17 Prominent chin and TMJDS
Summary
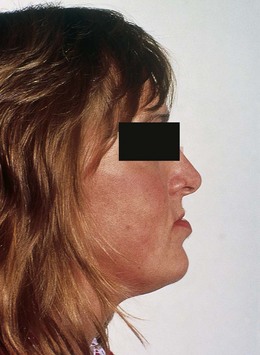
Jocelyn, aged 23, is referred by her general dental practitioner because of her prominent chin (Fig. 17.1) and pain in her left temporomandibular joint (TMJ). What are the causes and how would you manage these problems?
History
Examination
Extraoral examination
 What do you observe from Jocelyn’s profile view (Fig. 17.1)?
What do you observe from Jocelyn’s profile view (Fig. 17.1)?
Class III skeletal pattern with average FMPA. Competent lips.
 Based on the history, what other aspects would you assess extraorally?
Based on the history, what other aspects would you assess extraorally?
Temporomandibular joints. Opening and lateral mandibular movements should be assessed by first observing the patient from in front and second by palpation of the condylar heads while listening for the presence of crepitus or a joint click. As symptoms are present, the masticatory muscles should also be palpated. A left TMJ click and left masseteric tenderness were detected.
Intraoral examination
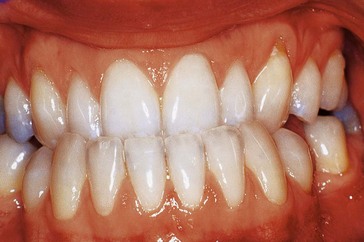
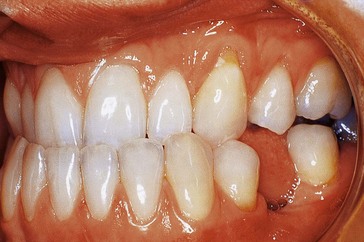
The intraoral views are shown in Figure 17.2.
 What do you see?
What do you see?
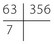
 What is the most likely cause of the considerable spacing in the lower premolar areas with
What is the most likely cause of the considerable spacing in the lower premolar areas with 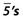 drifted into contact with
drifted into contact with 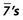 ?
?
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses



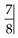 (centric relation to occlusion shift of ~3 mm).
(centric relation to occlusion shift of ~3 mm).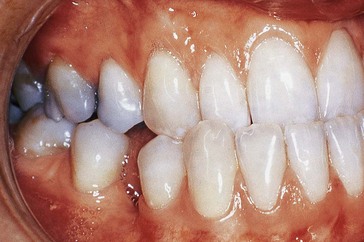
 .
.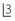
 are visible.
are visible.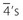 and
and 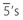 .
.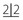 .
.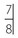 .
. in an uncrowded arch is the most likely explanation for the spacing. An uncrowded lower arch is common in Class III malocclusion.
in an uncrowded arch is the most likely explanation for the spacing. An uncrowded lower arch is common in Class III malocclusion.
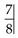 on closure. There are also anterior and posterior crossbites present.
on closure. There are also anterior and posterior crossbites present.
