenesis of long-term effect
• Irradiation of capillaries causes swelling, degeneration and necrosis.
• It increases the capillary permeability and initiates a slow progressive fibrosis around the vessels.
• Due to this, deposition of fibrous scar tissue increases around the vessels, leading to premature narrowing and eventual obliteration of vascular lumen.
• This impairs the transportation of oxygen, nutrients and waste products, and results in death of all cells.
• This leads to loss of function and reduced resistance to infection and trauma.
Pathologic effects
The long-term effects are associated with small amount of radiation absorbed over long period of time. The abnormalities induced by repeated low levels of radiation exposure are as follows:
• Carcinoma: The cancer of skin is the earliest form of radiation-induced malignant tumour.
• Leukaemia: It is one of the late effects and can be due to primary and secondary radiation. A higher incidence of leukaemia is observed in radiologists as compared to others.
• Necrosis: Due to heavy radiations, destruction of tissue can occur. Necrosis can be seen in extraction socket after radiation exposure.
• Retardation of growth: Irradiation of developing teeth results in disorganization of the odontoblasts. With larger doses retardation of bone and tooth development is more obvious.
• Effect on the taste buds: Taste buds are very sensitive to radiation and soon degenerative changes begin. Loss of taste is very common.
• Effect on the salivary glands: The parenchymal component of salivary gland is more radiosensitive. Exposure to radiation leads to injury of these parenchymal cells leading to following conditions:
Q. 4. Write in detail about harmful effects of radiation on whole body.
Or
Mention radiation hazards affecting whole body. How would you protect patients from these while taking intraoral radiographs.
Or
What are the hazards of radiation seen on skin and bone? Discuss briefly protection of patient from radiation.
Ans. When the whole body is exposed to low or moderate dose of radiation, characteristic changes called acute radiation syndrome develop.
Acute radiation syndrome
Prodromal period
• After exposure of 1.5 Gy within the first few minute to few hours, symptoms characteristic of gastrointestinal tract disturbance occur, such as anorexia, nausea, vomiting, diarrhoea, weakness and fatigue.
• They are dose-dependent; higher the dose, the more rapid onset and greater is the severity of symptoms.
Latent period
Haematopoietic syndrome
• Whole body exposure of 2 to 7 Gy causes injury to the haematopoietic stem cells of the bone marrow and spleen. It causes rapid and profound fall in the number of circulating granulocytes, platelets and erythrocytes.
• Common signs: Infection, haemorrhage and anaemia. Death can result from this syndrome usually 10 to 30 days after irradiation.
As periodontitis may be the likely source of entry of microorganism in the blood stream, the role of dentist is very important. The removal of source of infection by administration of antibiotics should be attempted at the earliest.
Gastrointestinal syndrome
• Exposure of whole body in the range of 7 to 15 Gy causes extensive damage to the gastrointestinal system.
• It causes considerable injury to the rapidly proliferating basal epithelial cells of the intestinal villi and leads to loss of the epithelial layer of the intestinal mucosa. Due to this denuded mucosal surface, plasma and electrolytes are lost, and efficient intestinal absorption is impaired.
• Signs and symptoms include ulceration following haemorrhage of the intestine. All these changes lead to diarrhoea, dehydration and loss of weight.
Bone marrow depression
Endogenous intestinal bacteria readily invade the denuded surface producing septicaemia. By this time, the developing damage to the gastrointestinal system reaches a maximum, the effect of bone marrow depression begins to manifest.
Lowering of body defence
By the end of 24 hours, the number of circulating lymphocytes falls to a very low level. This is followed by the decrease in the number of granulocytes and platelets. This hampers body defence mechanism against bacterial infection and decreases the effectiveness of the clotting mechanism.
Death
The combined effect on these stem cells causes death within 2 weeks due to fluid and electrolyte loss, infection and possible nutritional impairment.
Cardiovascular and central nervous system syndrome
• Exposure in excess of 50 Gy can cause death in 1 to 2 days. Human beings show collapse of the circulatory system with precipitous fall in blood pressure in the hours preceding death.
• Victims may show intermittent stupor, incoordination, disorientation and convulsion suggestive of extensive damage to the nervous system.
• This syndrome is irreversible and clinical course may run from only few minutes to about 48 h before death commences.
Management of acute radiation syndrome
• Antibiotics: Antibiotics should be started when infection threatens life or the granulocyte count falls.
• Fluid supplements: It is necessary to replace fluid and electrolytes.
• Blood transfusion: Whole blood transfusion is given to treat anaemia.
• Platelet: Administration of platelet to arrest thrombocytopenia.
• Bone marrow grafts: Bone marrow grafts are indicated for identical twins because there is no risk of graft-versus-host response.
Protection of the patient
Mandatory steps during routine diagnostic radiographic examination are as follows:
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses