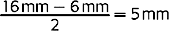Chapter 16 Single-Tooth Replacement: Treatment Options
Seventy percent of the dentate population in the United States is missing at least one tooth. Single-tooth replacement will most likely comprise a larger percentage of prosthetic dentistry in the future, compared with past generations. In 1960 the average American over age 55 years had just seven original teeth. Today the average 65 year old has 18 original teeth; however, baby boomers (those born between 1946 and 1964) can expect to have at least 24 original teeth when they reach 65 years of age. The first adult teeth lost today are usually between the ages of 35 and 54 years. Almost 30% of the 50 to 59 year olds examined in a U.S. national survey exhibited either single or multiple posterior edentulous spaces bordered by natural teeth.1 This segment of the population has the most disposable income and is the least dependent on insurance companies to pay for dental care. Treatment to replace single teeth in the posterior regions represents nearly 7% of the annual dental care reimbursement from insurance companies and totals more than 3.2 billion U.S. dollars each year.2,3
POSTERIOR MISSING TOOTH
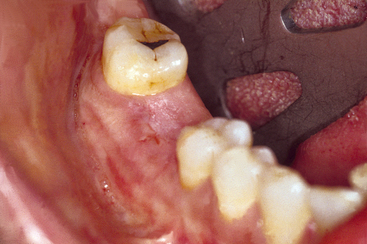
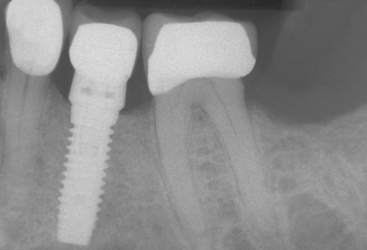
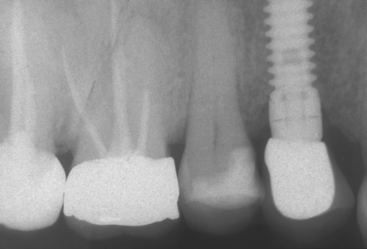
The first molars are the first permanent teeth to erupt in the mouth and often play a pivotal role in the maintenance of the arch form and proper occlusal schemes. These teeth are often the first to decay, and the adult patient often has had one or more crowns fabricated to restore the integrity of the tooth and replace previous large restorations. Longevity reports of crowns have yielded very disparate results, with the mean life span at failure reported to be 10.3 years. The primary cause of failure of the crown is endodontic therapy, porcelain or tooth fracture (or both), or uncemented restoration. The tooth is at risk for extraction as a result of these complications and is a leading cause of single posterior tooth loss in the adult1–9 (Figure 16-1).
POSTERIOR SINGLE-TOOTH REPLACEMENT OPTIONS
Evidence-based medicine is the conscientious, explicit, and judicious use of the best evidence in making decisions about the care of individual patients (Cochrane Center, Oxford, England).10 Over the years, researchers have observed that external clinical evidence would both invalidate previously accepted treatment and allow replacement with new modalities that are more efficacious and safe.10 An evidence-based approach may be applied to the replacement of a posterior single tooth.
Five alternative treatment options exist for the replacement of a posterior single missing tooth (Box 16-1). The interocclusal space must be assessed carefully, regardless of the treatment selected. Patients with insufficient vertical space may be contraindicated for any prosthesis without the prior correction of the occlusal plane and maxillomandibular relationships.
Removable Prosthesis
One option to replace a single missing tooth is a removable partial denture (RPD). A common axiom in restorative dentistry is to use a fixed prosthesis whenever possible.8 RPDs are usually indicated to replace spans of three or more posterior teeth or a missing canine and two or more adjacent teeth. Rarely does a patient consent to a RPD as an acceptable definitive substitute for one posterior single tooth.
The advantages of the removable restoration for multiple tooth loss include the following: ease of daily care of the adjacent teeth, the ability to have a soft tissue replacement around the missing tooth in esthetic zones with gross defects, maxillary lip support in gross defects, minimal preparation of the abutment teeth, and reduced cost (Box 16-2). However, no reported advantages exist for an RPD replacing one posterior tooth.
