chapter 17 Considerations for Implants in the Geriatric Patient
It has been predicted that there will be an increase in the proportion of people older than age 80 by the year 2020.1 Most elderly people are healthy and active, and many are seeking dental care to improve their oral function as they continue to age (Figure 17-1). Over the past decade, the number of patients presenting with more teeth and fewer prostheses has increased. This trend is the result of increased emphasis by dental professionals on prevention and the need for patients to improve their oral hygiene practices.2 However, the prosthodontic needs of elderly patients are extensive, and these patients will expect to maintain high standards of oral function.1
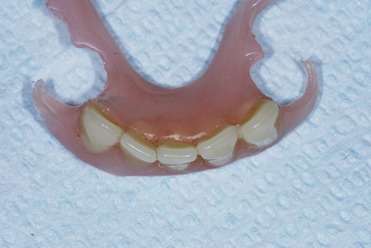
The use of removable dentures does not allow for adequate oral function in many geriatric patients, and these patients may have difficulty adapting to full dentures (Figure 17-2). Firmly retained, functional prostheses should be used in these patients for physiological and psychological reasons, as well as for the role that adequate oral function plays in proper digestion and nutrition.1 Patients who do not receive adequate oral rehabilitation to improve function and esthetics may withdraw from society and experience a loss of self-esteem.2
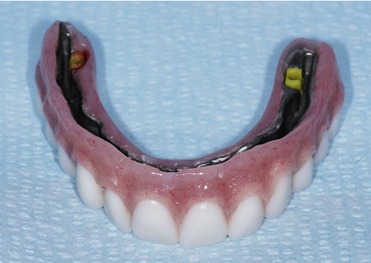
Dental implants and implant-supported prostheses have been used successfully in geriatric patients (Figure 17-3). In a study of implant placement in elderly patients, Kondell et al found that the success rate was similar to that found when implants were placed in younger patients.1 However, a single type of implant is not appropriate for all patients. The size, shape, quality, and quantity of bone are different in each patient. Clinicians who place dental implants in elderly patients must be aware of the systemic influences that affect alveolar bone and must understand bone physiology, metabolism, and the response of alveolar bone to systemic changes. It is important for clinicians to understand that alveolar bone responds similarly to systemic challenges as bone in other skeletal sites. Factors related to initial integration of the implants, such as maintaining vital osseous peri-implant margins, preserving subperiosteal osteogenic capacity, and stabilizing the implant firmly within bone, can be affected by the status of the alveolar bone and its associated structures.3
Age-related Considerations
As people age, their oral tissue undergoes change. Many physical, endocrine, and metabolic changes are associated with aging, and clinicians must be aware of how these changes can affect implant placement in older patients. Geriatric patients may present with a variety of problems that are not encountered when one is treating younger patients. Severe resorption of the alveolar process usually occurs following tooth loss in the posterior maxilla, resulting in an inadequate amount of bone for implant placement.4 Common problems encountered in elderly patients include diabetes, which can cause decreased bone density; systemic disease and osteoporosis, both of which can cause alveolar bone loss; compromised oral tissues from irradiation, which can cause impaired wound healing; and xerostomia, which can contribute to plaque formation and an increased incidence of caries.2
In addition, many elderly patients present with a variety of nutritional deficiencies. Deficiencies in vitamins A, B, and C can result in decreased cohesiveness and integrity of the epithelial layer, reduction in cell metabolism, and poorly differentiated connective tissue cells and fibers, respectively, leading to friability of the oral mucosa. Vitamin B deficiency can lead to loss of papillae on the tongue. Deficient protein and zinc intake can cause a delay in the renewal of taste buds, resulting in a depressed sense of taste. Degeneration of the olfactory receptors in the roof of the nasal cavity also occurs with aging. Patients may not notice the decrease in their sense of taste and smell until the time of placement of a new prosthesis, when attention is drawn to the mouth. As a result, patients may blame the prosthesis for the decrease noted in these senses. Clinicians should obtain a written dietary history from their patients, including how food is prepared, to determine whether patients have satisfactory mineral intake to undergo implant surgery and the placement of prosthodontics.5
Smith et al studied the risks associated with the placement of dental implants to determine whether a medically compromised status, the age or gender of a patient, or the number of implants placed affected implant failure or led to an increased incidence of complications.6 They found that the patient’s medical status and the number of medical problems were not statistically associated with complications related to implant surgery or implant failure. However, patients with surgical ri/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses