2
Background Description and Epidemiology
Background
Dentistry and dental treatment have always been associated with pain and anxiety, probably because treatment used to be extremely unpleasant and painful before the development of today’s modern techniques and anaesthetics. However, despite the invention of new equipment and less unpleasant treatment techniques during the twentieth century, dental fear, anxiety and phobia are still serious problems affecting a significant part of the population and are among the most frequent fears in western countries (Smith and Heaton 2003).
Since dental avoidance and reduced oral health reflect the serious consequences of dental anxiety, an increased interest for research into this field has evolved during the last decade. From its origin within natural science, a growing sector of behavioural research is now emanating in dentistry. This research includes a variety of problems of importance for the quality of services delivered by the dental profession, such as general psychology, clinical communication, the patient–dentist relationship, dental fear and anxiety, patient satisfaction and quality of life.
This development also reflects the recognition of the soul and body as one biological entity, that somatic and psychological processes are integrated and thereby the great impact of fear and anxiety reactions on all aspects of health. This holistic view has also been important for the trend that oral health care is becoming more and more integrated in general health care, reflecting that the oral cavity is part of the body and its functions are based on the same biological processes.
Dental Fear, Dental Anxiety and Dental Phobia
Even though the terms ‘fear’, ‘anxiety’ and ‘phobia’ are frequently used interchangeably in the literature, it may be practical to define them separately in the clinical dental setting. For example, a distinction should be made between dental fear, a natural emotion usually seen in small children, and dental anxiety and phobia, a disorder-like phenomena among more mature children and adults because the treatment approach (psychological and dental) should be different.
Fear is a normal emotional response to objects or situations perceived as genuinely threatening (Draper and James 1985). The response involves activation of the sympathetic branch of the autonomic nervous system, making the individual prepared for fight or flight, which is seen as a normal preventive reaction. Fear should therefore be considered as rational.
Anxiety has similar physical and behavioural components as fear, but it occurs without a present triggering stimulus. Anticipation of future events associated with previous negative experiences is frequently the reason. The response is irrational since there is no immediate threat, but it may be estimated as priming for a future fear response. In cases where the anticipatory anxiety reaction is strong and irrational, it may be regarded as a disorder.
Phobia is a clinical mental disorder according to the diagnostic criteria (DSM-IV or ICD-10). Among the criteria are: subjects display an extreme and persisting fear of clearly discernible objects or situations, avoidance behaviour and interference with daily life.
Consequences
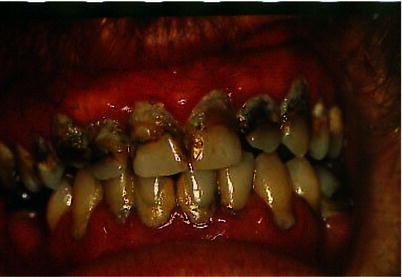
The most obvious consequence of dental fear, anxiety and phobia is the avoidance of dental treatment. A number of studies has shown the relationship between dental anxiety problems and cancelled and missed dental appointments (Armfield, Stewart and Spencer 2007; Berggren and Meynert 1984; Skaret et al. 1999). Avoidance behaviour may have consequences for the patients’ oral health with pain and deteriorated teeth (Figure 2.1) and patients with dental anxiety disorders generally have reduced oral health (Agdal et al. 2008; Berggren and Meynert 1984; Schuller, Willumsen and Holst 2003). Healthy teeth and regular dental visits are among the accepted norms in modern society and dentition is also an important aesthetic factor. Poor oral health and awareness of a dental avoidance problem may therefore give rise to embarrassment, reduced social functioning and possibly reduced quality of life (Berggren 1993; Crofts-Barnes et al. 2010; Locker 2003).
Figure 2.1 A 35-year-old male odontophobic patient with long-time avoidance of dental care
Measurement of Dental Fear and Anxiety
Before discussing the prevalence of dental fear, anxiety and phobia it is necessary to discuss how these concepts may be measured.
The multidimensional responses of dental fear and anxiety involve cognitive, emotional, behavioural and physiological components and measurement techniques try to evaluate all, or some, of these components. Many measurement techniques are in use, such as self-report questionnaires, behavioural ratings, physiological measures and projective techniques. Most population studies are based on self-report questionnaires (dental anxiety scales), which have been composed in an attempt to tap all components in dental fear and anxiety and tested for their reliability and validity characteristics. These instruments are also used by clinicians for screening purposes among their patients. Based on studies that have tested the construct validity of the scales, some of them have certain cut-off scores to define high dental anxiety or phobia. However, since the constructs of the existing scales vary greatly and none of them are considered perfect for tapping the multidimensional aspects of anxiety and phobia (Armfield 2010a, Newton and Buck 2000), the prevalence of dental fear, anxiety and phobia varies a lot in the literature.
The scales can be divided into adult dental anxiety scales and child-specific dental anxiety scales. Among the adult dental anxiety scales, the Dental Anxiety Scale (DAS) (Corah, Gale and Illig 1978) is the most widely used. It consists of four items, each of which the subjects rate on a five-point scale from A (calm) to E (terrified). The first two questions relate to the anticipation of having a dental appointment tomorrow and sitting in the waiting room, whereas the last two questions relate to anticipated fear of specific stimuli in the dental chair. The total score of the scale varies from 4 to 20. Corah et al. (1978) suggested a score above 13 as an indicator of high dental anxiety, but various cut-offs have been used in population studies as indicated in Table 2.2.
The Modified Dental Anxiety Scale (MDAS) (Humphris, Morrison and Lindsay 1995) is a modified version of the DAS scale, in which a fifth item related to the receipt of local analgesia is included. Since the alternative answers in the DAS differ among the questions, thus making them difficult to compare, the MDAS has the same answers for all questions in a clear order of anxiety: Not anxious – Slightly anxious – Fairly anxious – Very anxious – Extremely anxious. Fear of injections is an important factor in dental anxiety and phobia and the MDAS therefore seems to be an improvement compared to the DAS. However, the DAS scale is still the most extensively used.
The Dental Fear Survey (DFS) (Kleinknecht, Klepac and Alexander 1973) is the second-most common self-report measure of dental anxiety. The present scale (Kleinknecht et al. 1984) has 20 items reflecting a variety of symptoms of dental fear and anxiety. Two items focus on avoidance, five items are related to physiological arousal, 12 items assess fear of specific dental stimuli and the last item taps overall fear. In population studies the individual item scores are summed into a total score varying from 20 to 100. Cut-off for high dental anxiety has been suggested to be 60 or more (Milgrom, Getz and Weinstein 1988; Milgrom et al. 1990). In clinical use among individual patients the single items are used to help the clinician understand the type of fear.
The Index of Dental Anxiety and Fear (IDAF-4C) is a new theoretically derived instrument developed to measure a person’s level of dental fear (Armfield 2010a, 2011b). The scale assesses emotional, behavioural, physiological and cognitive components of the anxiety and fear response and it is claimed to have a stronger theoretical basis than other scales.
The Dental Belief Survey (DBS) (Smith et al. 1987) is a 15-item instrument that assesses the patient’s attitudes to dental personnel and dental treatment, e.g. to what extent they feel that the dentist is rushing, not listening to the patient and putting the patient down. A DBS score of 48 or more has been classified as high, meaning that the patient has a feeling of distrust of the dentist (Milgrom, Vignehsa and Weinstein 1992). A revised version of the scale, the Dental Belief Survey – Revised (DBS-R) containing 28 items, was later suggested by the same group of researchers (Milgrom, Weinstein and Getz 1995). Both scales have been evaluated and found to have good psychometric features. Results from a Swedish study point towards the use of the 28-item DBS-R since this scale measures an overall construct of patients’ attitudes and feelings related to dentists and dentistry (Abrahamsson, Ohrn and Hakeberg 2009).
Among the variety of other self-report questionnaires for measuring dental fear and anxiety among adults, but not so frequently reported in the literature, is the Dental Anxiety Inventory (DAI) (Stouthard, Hoogstraten and Mellenbergh 1995). There are two versions, a full scale with 36 items covering three facets of dental anxiety (time, situation, reaction) and a short version with nine items (DAI-S). Good reliability and validity have been established for both scales (Aartman 1998; Stouthard et al. 1995). Also a number of single-item self-report measures of dental fear and anxiety have been published.
Among the child-specific dental anxiety scales, the Child Fear Survey Schedule – Dental Subscale (CFSS-DS) (Cuthbert and Melamed 1982) is by far the most widely used. The scale, which has 15 items scored on a Likert scale from 1 to 5, is a modification of the more general Child Fear Survey Schedule (CFSS) (Scherer and Nakamura 1968). The test is used in two versions: a self-report by the child version and a parental version. Different cut-off scores for high dental anxiety have been suggested. In a Swedish study among children aged 4–14 years, sum scores of 38 or more in the parental version were found to be associated with negative behaviour in the clinic (Klingberg 1994).
Behavioural rating is frequently used in child populations since behaviour management problems are so frequently linked to dental anxiety (Klingberg and Broberg 2007). The most commonly used is the Frankl scale (Frankl, Shiere and Fogels 1962), by which the behaviour is rated in one of four categories from 1 (definitely negative) to 4 (definitively positive). Examples of projective scales that are used among children are the Venham Picture Scale (Venham and Gaulin-Kremer 1979) and the Facial Image Scale (Buchanan and Niven 2002). Physiological techniques (e.g. heart rate, basal skin response, muscle tension) are usually restricted to specific test situations.
Prevalence
The prevalence of dental anxiety has been explored in a variety of populations and cultures during the last 30 years (for review see Klingberg and Broberg 2007; Smith and Heaton 2003). Results from the literature review by Smith and Heaton (2003), indicates stability in dental anxiety scores over time. They found neither a significant increase, nor a decrease in self-reported anxiety levels among US college students. The results from a great number of prevalence studies over time have indicated a similar situation in other parts of />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