Removable prostheses do not maintain bone. The maxillary posterior teeth are often in the esthetic zone (especially the maxillary premolars), and bone loss may compromise the esthetic result. Function is not improved with a removable prosthesis replacing one or two teeth, so esthetics and the fear of other teeth shifting in the arch are the two primary reasons for the patient to consent to wearing the restoration. Because of its bulk and the need for cross arch stabilization, an RPD promotes more food debris and plaque accumulation on the adjacent teeth than any other treatment option (Box 16-3). No clinical reports are available to assess the longevity survival rate, complications, or survival of adjacent teeth for a single-tooth RPD in the posterior regions of the mouth. From an evidence-based approach, this procedure is not indicated.
Recently, Shugars et al.3 and Aquilino et al.11 have reported on survival rates of teeth adjacent to treated and untreated posterior-bounded edentulous spaces. When RPDs were used to replace teeth, the survival of the posterior teeth adjacent to the edentulous space were poorer than with any other treatment option, with ranges from 17% to 44% abutment tooth loss at 4.2 to 13.5 years.3,11–14 Patients electing not to wear the RPD may enjoy greater survival of the adjacent teeth than those wearing the removable prosthesis.
Resin-Bonded Fixed Partial Denture
A second option to restore a single missing tooth bordered by posterior natural teeth is a resin-bonded fixed partial prosthesis. The primary advantages of this restoration are the minimal preparation of the adjacent teeth and reduced cost (Box 16-4).
Failure rates reported in the literature are greatly disparate, but the majority of reports indicate a failure rate of at least 30% within 10 years and as high as 54% within 11 months.6,15–17 It also appears that earlier perforated designs exhibited lower survival rates (Box 16-5).
The majority of resin-bonded fixed partial denture (FPD) failure occurs from cement failure, with different regions of the mouth exhibiting various retention rates. The highest survival rates occur in the maxillary anterior, followed by mandibular anterior, maxillary posterior, and mandibular posterior teeth respectively.18 Therefore posterior tooth replacement is not as successful, compared with an anterior resin-bonded restoration. Debonding most often occurs during function; because eating is often a social experience, this may cause the patient embarrassment and insecurity. The selection of this option is usually driven by economics and the desire to maintain as much tooth structure as possible on the abutment teeth. This option is usually more accepted by the patient than the RPD, but it must be considered as a transitional restoration because of its high debonding rate.
Maintenance of the Posterior Space
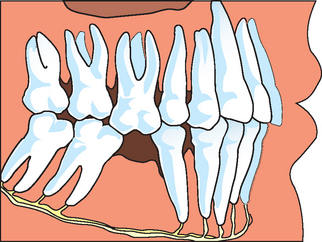
A third treatment option to restore missing posterior teeth is to not replace the tooth but instead to maintain the missing space. A common doctrine has been to replace a missing tooth to prevent complications such as tipping, extrusion, increased plaque retention, caries, periodontal disease, and collapse of the integrity of the arch8,14 (Figure 16-2). However, clinical studies evaluating the consequences of adjacent tooth loss indicate the loss of one or two teeth adjacent to a long-term edentulous space may range from 25% to less than 8% at 8 to 12 years.3,13,14 For example, Aquilino et al.11 reported an 18% 10-year tooth loss rate of adjacent teeth to a posterior missing tooth. The location of a missing posterior tooth often influences the prosthodontic treatment plan. In general, when third molars are missing, the author suggests not replacing a second mandibular molar19 (Box 16-6). The mandibular second molar is not in the esthetic zone of the patient. Ninety percent of the masticatory efficiency is generated anterior to the mesial half of the mandibular first molar, so function is rarely a primary reason to replace the second molar. A 10% greater occlusal force is measured on the second molar compared with the first. This tooth is more likely to exhibit working or nonworking interfaces during mandibular excursions. The crown height space decreases as it proceeds posteriorly and represents a limited access for implant placement, component, and prosthesis screw, especially when opposing a natural dentition. As a result of the increased forces, occlusal interferences, limited abutment height, reduced retention, and cement surface area, a greater incidence of porcelain fracture, uncemented restorations, or both exists. In addition, the course of the mandibular canal anterior to the midfirst molar corresponds to the level of the mental foramen. However, in the region of the second molar, its course becomes highly variable with an elevated risk of paresthesia and neurovascular bundle damage during implant surgery and insertion. The bone quality in the second mandibular molar region is often inferior to other regions of the mandible, with increased risk of bone loss or implant failure.20 The submandibular fossa topography mandates greater implant body angulation, with increased stresses at the crestal region of the implant, thereby increasing the risk of bone loss. Cheek biting is more common in this region because of the proximity of the buccinator muscle. The mandible exhibits increased flexure and torsion during opening or heavy biting on one side at this second molar site, and masticatory dynamics are less favorable. Finally, the cost of an implant and/or fixed prosthesis to replace the second molar often does not warrant the benefits achieved. As a consequence, the mandibular second molar is often not replaced when the third molar and second molar are the only posterior mandibular teeth missing.
Box 16-6 Disadvantages of Replacing a Mandibular Second Molar
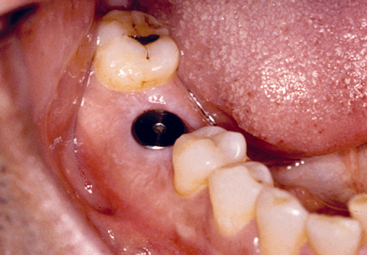
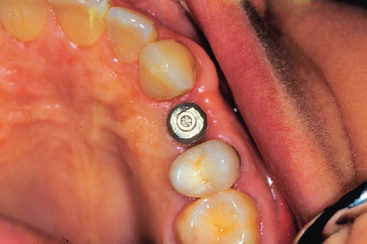
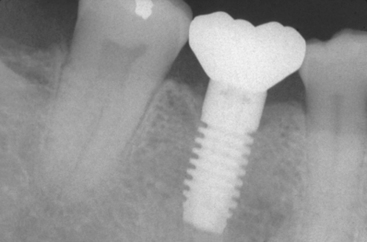
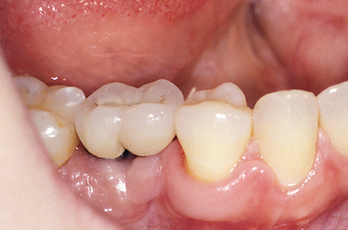
The mandibular second molar is usually replaced when the third molar is present and will remain in function (Figure 16-3). In addition, some patients desire an intact dentition and wish to have the tooth replaced (Figure 16-4). If the bone is abundant and no paresthesia risk is apparent, then the second molar may be replaced. However, this is usually the exception rather than the rule of treatment.
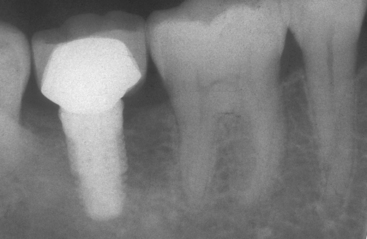
Figure 16-3 The second mandibular molar is usually replaced when the third molar is present and will remain in function.
Fixed Partial Denture
The treatment most commonly used for the replacement of a posterior single tooth is the three-unit fixed restoration. In 1990 more than 4 million FPDs were placed in the United States.21 This type of restoration can be fabricated within 1 to 2 weeks and satisfies the criteria of normal contour, comfort, function, esthetics, speech, and health. Because of these benefits, the FPD has been the treatment of choice for the last 6 decades.22,23 Few bone and soft tissue considerations exist in the missing tooth site. Every dentist is familiar with the procedure, and it is widely accepted by the profession, patients, and dental insurance companies (Box 16-7).
A three-unit FPD presents survival limitations to the restoration and to the abutment teeth.7 In an evaluation of 42 reports since 1970, Creugers et al.23 calculated a 74% survival rate for FPDs for 15 years. Walton et al.24 and Schwartz et al.25 reported mean life spans (50%) of 9.6 and 10.3 years, respectively. Scurria et al.26 performed a metaanalysis of several reports at 10 to 15 years and found 30% to 50% failure within these time frames. However, reports are very inconsistent with as little as 3% loss over 23 years to 20% loss over 3 years.4,5,23–26
When a tooth is prepared for a crown, a 5.7% risk of irreversible pulpal injury and subsequent need for endodontic treatment exists.27 In addition, the crown margin next to the pontic is more at risk of decay and the need for endodontics as a result. Caries and endodontic failure of the abutment teeth are the most common causes of prostheses failure.22,24,26 Researchers have observed that abutment teeth for an FPD fail from endodontic complications more often than those with vital pulps.28–30 Caries on the crown primarily occurs on the margin next to the pontic. A low percentage of patients floss on a regular basis, and those using a floss threader are even fewer.30 As a result, the pontic acts as a large overhang next to the crown and a reservoir for plaque. Up to 15% of abutment teeth for a fixed restoration require endodontic therapy, compared with 3% of nonabutment teeth with crown preparations31 (Box 16-8). The long-term periodontal health of the abutment teeth may also be at greater risk, including bone loss.
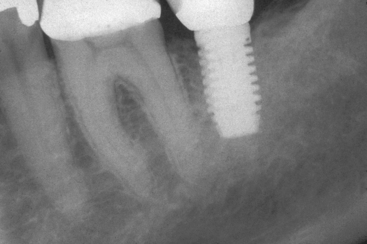
Unfavorable outcomes of FPD failure include not only the need to replace the failed prosthesis but also the loss of an abutment and the need for additional pontics and abutment teeth in the replacement bridge. Because 15% of FPD abutment teeth require endodontics, and root canal therapy is 90% successful at the 8-year mark, many abutment teeth may be lost (Figure 16-5).
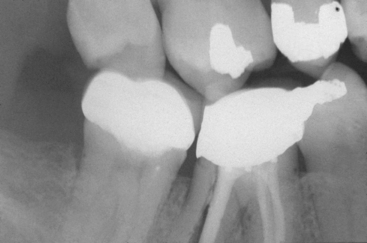
Figure 16-5 The most common cause of single-tooth loss is endodontic failure or fracture after endodontic therapy.
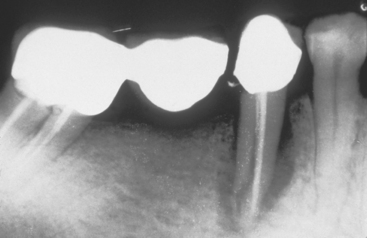
The abutment teeth of an FPD may be lost at rates up to 30% for 8 to 14 years.3,13,14 Recent reports indicate 8% to 18% of the abutment teeth holding an FPD are lost within 10 years (Figure 16-6). This is most disturbing, because 80% of abutments have no previous decay or are minimally restored before the fabrication of the FPD.6 Some contraindications for a posterior fixed partial prosthesis are included in Box 16-9.
Single-Tooth Implants
The fifth treatment option to replace a posterior single missing tooth is a single-tooth implant. For years patients were advised to set their desires aside and accept the limitations of an FPD. However, many feel the most natural method to replace a tooth is to use an implant, rather than preparing adjacent teeth and joining them together with a prosthesis. The primary reasons for suggesting the FPD were its clinical ease and reduced treatment time. However, if this concept were expanded, then extractions would replace endodontics and dentures could even replace orthodontics. The primary reason to suggest or perform a treatment should not only be related to treatment time or difficulty to perform the procedure but also should reflect the best possible long-term solution for each individual (Figure 16-7).
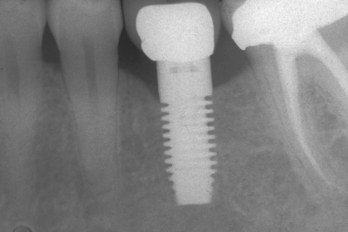
Figure 16-7 A single-tooth implant is usually the best treatment option to replace a posterior missing tooth.
Before 1990 few long-term studies focusing on single-tooth implant replacement with osteointegrated implants in any region of the mouth had been published. Early reports indicated single-tooth implant results were less predictable than they have become in the last 10 years. For example, in 1990, Jemt et al.32 reported a 9% implant failure within 3 years of prosthesis completion on 23 implants with screw-retained restorations (21 in the maxilla, two in the mandible). In 1992, Andersson et al.33 published a preliminary report of a prospective study of 37 implants restored with cemented single-tooth crowns in 34 patients. A 3-year follow-up included this “developmental group” and an additional 23 patients with 28 crowns. The cumulative success rate recorded was 93.7%, with 89% of the developmental group in function 3 to 4 years.33
From 1993 to the present time, single-tooth implants have become the most predictable method of tooth replacement. More refereed reports exist in the literature than for any other method of tooth replacement. Most all 5-year reports demonstrate a higher survival rate than for any other method of tooth replacement. For example, in 1993, Schmitt and Zarb34 reported no failures for 40 implants placed in 32 patients (28 in the maxilla, 12 in the mandible, with 27 in the anterior region and 13 in the posterior). After a period of up to 6.6 years, all implants were in function. In 1994, Ekfeldt et al.35 reported a 4- to 7-year retrospective study of 77 patients who received 93 implants. The restorations were cemented or screw retained. Two implants were lost, both within the first year of function. In the same year, Cordioli et al.36 evaluated 67 endosteal implants for single-tooth replacement over a 5-year period and observed an implant loss of 5.6%. In 1995, Haas et al.37 also reported on 76 single-tooth implants observed for 6 years with a 2.6% implant loss.
A series of reports in 1991, 1994, and 1996 reported on a multicenter prospective study consisting of 92 patients who received 107 implants with a cumulative survival rate of 97.2% at 3 and 5 years.38–40 The mean marginal bone loss (measured from the first thread, which is 2 mm below the crestal bone) did not exceed 1.0 mm. Plaque and gingival indices were indicative of soft tissue health. The most frequent complication was loosening of the abutment fixation screw, and this complication was significantly reduced after the first year.
Becker et al.41,42 reported more than 90% success in a study over 4 years and 282 molar implants. Simon43 observed 70 molar implants over a period ranging from 6 months to 10 years, with a 97.1% success rate. Levin et al.44 reported in 2006 on single-molar replacement with implants over a longer period, with a 93.6% success rate.
A multicenter prospective clinical study was initiated with the Maestro Dental Implant System from BioHorizons in 1996.45 Thirty-eight implants were placed in the posterior regions of the jaws: 15 in the maxilla and 23 in the mandible. These included six second molars (four maxillary and two mandibular), 22 first molars (six maxillary and 16 mandibular), seven second premolars (three maxillary and four mandibular), and three first premolars (two maxillary and one mandibular). All crowns were cement retained. The implant survival rate was 100% at the 5-year follow-up. The mean bone loss from implant insertion to uncovering was 0.4 mm from the original crest of the ridge, the additional mean bone loss over the first 1 year of loading averaged less than 0.3 mm, and no bone loss over the following year was observed. No incidence of abutment screw loosening or fracture of any components was observed in this study. In 2000, Misch et al.46 reported on 30 single-tooth implants with this same implant system in the posterior maxilla, with 100% survival rate over a 5-year period. In 2006, Misch et al.47 found the 100% survival rate for single-tooth implants was maintained for as long as 10 years.47
A 10-year report by Priest6 indicated the posterior single-tooth implant was more than 97% successful. Perhaps of more significance, no adjacent teeth loss from endodontic failure or caries occurred, and only one tooth required endodontic therapy after implant insertion. This report clearly identifies that the adjacent teeth are least at risk when the missing tooth is replaced with an implant.
Although posterior single-tooth replacement is a relatively new treatment alternative, more articles have been published than for any other treatment alternative. If early reports are excluded, then survival rates reported range from a low of 94.6% to a high of 100% for 1 to 10 years. A review of the literature by Goodacre et al.48 from 1981 to 2003 found single-tooth replacement with an implant had the highest implant prosthesis survival rate and averaged 97% survival. The most common complication reported was abutment screw loosening, which did not cause the prosthesis or implant to fail.
The single-tooth implant exhibits the highest survival rates of the five treatment options presented for single-tooth replacement. In addition, the adjacent teeth have the highest survival rate and the lowest complication rate, which is a considerable advantage (Figure 16-8). On the other hand, the longevity of the implant crown has not been adequately determined, because these reports do not extend as long as those of other treatment options. However, 10-year data clearly indicate an implant and its associated crown has greater survival than an FPD.
Despite some limitations and obvious clinical challenges, the posterior single-tooth implant represents a highly desirable and justified treatment option. In addition, cost comparison studies conclude that the implant restoration demonstrates a more favorable cost-effectiveness ratio.6,48–49 When adjacent teeth are healthy or are able to be restored, or when the patient refuses their preparation for the fabrication of a traditional three-unit fixed partial restoration, a posterior single-tooth implant is an excellent solution. As a consequence of not preparing the adjacent teeth for crowns, many additional advantages are incurred. These advantages include the decreased risk of caries and endodontics treatment on the abutment teeth, the improved ability to clean the proximal surfaces of the adjacent teeth (which decreases the risk of decay and periodontal disease), a decreased risk of cold or root contact sensitivity with a brush or scaler on the abutment teeth, improved esthetics, maintenance of bone in the edentulous site, psychological advantages (especially with congenitally missing teeth or the loss of a tooth after a crown restoration), and the decreased risk of abutment tooth loss from endodontic failure or caries (Box 16-10). These advantages are so significant to the health and periodontal condition of the adjacent teeth and maintenance of the arch form that the single-tooth implant has become the treatment of choice in most situations.
Box 16-10 Advantages of Single-Tooth Implants
CONTRAINDICATIONS AND LIMITATIONS OF POSTERIOR SINGLE-TOOTH IMPLANTS
Local contraindications that are unique to posterior single-tooth implants (Table 16-1) and favor an FPD include inadequate bone volume, inadequate intratooth space, and observable mobility of the adjacent teeth. Grafting may modify inadequate bone volume, either in height or width. Bone grafting for additional height when the adjacent teeth have lost bone is not as predictable as implant insertion and healing, regardless of the technique used. Therefore an FPD may still be the treatment of choice.
Table 16-1 Contraindications for a Posterior Single-Tooth Implant versus Indications for a Posterior Three-Unit FPD
| LOCAL CONTRAINDICATIONS FOR A POSTERIOR SINGLE-TOOTH IMPLANT | INDICATIONS FOR A POSTERIOR THREE-UNIT FPD |
|---|---|
FPD, Fixed partial denture.
The mesiodistal posterior space should be at least 6.5 mm or greater. Smaller intratooth spaces should be restored with an FPD or two adjacent crowns that are overcontoured. Flossing is easier between unsplinted crowns than for a fixed prosthesis, and the cost is reduced. If the space is out of the esthetic zone, then the clinician may consider not replacing the tooth, if the adjacent teeth are not at risk of tipping or extrusion because of the occlusal relationship of the opposing teeth.
Transitional Restorations
An absence of transitional posterior tooth replacement is the most frequent situation during bone augmentation and implant healing in a nonesthetic region, such as the mandibular posterior aspect of the mouth. Although the occlusion and adjacent teeth may change during the 4-month healing period, rarely is this a cause of further restoration in the region (Figure 16-9).
IMPLANT BODY SELECTION
The implant body for a posterior single-tooth implant should include specific features to reduce complications. The most common problem associated with a single tooth is abutment screw loosening.35,38–42,47–55 Crest module and abutment connection designs that decrease forces to the abutment screw are therefore indicated. The implant must have an antirotational feature (i.e., external or internal hex). The greater the height or depth of the antirotational feature, the less force transmitted to the abutment screw. Accuracy of component fit and abutment screw design, as well as the number of threads, are other critical features.56–58
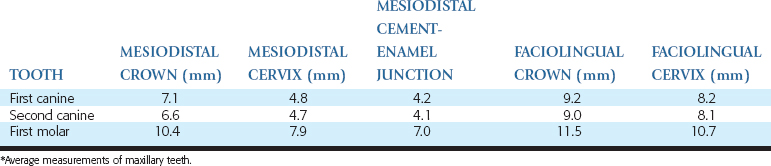
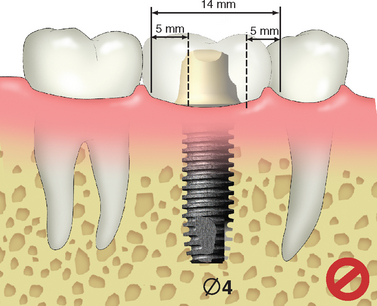
The ideal diameter of a single-tooth implant is dependent on the mesiodistal dimension of the missing tooth and the buccolingual dimension of the implant site (Table 16-2). An angular defect may develop around the abutment-body connection measuring 1.0 to 1.4 mm in width. As a result, when the implant is placed closer than this dimension to an adjacent tooth, the vertical, angular defect dimension may cause bone loss on the tooth. When the implant has facial bone thickness less than 1.4 mm, bone loss may result and implant failures occur more frequently.59 The horizontal bone loss around the implant will cause an increase in probing depths or an increased risk of soft tissue shrinkage. These may affect the bacterial flora or cervical esthetics of the soft tissue drape. This may be why gingival recession around wide-diameter implants have been noted to be greater than with a standard diameter.60,61 As a consequence, the ideal implant diameter is 1.5 to 2.0 mm from an adjacent tooth and 1.5 mm from the lateral width of the ridge. Therefore the ideal implant diameter in the intratooth posterior region should be at least 3 mm less than the mesiodistal dimension of the missing tooth (from cement-enamel junction [CEJ] to CEJ) and 3 mm narrower than the buccolingual dimension of bone. As general rule, the molar implant should be larger in diameter than a premolar implant (Figure 16-10).
PREMOLAR IMPLANT REPLACEMENT
The most ideal posterior tooth to replace with an implant is the first premolar in either arch (Figure 16-11). When used as an abutment for a three-unit FPD, the canine is at an increased risk of material fracture or uncementation (because of the lateral forces applied) and is often more difficult to restore to its original appearance than are other anterior or posterior teeth. The vertical available bone is usually greater in the first premolar locations than in any other posterior tooth positions. In the maxilla, it is almost always anterior or below the maxillary sinus (or both), and the mandibular first premolar is almost always anterior to the mental foramen and associated mandibular neurovascular complex. The bone trajectory for implant insertion is more favorable in the mandibular first premolar than for any other tooth in the arch.
To ensure a proper esthetic result and to avoid the need for a crown with a ridge lap, the implant body is often positioned similar to an anterior implant, under the buccal cusp. The slight buccal implant placement improves the cervical emergence profile of the maxillary premolar crown (Figure 16-12). The natural premolar tooth root is 4.2 mm in diameter on average at a distance of 2 mm below the CEJ. As a consequence, the most common implant diameter is about 4 mm at the crest module. This also provides approximately 1.5 mm of bone on the proximal surfaces adjacent to the natural teeth when the mesiodistal space is 7 mm or greater. However, when the mesiodistal dimension is only 6.5 mm, a 3.5-mm implant is suggested.
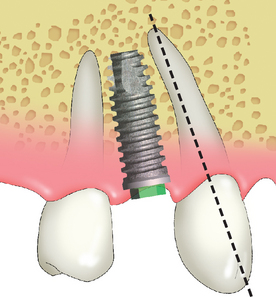
The maxillary canine root is often angled 11 degrees distally and presents a distal curve 32% of the time, which may extend over the shorter root of the maxillary first premolar. The implant body is often longer than the natural tooth root. The surgeon may inadvertently place the implant parallel to the second premolar and, consequently, into the natural canine root. This may not only result in endodontic therapy of the canine but also may cause root fracture and loss of the tooth. Therefore in the maxillary first premolar region, care must be taken to evaluate the canine angulation and vertical height limitation. The first premolar implant may need to be placed parallel to the canine root, and a shorter implant than is considered ideal may be required. A tapered implant body at the apical one third may also be of benefit (Figure 16-13).
FIRST-MOLAR IMPLANT REPLACEMENT
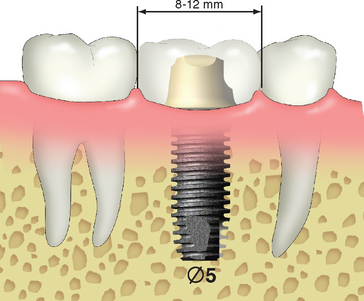
The first molar is one of the teeth most frequently lost in a posterior segment. Its mesiodistal dimension usually ranges from 8 to 12 mm, depending on the original tooth size and the amount of mesial drift of the second molar before implant placement. When one 4-mm-diameter implant is placed to support a crown with a mesiodistal dimension of 12 mm, this may create a 4- to 5-mm cantilever on the marginal ridges of the crown (Figure 16-14). The magnified occlusal forces (especially important in parafunction) may cause bone loss, which may complicate home care, increase abutment screw loosening, and increase abutment or implant failure because of overload.61,62 Sullivan62 reported a 14% implant fracture rate for single molars fabricated on standard-diameter Nobel Biocare implants and concluded that this is not a viable treatment. Rangert et al.63 reported overload-induced bone resorption appeared to precede implant fracture in a significant number of single-molar implant restorations. When possible, a larger-diameter implant should be inserted to enhance the mechanical properties of the implant system through increased surface area, stronger resistance to component fracture, increased abutment stability, and enhanced emergence profile for the crown64–67 (Figure 16-15).
When the mesiodistal dimension of the missing tooth is 8 to 12 mm, with a buccolingual width greater than 7 mm, a 5- to 6-mm-diameter implant body is suggested (Figure 16-16). Langer et al.64 also recommended the use of wide-diameter implants in bone of poor quality or for the immediate replacement of failed implants. The larger-diameter implant does not require as long an implant, which is also a benefit because of the reduced posterior vertical bone height due to anatomical limitations and landmarks present, such as the maxillary sinus or mandibular canal.51,64,68
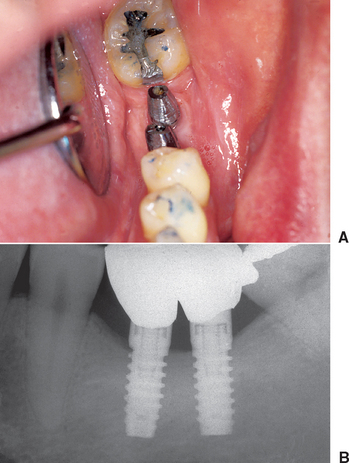
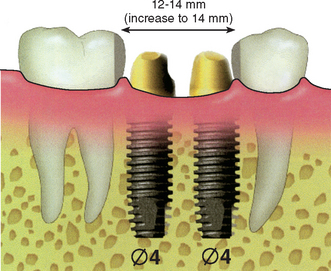
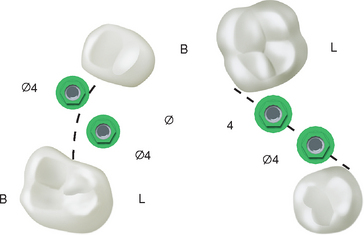
When the mesiodistal dimension is 14 mm or greater, two 4-mm-diameter implants should be considered to restore the region. When two implants replace the molar region, the mesiodistal offset loads to the prosthesis can be eliminated. The total surface area of support is greater for the two implants compared with the surface area provided by one larger-diameter implant. In addition, the two regular-size implants provide more stress reduction than just one larger-diameter implant, which in turn reduces the incidence of abutment screw loosening. In 1996, Bahat et al.51 reported on the results of various implant numbers and size selection. The overall failure rate was 1.2%, with the two 5-mm implants having 100% success. In the same year, Balshi et al.52,53 compared the use of one implant and two implants to replace a single molar. The 3-year cumulative success rate was 99%. Prosthesis mobility and screw loosening were the most common complications for the one-implant group (48%); this complication rate was reduced to 8% in the two-implant group. An in vitro study compared screw loosening of one wide-diameter versus two standard-diameter implants. Bakaeen et al.69 also concluded that the one wide-diameter implant had greater screw loosening. In a finite element analysis of three different implant-supported molar crown design, Geramy and Morgano70 showed a 50% decrease in mesiodistal and buccolingual stress between a 5-mm- and standard-diameter implants. The double implant design had the least stress of all. Therefore whenever possible, two implants should be used to replace a larger single-molar space to reduce cantilever loads and abutment screw loosening (Figure 16-17).
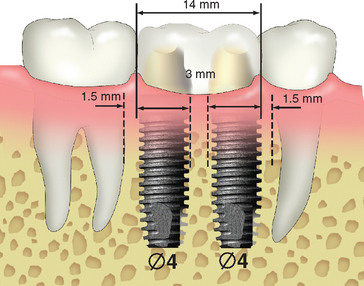
When the posterior space is 14 mm or greater, the largest implant diameter for the two implants may be calculated by subtracting 6 mm (1.5 mm from each tooth for soft tissue and surgical risk, and 3 mm between the implants) from the intratooth distance and dividing by 2, for a total of 5 mm for each implant (Figure 16-18).
The diameter is the crest module dimension, which is often 0.35 mm greater than the implant body dimension (i.e., Nobel Biocare, SteriOss, 3-I, LifeCore). The two implants should be 3 mm apart, because crestal bone loss around each implant may occur. The width of the crestal defect is usually less than 1.5 mm. Therefore the two adjacent implants 3 mm or more apart will not convert the angular defect to a horizontal defect that may increase sulcus depths and cause a loss of papilla height.71 When possible, two regular-size or one regular- and one larger-diameter implant are suggested when replacing molars. The natural molars have 200% more root surface area compared with premolars; therefore the implant support in a molar region should be greater than in the premolar position.
| MESIODISTAL DIMENSION (mm) | IMPLANT DIAMETER |
|---|---|
| 7 | 4 mm |
| 8 to 12 | 5 mm |
| 12 to 14 | Gain additional space, then place 2 × 4 mm |
| ≥14 |
ESTHETIC MAXILLARY ANTERIOR TOOTH REPLACEMENT
In 1994 the number of implants used in the United States averaged fewer than two per patient. This was a consequence of most dentists using implant treatments for a single-tooth implant,72 small-span FPDs with two implants, and two implant overdentures. From 1990 to 1999, a threefold increase occurred in the number of single-tooth implants placed by a practitioner, as well as an increase in the overall implant market.73 Single-tooth impl/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses